“All Possible Care”: The Strides and Limits of Emergency Care in Sierra Leone
Luck and a team of determined clinicians saved James Fatoma’s life
Posted on Jul 27, 2022

James Fatoma moved to Kono District, Sierra Leone, when he was in high school—and from his teens through his early 30s, had only been to the doctor once.
That checkup was five or six years ago, when, sick with a fever and headache, he opted to go to a private clinic in Kono, where they diagnosed and treated him for malaria. It was an expensive visit—but one Fatoma said he had much more faith in than going to Kono’s public hospital, Koidu Government Hospital (KGH).
“KGH was cheaper,” he said. “But the quality of services was poor, so people didn’t go.”
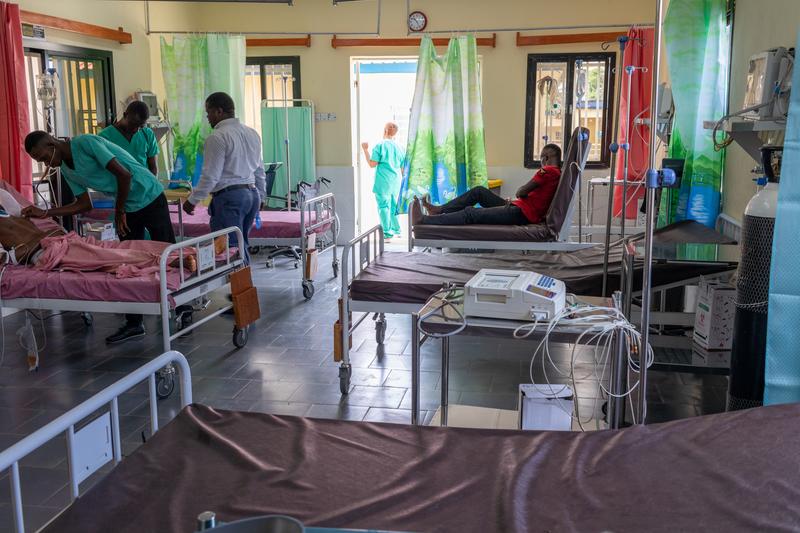
That changed in early 2019, on a day that quickly turned from typical to, in Fatoma’s words, “very scary.” At his job as a computer specialist, Fatoma fainted, and then that night at home began vomiting blood. Friends rushed him to KGH, where he was admitted to the emergency room—a department that had only recently opened thanks to Partners In Health’s (PIH) support of the hospital, five years after PIH began working in Sierra Leone.
It's also thanks to PIH’s investments in the hospital’s staff, stuff, and systems—from its team of nurses to its blood bank—that Fatoma survived through the night, even despite massive blood loss.
“There was a quick assessment [of Fatoma’s condition] and there was a very rapid response from the emergency team, the surgical team, and the blood bank,” said Dr. Marta Patiño, PIH’s internist at KGH who led Fatoma’s care. “We were dealing with life and death for two or three hours until he was stable.”
That stability didn’t last long—the next day, another bout of gastrointestinal bleeding necessitated that clinicians transfuse 18 units of blood. For three weeks, Fatoma remained in limbo in the emergency room, alternately stable and in critical condition, routinely saved by clinicians’ ingenuity.
“James was very, very close to dying on two occasions,” said Patiño. “He was lucky because we didn’t have an endoscopy, but we did multiple transfusions, kept his blood pressure stable through IV fluids, and did something that isn’t done anymore except in settings of poverty: we connected a nasogastric tube with the stomach and filled it with ice water, to stop the bleeding.”
“The information and the treatment”
“Let's assume this happened when a hospital like this was not around,” said Fatoma. “I would have been six feet below.”
Indeed, had Fatoma arrived at KGH five years earlier, when the hospital wasn’t resourced with clinicians trained in emergency medicine and supplies like IV lines, his chances of survival would have been slim. Still, as Patino notes, the hospital remained underequipped to provide truly proper care for Fatoma: Had he been a patient at a standard emergency department in the U.S. or Europe, clinicians would have immediately had the equipment and training to perform an endoscopy, a procedure that allows them to see inside a patient’s gastrointestinal tract to diagnose their illness and stop bleeding at the source.
“Endoscopy provides the information and the treatment,” Patiño explained. “If you ask any hospital in any wealthy country, nobody has any doubt that endoscopy saves lives.”
Without this essential procedure, clinicians were still able to diagnose Fatoma: Using ultrasound equipment and lab tests, they determined their patient was suffering from schistosomiasis, a parasitic infection commonly picked up in rivers in sub-Saharan Africa that, left untreated, can lead to liver cirrhosis. Growing up swimming in a nearby river with his friends, Fatoma likely had the infection for decades before it erupted in life-threateningly high blood pressure and subsequent bleeding.
Treatment was much more difficult to come by, contingent upon endoscopy services in capital city Freetown being up and running at the same time that Fatoma was stable enough to make the six-hour drive from Kono. In a testament to the volatility of health care services nationwide and the volatility of Fatoma’s health, the stars didn’t align for more than a year—during which Fatoma was in and out of the hospital with more episodes of intense bleeding.
With blood pressure medication, Fatoma had periods of stability—but daily life was a challenge.
“I was not able to eat much, I was weak and tired, I was not able to walk or even sit long, I had headaches,” Fatoma recalled, also noting that he sometimes had to miss months of work, an incredible stressor as the breadwinner for his fiancé, Dorcas, and two younger siblings.
Even so, Fatoma never lost hope. While he was still sick, Dorcas safely delivered their daughter at KGH. Fatoma named her Gifty—“because I got her during some amount of tragedy in my life.” And the care he continued to receive at the hospital kept him confident that one day his illness would subside.
“[The clinicians at KGH] applied a lot of effort,” he said. “They treated me with all possible care, as if I was a brother or sister to them. So I had 100% hope I would recover.”
Looking Ahead
That effort and optimism paid off when word arrived that a hospital in Freetown could perform an endoscopy for Fatoma, allowing clinicians to staunch all sources of bleeding as a complement to keeping his blood pressure down through medication. PIH provided transportation to and lodging in Freetown and paid for the $400 procedure.
Today, Fatoma is healthy—back at work and relishing returning home to his family each evening.
“When I get home, they are happy,” he said. “I play with Gifty, which brings such joy to my heart.”
Fatoma still goes to KGH regularly for checkups, and given the seriousness and permanence of liver cirrhosis, clinicians will continue to monitor his health closely for years to come. They say his case is emblematic of how far health care in Kono has come, but also the extent to which it still needs to be invested in and improved.
“James was lucky our treatment worked as we waited for months until we were able to find a facility [in Freetown] where we could send him,” Patiño said. “We have lost many patients in the emergency department to bleeding. Not all are able to survive, and some don’t even come in.”
Prevention—including education, screening, and early identification of schistosomiasis, as well as other conditions that cause liver problems, like hepatitis—is key, Patiño says. But so is providing timely, quality care to patients past the point of prevention.
“We need to be able to provide treatment,” Patiño continued. “We need to buy endoscopy equipment, train staff on it, maintain it. It is our responsibility to try and implement interventions that we think are going to make a change. And this is one of them.”


