Putting Community Health Front and Center in Massachusetts
Promotoras survey overlooked populations to gather critical health information
Posted on Feb 28, 2023
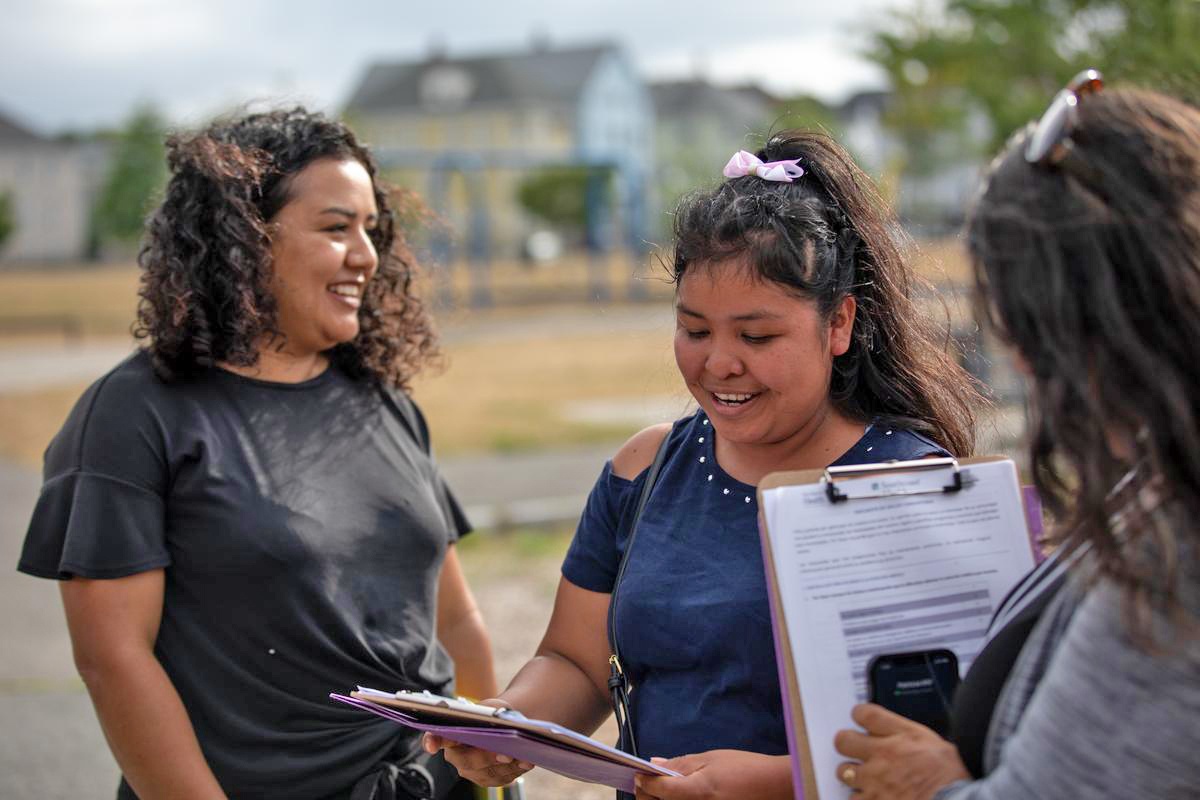
When health worker Alicia Cortez set out to evaluate community needs in New Bedford, Mass., she was resolute that her own community should be heard.
So, Cortez, working with a team of 11 other community health workers, known as the promotoras victoriosas, showed up at the fisheries and markets, shopping areas and public spaces where she knew people of Guatemalan descent gathered. This new effort, backed with training by the New Bedford Health Department and the U.S. division of Partners In Health, worked.
“We know where people walk around and at what times, so we would just stop them and ask them,” said Cortez, who was born in Guatemala and has lived in the U.S. since she was 8 years old. “We’d tell them we want to know how they feel about the health department, and ask if they know all the services available. … We said if they’d answer a few questions, it would open up doors to their health.”
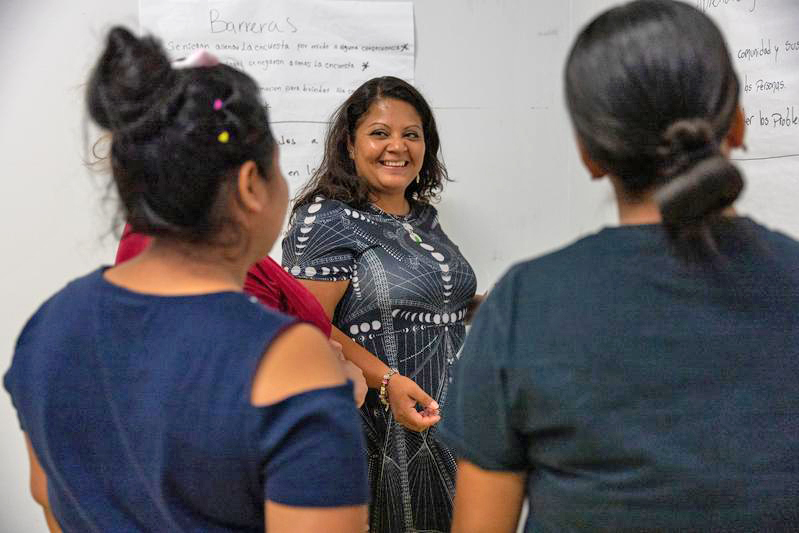
Barriers to Care
And open up they did. People cited an array of barriers to getting quality health care: inadequate transportation; no time off from work to see a doctor; a dearth of dental care; a lack of understanding from health officials when they had trouble understanding English-only materials; no insurance; fear of deportation; and cultural stigma surrounding illness.
