Young Doctors Ensure Continuity of Care in Rural Mexico
Posted on Apr 14, 2015
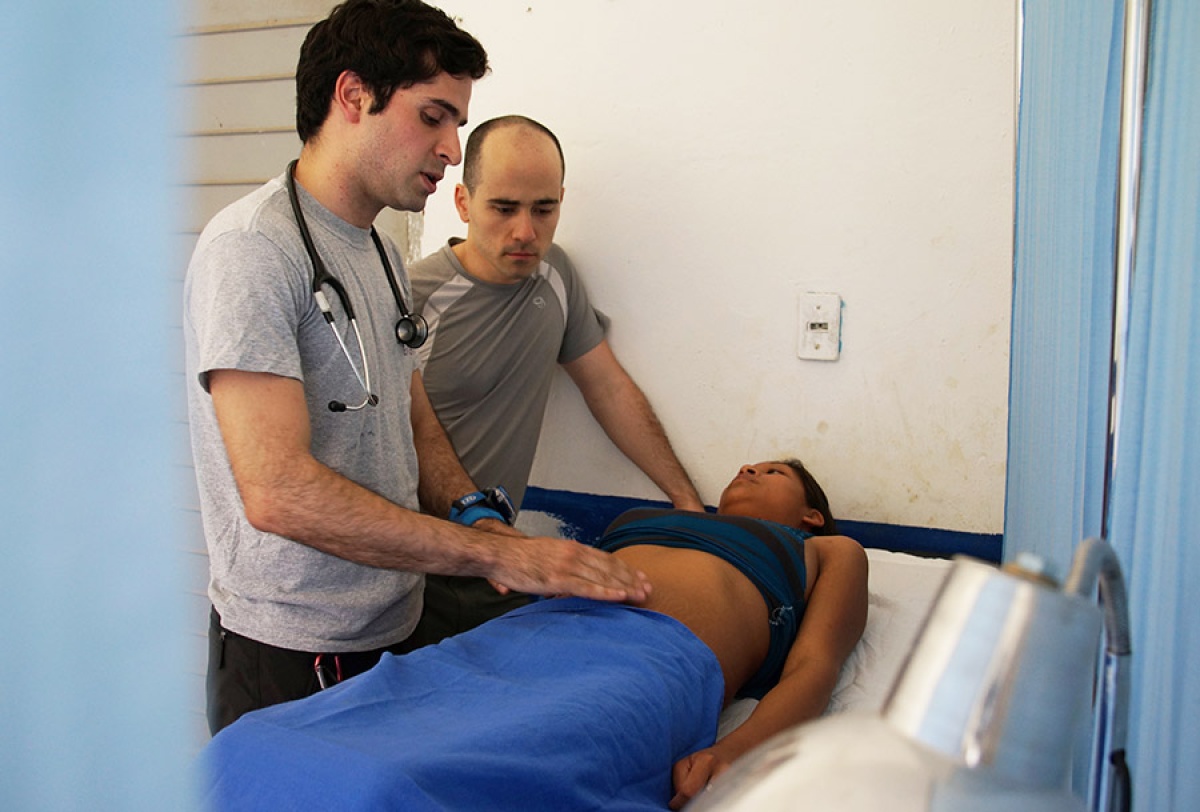
Dr. Eduardo Peters arrived in the town of Plan de la Libertad with a head full of knowledge, a good stock of medication, and a healthy helping of good will. While all were important in managing a public clinic in rural Chiapas with Compaňeros En Salud (CES), Partners In Health’s sister organization in Mexico, there was one thing he lacked: the community’s trust. That takes time to cultivate.
“Trust is definitely something you build over months,” said Peters, who recently completed his social service year and now works as CES’s public relations coordinator. He felt that trust grow with each office visit, successful treatment, and trip into the surrounding hillside when he checked on patients and shot the breeze. ”You are part of the community, you’re marginalized with them. You start getting into their homes, you take care of their kids, you cook with their wives and they laugh because you’re a guy” who cooks.
In these moments Peters was more than a doctor; he was a friend and neighbor. Yet he knew that after one year, he would be replaced by another first-year doctor—or pasante—who would have to earn trust all over again.
Since launching in 2012, CES has partnered with Mexico’s Ministry of Health to send seven generations of pasantes—25 young doctors in all—to rural, public clinics at 10 sites throughout Chiapas. Each transition requires a careful passing of the baton from one wave of doctors to the next. While CES staff facilitate this transition through introductions and regular site visits, outgoing pasantes smooth the path for their colleagues by remaining in the community for as many as four weeks to bring them up to speed on patients’ cases and help them adjust to life in a remote rural location.
