Improved Maternal, Child Health Care Expands Across Sierra Leone
New initiative will transform rural health centers and reduce maternal and infant mortality
Posted on Dec 20, 2022

The maternal mortality rate is alarming in Sierra Leone, where 1 in 20 women face a lifetime risk of dying in pregnancy or childbirth. The mortality rate of infants and children under 5 are also among the highest globally: 122 deaths per 1,000 live births.
Many of these deaths are completely preventable when the right care is available. No woman should die from obstructed labor or a postpartum hemorrhage, nor should a child from diarrhea, pneumonia, or malaria.
In response to this injustice, Sierra Leone’s Ministry of Health and Sanitation (MOHS) is collaborating with Partners In Health (PIH) in the delivery of a pivotal project, the Quality Essential Health Services and Systems Support Project (QEHSSSP), which aims to improve care available at community health centers in rural districts so that patients, regardless of where they go, will receive the services they need—and deserve.
A partnership between the Government of Sierra Leone and PIH and funded by the World Bank, QEHSSSP is modeled after improvements made over the past several years at PIH-supported Wellbody Clinic and other facilities in Kono District. Patients have noticed the difference in quality of care, and each facility is now bustling with activity.
PIH leaders see huge potential in multiplying that impact more broadly.
“We should all see [this project] as a catalyst in changing and strengthening the health care system in Sierra Leone,” says Dr. Bailor Barrie, executive director of PIH Sierra Leone.
Project Goals
In December 2021, the World Bank approved a significant grant to support QEHSSSP, which will have a deep impact on maternal and child health services for 2 million people in Sierra Leone, a country of more than 8 million. The project focuses on 14 health facilities in five districts—Kailahun in the East, Bonthe in the South, Western Rural in the West, and Falaba and Tonkolili in the North—where the government of Sierra Leone will build resilient, efficient, and equitable health systems, with support from PIH. More specifically, the project aims to increase facility-based deliveries, access to basic nutrition services, and the number of pregnant women who receive a community health worker visit.
“This project will help very seriously to reduce maternal deaths,” says Michael Hallie Kendor, chiefdom speaker of Kissi Tongi in Kailahun District.

Key to success will be ensuring that each facility is equipped with essential health systems inputs. At PIH, we think of these investments as the five S’s:
- Staff: well-trained, qualified employees—such as nurses, midwives, community health workers, lab technicians, and more—in sufficient quantity to respond to patients’ needs
- Stuff: medication, diagnostic tools, medical equipment, furniture, and other resources to deliver services
- Space: safe and dignified facilities with the capacity to serve the community’s needs
- Systems: leadership and governance, information, and financial management systems for timely decision-making
- Social Support: meeting patients’ needs beyond medical care, including nutrition and social support
Improving Systems, Facilities
PIH has decades of experience in designing and delivering primary health care with government partners. In Sierra Leone, leaders see this as a hub-and-spoke model reflected in the work across Kono District, at one point a district with among the poorest health care options, having been at the center of the years-long civil war. There, PIH supports Koidu Government Hospital (KGH), which is the main district hospital for specialized care, where patients access everything from emergency services and surgeries to pediatric and chronic disease care.
At nearby Wellbody Clinic, a model primary care facility, patients access a variety of essential health services, such as prenatal and family planning appointments, malaria consultations, and malnutrition care. Complex cases, such as C-sections, are referred to the “hub” of KGH. Wellbody also serves as its own hub to which community health workers refer and accompany their neighbors from surrounding communities, and smaller “spoke” facilities. This continuous web of care flows back and forth, between hub and spoke, as patients’ needs are assessed, triaged, and met from community, to clinic, to hospital.
The model, introduced in 2014 when PIH began working in Sierra Leone, has proved to be successful. There is an increased flow of patients and from 2018-2021, there were about 55% more facility-based deliveries, 116% more lifesaving C-sections, and 44% more antenatal care visits across all PIH-supported facilities in the country. Most importantly, there has been a significant decline in maternal and infant mortality.
This success was recognized by the Ministry of Health and Sanitation (MOHS), which is why a hub-and-spoke model was prioritized for a new World Bank project that will support the ministry in creating new hubs across five districts. As with Wellbody Clinic in Kono District, to support MOHS, PIH will work to build health systems within the Jojoima, Bandajuma, and Buedu facilities in Kailahun District. In the other four districts, PIH will serve as an advisor to the MOHS, in an effort to replicate the hub-and-spoke model across 11 of the districts’ rural health centers.

