Our Work in Sierra Leone
Sierra Leone previously had one of the highest maternal mortality rates in the world—an injustice that the Ministry of Health and PIH are working tirelessly to address. Despite significant improvements, roughly 1 in 74 women in Sierra Leone face a lifetime risk of dying in childbirth. Extreme poverty prevents most families from accessing health care, and often the care they need isn’t available, given the country’s severe shortage of trained clinicians, health infrastructure, and medical supplies.
West Africa’s historic Ebola outbreak intensified all of these problems and further eroded Sierra Leone’s already weak health system. So when the government requested PIH’s help to end the outbreak, we agreed—and committed to staying long past Ebola, to build and strengthen the health system. Today, in partnership with the government, PIH directly supports 11 health facilities and works across eight districts in an effort to build a health system that protects every Sierra Leonean’s right to health, especially those most vulnerable to sickness and injustice.
Our Impact
73%
134%
49%
Innovations in Care
In Kono District, a rural eastern region of 620,000 people, famous for its diamond mines and as the epicenter of Sierra Leone’s decade-long civil war, PIH is investing in every level of the health system. We operate Wellbody Clinic; support Koidu Government Hospital (KGH), Kono’s only hospital; and partner with smaller public primary health clinics throughout the district.
Our ongoing investments alongside the government in clinical training, infrastructure, and supply chain have equipped clinicians, pharmacists, and lab techs with what they need to deliver lifesaving care
PIH employs a network of community health workers (CHWs) who link patients to health facilities and social support. CHWs maintain close relationships with patients and their families, making regular home visits to check on patients’ health and well-being, refer and accompany them to care, and connect them with social support from PIH, such as food packages, housing repairs, transportation, and educational opportunities like adult literacy courses.
Wellbody Clinic is our model primary health clinic, providing expert care—from vaccinations, to malnutrition care, to HIV treatment and counseling.
The clinic is setting new standards for health care, not just in Kono, but nationally. Since 2016, only one maternal death was registered, thanks to the mentorship of maternity staff and maternal waiting homes, facilities where women with high-risk pregnancies can stay for 24-hour monitoring ahead of their due date. The electronic medical record system—the first in the country—ensures clinicians quick access to comprehensive, up-to-date medical histories, in order to better inform patient care. At KGH—the only secondary care facility in Kono—we’ve introduced resources as basic as 24-hour electricity and running water, to as advanced as oxygen production and a functioning blood bank.
We employ the district’s only specialized OB/GYN and pediatrician. We’ve opened an emergency room and special care baby unit, established chronic disease care, and made lifesaving C-sections and other surgeries available 24 hours a day. And we maintain a steady flow of vital medical supplies and medications to ensure quality care for any number of health issues—from diabetes, to tuberculosis, to obstructed labor.
In a bold step toward ending preventable maternal deaths, we are opening The Paul E. Farmer Maternal Center of Excellence (MCOE) in 2026, a brand-new clinical facility. Situated on the same campus as KGH in rural Kono District, this teaching and referral facility will dramatically expand the clinical space, increasing its current 48-bed maternal ward and special care baby unit to a 120-bed center that includes a cutting-edge neonatal intensive care unit.
We are supporting the Ministry of Health to strengthen the quality of essential health services in five districts outside Kono. By leveraging the proven hub-and-spoke service delivery model successfully, implemented in Kono District, we are applying lessons learned and best practices to 179 more health facilities across Sierra Leone. Through this effort, we aim to increase the use of facility-based services and improve maternal and child health care by supporting peripheral health units in rural districts—that patients, no matter where they live, receive the care they need and deserve.
The capital city, Freetown, is home to the country’s only specialized, dedicated hospitals for tuberculosis and mental health care: Lakka Government Hospital and Sierra Leone Psychiatric Teaching Hospital (SLPTH).
At Lakka, we’ve worked with the National TB Program to introduce never-before-available care for multidrug-resistant tuberculosis, are renovating hospital infrastructure to make it more comfortable for patients, have introduced new clinical capacities like a critical care unit, and provide social support, like food packages and transportation stipends, to ensure that patients can adhere to treatment and attend their appointments.
Today, the treatment success rate at the hospital is far above the global average for multidrug-resistant TB.
At SLPTH, we have transformed the facility into a hub for high-quality mental health care in partnership with the Ministry of Health. This facility—the oldest psychiatric hospital in sub-Saharan Africa—received formal five-year accreditation by the West African College of Physicians in 2022 to host the country's first psychiatric residency program. With this authorization, Sierra Leone began training its own psychiatrists for the first time, while strengthening the capacity of other health professionals in mental health care delivery.
Sierra Leone Videos
Latest Sierra Leone Stories

PIH Sierra Leone’s Isata Dumbuya Named to TIME Women of the Year List
A Global Honor for Local LeadershipPartners In Health (PIH) Sierra Leone’s Isata Dumbuya has been named to TIME’s annual Women of the Year list, recog ...
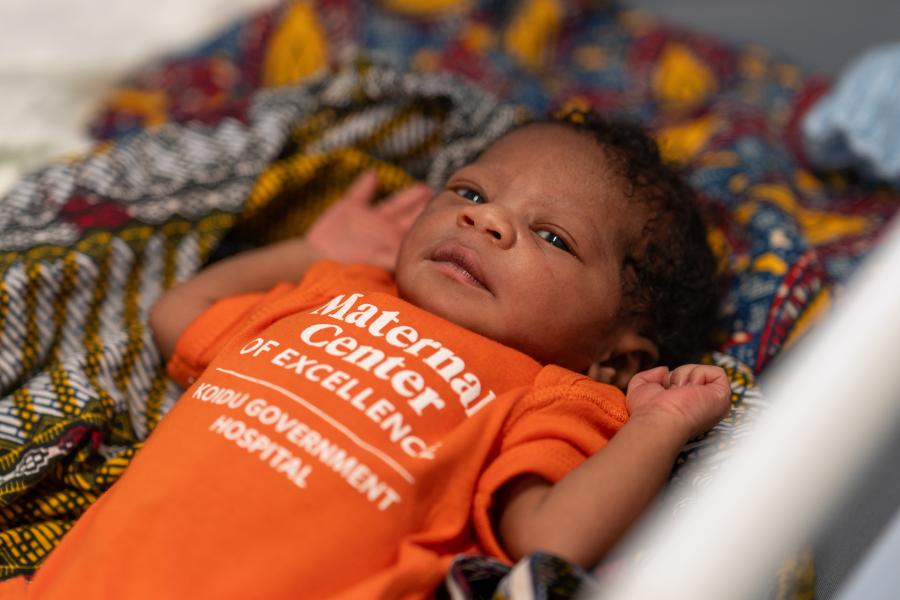
Opening Day at the Maternal Center of Excellence in Sierra Leone
On February 14, 2026, a warm breeze swept over Koidu Town in Kono District, Sierra Leone, as the sun rose over the Paul E. Farmer Maternal Center of E ...

9 Initiatives Keeping Paul Farmer’s Name and Legacy Alive
On February 14, the longtime vision of the Paul E. Farmer Maternal Center of Excellence will become reality, as the doors open to its first patients. ...