A new home
Peters remembered vividly what it was like arriving in “Plan,” a bumpy three-hour ride from CES headquarters in Jaltenango through the Sierra Madre mountains. “I’m a city rat,” he said. “I’m used to seeing everything gray and concrete. You get to this beautiful green place full of mountains, and you see corn fields and coffee plantations”—the sources of most families’ income.
 |
|
|
Everything reminded him that he was a long way from home. “I remember my first few months,” Peters said. “There were days when I would wake up on a horrible mattress, under a mosquito net, and say, ‘What am I doing here?’ But it wasn’t regret. It was just surreal sometimes to wake up in the middle of a forest, in a teeny house, with bucket showers and no internet, and a terrible phone” shared by the entire community. (The phone operator announced over a public loudspeaker whenever a call was for him.) It wasn’t so much culture shock, he said, as getting used to a new way of life.
Dr. Gabriela Chalup, a CES clinic supervisor, accompanied Peters his first weeks in the community and showed him how to fill out government paperwork, introduced him to patients, and took him around to families’ homes. “It definitely makes a huge difference,” he said. “I would have gone there myself, I’m adaptable, but Gabi helped with the transition.”
The best year of medical service
Peters found well-stocked clinics in the community’s two villages—Plan Alta and Plan Baja. And he learned he’d have help four days a week from Rosa Huet Pale, a Tzotzil-speaking nurse who translated for indigenous Mayan families coming to work in Plan’s coffee fields.
Still, Peters’s transition wasn’t easy. The pasante before him had to leave four months early, and he saw the difference that absence made in the community. All of the chronic patients were “a mess,” he said. People with hypertension or diabetes weren’t taking their pills or had decided to change their own dosage. One patient developed glaucoma and went blind. The hardest thing for him to take was hearing that a six-year-old girl had died from diarrhea while the clinics sat empty.
“In 2015, it’s unacceptable,” he said. “It’s not frequent, but it’s such a preventable death.”
Peters never lacked work. Depending on the day, he could see anywhere from 14 to 34 patients. And while he was the community's primary care physician, he often dealt with issues fit for a dermatologist, cardiologist, pediatrician, or EMT. He got most chronic patients on a regular regimen of medication. He started at least one middle-aged man on treatment for TB after he’d been misdiagnosed with pneumonia. And he connected with a dermatologist, who brokered a deal with a drug company so that an 11-year-old boy suffering from disfiguring eczema could get a steady supply of free medication.
Whenever a particularly tough case presented itself, Peters knew he could call CES Clinical Director Dr. Patrick Elliott for guidance. Elliott and other CES mentors visited regularly to check on his progress and deliver supplies. And he and other pasantes traveled monthly to Jaltenango for three days of global health and social justice courses, all part of CES’s social service year program.
“Even though there was a lot of work,” Peters said, “it was by far the best experience of my medical training.”
A smooth transition
 |
|
|
When Dr. Rodrigo Bazúa arrived to replace him in February, Peters was prepared. He had Bazúa shadow him for two weeks as they held clinic and made home visits, all while providing him with cultural tips, a quick community history, and introductions to allies. He even prepared a 10-page document detailing regular patients’ cases so that no information was lost in the transition. And that was in addition to the electronic medical records that are kept for each CES patient.
“It’s nice to know that you’re helping out another pasante and making sure he knows all those details you know,” Peters said.
Like Peters, all pasantes have agreed to stay an extra two weeks after their year of service to help colleagues adapt to their communities.
"This is incredibly rare since most pasantes in other parts of Mexico eagerly await their last day of social service to head back home, to vacation, or to a new job," Elliott said. "But for our pasantes, the largest concern they had was to make sure that their patients received the best care possible. Without an active and personal hand-off, this simply hadn't been possible. ... I am incredibly proud of the way our clinicans have responded to this call."
For his part, Bazúa felt little culture shock when he took over the reins from Peters. “I think Eduardo did a great job in making a smooth transition, and I feel great,” he said. Two months in, he’s beginning to get a fuller picture of Plan and its people. He’s surprised by its diversity (he’d never expected to find such a mix of Catholics, Adventists, and Jehovah’s Witnesses in rural Chiapas) and is learning regional slang for body parts and ailments. He wants to get more chronic patients on treatment regimens and to better understand why so many of his patients endure bouts of asthma and allergies, which he’d thought were common only in wealthier communities.
By the end of his social service year, Bazúa hopes “to be absolutely capable of seeing any disease that is treatable in primary care and treating patients well.” And it would be nice to know, he said, that “the community is satisfied with their doctor.”