In the end, the PIH-trained promotoras, working with SouthCoast Health and the local health department, gathered over 800 of the more than 1,200 surveys collected from people detailing their health needs, challenges, and concerns about the system. Two years earlier, a different health assessment team, that didn’t lean on the expertise of the promotoras, collected only 430 surveys.
Two-thirds of the recent survey respondents were Hispanic, women, and living with a median household income below $25,000. By comparison, in 2019, the vast majority of respondents were white, female, and highly educated.
Marlene Cerritos-Rivas, PIH’s health equity program manager in New Bedford, said it was meaningful that the latest survey included communities that were previously overlooked. “To have their voices included, that was very important, “ she said.
“For the health department, but also for the community to know that the government wanted their input, wanted to know about the barriers. It was a very empowering experience.”
The new data, which will be analyzed, verified, and ultimately used to inform future regional public health planning strategies, offers a deeper understanding of the demographic evolution of New Bedford.
A City of Immigrants
Located in southeastern Massachusetts, New Bedford is home to about 105,000 residents, including approximately 5,000-10,000 undocumented immigrants. Like many other cities with comparable demographics, New Bedford has been hit hard by health crises, including the COVID-19 pandemic, the opioid epidemic, and homelessness, among others. As a result, according to the health department, New Bedford’s Hispanic population and other marginalized groups suffer from disproportionately poor health outcomes.
To begin to address this, the health department hired three full-time outreach workers who provide services to community members in English, Spanish, Portuguese, and Cape Verdean Creole. And, in collaboration with PIH-US, the department provided training and employment to the promotoras in order to reach out to communities that had never before been asked for their opinion. This practice of hiring local community health workers to strengthen and broaden care is modeled off of PIH's work globally, where CHWs are a central component of every health care team.
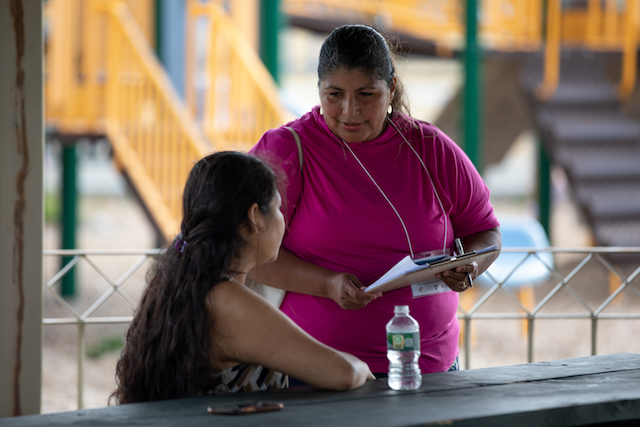
The PIH-New Bedford partnership started in late 2020, as PIH began responding to requests for technical support from regions across the United States slammed by COVID-19. In early 2021, PIH-US recruited, hired, and trained a five-person team embedded in the New Bedford Health Department. The team’s full-time epidemiologist, contact tracer, community liaison, health equity specialist, and senior team leader began supporting all aspects of the city’s COVID response, but are now pivoting to support the development of a stronger, more equitable regional health system.
“Our emergency response work in New Bedford has evolved into a longer term commitment to improving health equity,” said Katie Bollbach, executive director of PIH-US. “As we now work to address the underlying systemic issues that drove deeply inequitable COVID-19 outcomes, we’re deepening our partnerships in the city to ensure local expertise and experience are driving identification of new solutions to these long-standing challenges.”
A significant element of this strengthening involves gathering more input from people who are most affected by various health care policies and structures.
Gaining Trust
So, Cerritos-Rivas said, in the summer of 2022, the promotora training began. “They practiced with friends and family and then began reaching out to the broader community, going to public areas, festivals, church, and then to the streets, to places with heavy foot traffic by the Hispanic community.” The promotoras, she said, reflect that community: they are predominantly from Central America, notably Guatemala and El Salvador. Four of the health workers speak K’iche, a language indigenous to Guatemala. “We’d had a hard time reaching out to the K’iche community,” she said. “There was a lack of trust.”
Luisa Carina Raymundo, another promotora from Guatemala, said community members were motivated to speak to people familiar with their struggles and lived experience. “They do this because they believe that together we will be able to make changes and because they are tired of living in an oppressive system.”
Raymundo, who was raised by a single mother, and has lived in New Bedford for the past four years, said there is significant fear in these immigrant communities. “One of the things that worries me is knowing that there are families that experience domestic violence and knowing that there are many children who are growing up in an unsafe family environment,” she said. “Many people are scared because they do not feel safe on the streets, and others cannot feel safe at home because of alcohol abuse or other problems.”
Overall, the promotoras said, their goal is essentially to help people use the health care system to improve their daily lives.
All of the information from the surveys will inform a comprehensive health disparities data analysis, documenting the impact of race and ethnicity on health outcomes in New Bedford.
Based on this information, officials said, new recommendations on health policy and programming will emerge, “providing a blueprint to reduce, and ultimately eliminate, racially- and ethnically-driven health inequities.”
The vision, added Alicia Cortez, is “to send a powerful message…this job, the work is very powerful and we can save lives.”


