Toddlers Growing, Gaining with Help from Malawi Clinic
Posted on Nov 20, 2018
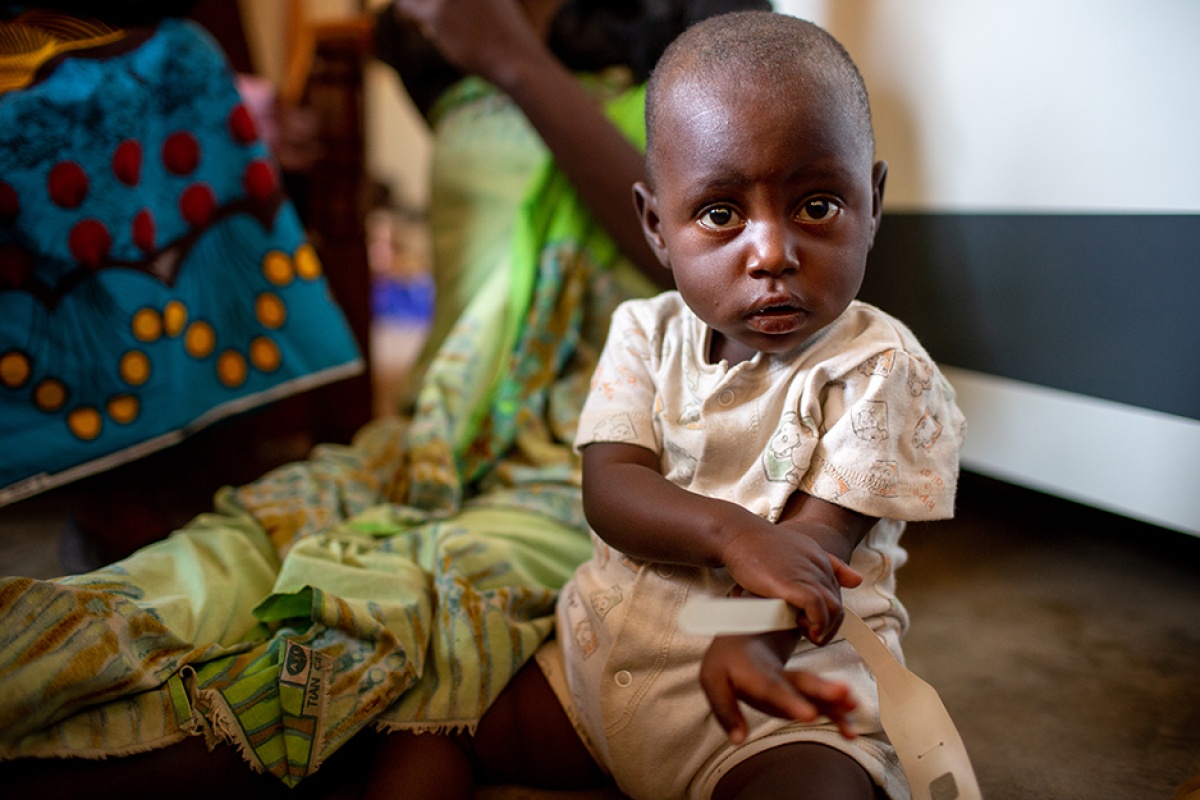
Violet McDonald has an expressive, thoughtful face that belies her age of just one year.
As several adults crowded around her in a small, noisy room at Matope Health Center in Neno District, Malawi, baby Violet sat on the floor in her onesie, quietly looked around and held a MUAC strip against her arm, as if she knew how to measure her own Mid-Upper Arm Circumference, a primary gauge of malnutrition in small children.
She actually might have. Lydia McDonald, 20, had been bringing her baby daughter to the Matope facility since late June, for regular checkups through the program known as CMAM, or Community Management of Acute Malnutrition. Violet’s weight had increased from 7 kilograms at her first visit to 7.9 kilograms at this visit, in early October. That equates to growing from about 15 pounds to 17.4 pounds.
It was a significant gain, but there was plenty of room to grow. CMAM facilitator Jessie Chizumo carefully recorded Violet’s health information in large paper files, and checked her weight on a chart that showed a corresponding amount of RUTF—ready-to-use therapeutic food, or nutritional meal supplements known locally as chiponde—that Violet would need for the week ahead.
For 2-year-old Stella Alfred, also in the CMAM clinic that morning, the number of needed meals was 23, or three-and-a-quarter RUTF packages per day. Chizumo explained the recommendation—one package in the morning, one for lunch, a snack, and one for dinner—to Stella’s mother, 27-year-old Jennifer Andrea.


Stella’s weight—at a full year older than Violet—was just 8.4 kilograms, or about 18.5 pounds. She cried throughout her checkup, as Andrea rocked her gently.
Violet and Stella are two of the 11 children enrolled in the CMAM clinic at Matope Health Center, which serves 11 nearby villages and is supported by Partners In Health. On this particular morning, an integrated chronic care clinic also was underway, with lines of people waiting for screenings, talking with staff or resting in the shade of a huge baobab tree. The malnutrition clinic was toward the rear of the health center, away from much of the bustle.
Known in Malawi as Abwenzi Pa Za Umoyo, PIH supports malnutrition care for more than 2,400 children younger than 5, across Neno District.
This was the hardest time of year for them and their families.
September and October are Malawi’s hottest months, known colloquially as “hunger season.” Riverbeds are dry, fields are dustbowls, the harvest is weeks in the past and new rains have not yet arrived. Dry heat turns bent, picked-bare cornstalks into crinkly brown matchsticks. For Neno District’s population of about 170,000, it’s a time of food scarcity and corresponding high prices for corn and other staples—especially this year, when many people around Neno cited a weak harvest.
Robert Jackson, supervisor for Matope’s community health workers, said the 115 CHWs based at the health center do all they can to screen every child for malnutrition, and refer children and parents to the CMAM clinic. It’s a busy job. Just nearby Tchenga Village, where McDonald lives with Violet, has more than 600 households.
But the need is vital.
“By screening all children at the household level through visits by community health workers, our goal is to catch malnutrition earlier and refer children quickly to treatment, to avoid hospitalization or significant illness,” said Emilia Connolly, chief medical officer for PIH in Malawi. “This will improve the health of children and families overall, thanks to the invaluable work by the community health workers—our foot soldiers.”