Overcoming Challenges
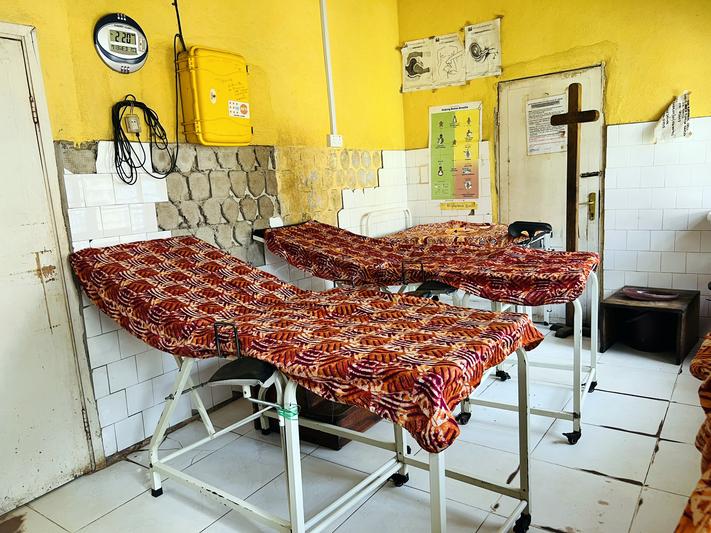
While each facility and location are unique, they uniformly need immediate infrastructure improvements. Nearly all of the 14 health facilities struggle with electricity, making it difficult to provide services at night or power lifesaving equipment. Some lack access to water, leaving them with sanitation systems that, among other things, make sterilizing instruments challenging.
“We are not able to handle some emergencies right now. We lack the necessary infrastructure,” says Ibrahim Allieu, a community health officer at Bandajuma Community Health Center in Kailahun District. “The well-being of our people in the community has been seriously impacted by this.”
Facilities lack well-stocked pharmacies, which leads to an inadequate drug supply and sometimes forces patients to buy questionable medication from outside vendors—or go without. Well-trained and sufficient staff is also in short supply. All of these and many other challenges have made it nearly impossible to deliver high-quality health services across the facilities.
Marian Sanjah, a midwife, juggles this reality every day at Jojoima Community Health Center in Kailahun District. “Our labor room is out of space and we struggle to get water at the facility,” Sanjah says. “Even though we have a solar-powered generator, we struggle with electricity. We experience frequent power cuts.”
“We use our phone lights or rechargeable flashlights to deliver [babies] at night,” she adds. “We are constrained and find it difficult to do our work. Delivering shouldn’t be done in the dark.”
Early Signs of Progress
PIH Sierra Leone staff and government partners have assessed all public clinics across the five districts to determine short- and long-term needs. Soon, repairs and construction will begin, medications will arrive to fill bare pharmacy shelves, and staff will receive training on new diagnostic testing that will ultimately improve the quality and variety of care available to patients in rural communities.
The work will be similar to what has already taken place at the health center in Gandorhun in Kono District. The remote facility shines with a fresh coat of blue and white paint. Water and electricity are now available 24 hours a day. And lab and pharmacy staff prepare their renovated and stocked spaces for what will inevitably be a steady flow of patients.

Several hours further along a rutted dirt road, a large, modern facility rises within a walled compound up the hill from the Jojoima Community Health Center. The facility, built by the MOHS with support from the World Bank, will serve as a referral center for the surrounding region and specialize in maternal and newborn care, but will also be home to pediatric care and other essential health services.
Touring the grounds on a recent September afternoon, Barrie envisions a future maternal waiting home at the site of the current health center and points to where the pharmacy, laboratory, kitchen, and laundry facilities will be, ideally, with a March 2023 opening. PIH is helping partners develop operational plans for the impressive facility, learning from work done in Kono District.
Meanwhile, back at Bandajuma Community Health Center, Allieu surveys the humble facility where he and other clinicians do what they can to deliver care without access to running water, electricity, and sufficient stock of essential medications. He has seen the work MOHS and PIH Sierra Leone have done together in neighboring communities, and he has hope.
“I believe with this intervention, some of these challenges will be addressed,” says Barrie.


