Malaria Cases Rising in Malawi as Peak Season Nears
Posted on Nov 8, 2018
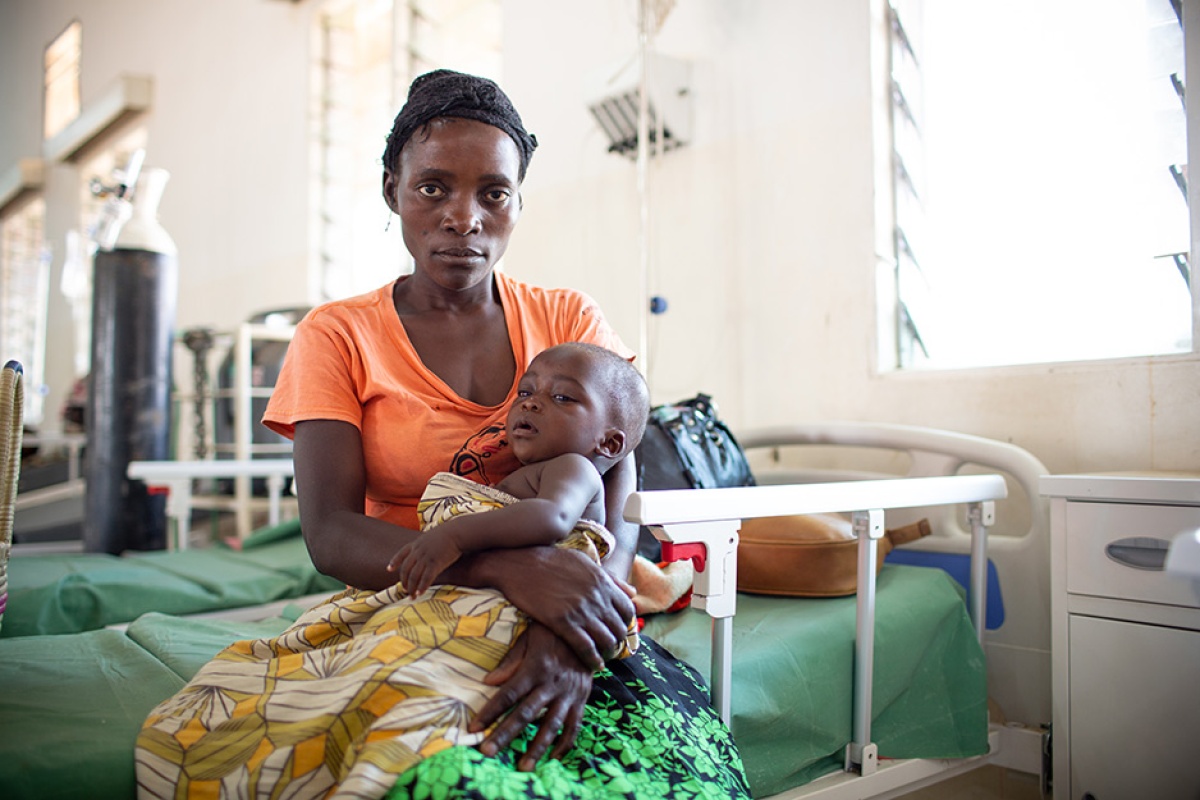
Photos by Zack DeClerck / Partners In Health
Flora and Thomas Tigone said they knew something wasn’t right when their 7-month-old son, Chisomo, suddenly became much less playful than usual.
Their worries increased when Chisomo grew feverish, and began vomiting and breathing heavily. It was a Monday in late September, in Luwani Village of Neno District, Malawi. Chisomo is the youngest of the parents’ six children. Just a month before, their second-youngest, a 7-year-old, had contracted and recovered from malaria.
Malaria is a mosquito-borne illness that can cause fevers, chills, muscle aches and fatigue. If left untreated, symptoms can escalate to nausea, vomiting, kidney failure, seizures, coma and death.
If malaria was the case again—and this time, with an infant—Flora and Thomas knew treatment would have to start quickly, to prevent complications. They brought Chisomo to Lisungwi Community Hospital at 5 a.m. the next morning.
Lisungwi is one of two hospitals that Partners In Health supports in Neno District. PIH, known locally as Abwenzi Pa Za Umoyo, has worked in Neno since 2007 and also supports 12 health centers there. The rural district borders Mozambique and is home to about 170,000 people.
Malaria is one of the most consistent, severe diseases afflicting the population, and Neno health workers are concerned about the peak season, now just weeks away. During the dry season, from May to September, PIH and Ministry of Health staff conduct about 17,500 malaria tests a month across Neno’s 14 PIH-supported health facilities.
But that number rises to about 30,000 tests a month—equating to nearly one-fifth of Neno’s entire population—in the rainy months from January to April, breeding time for mosquitos.
About 55 percent of malaria tests across Neno District show a positive result—meaning, positive for malaria, not for the patient. Subsequent treatment and care can place a heavy load on PIH and Ministry of Health staff in hospitals, health centers, and communities.
“To cope with the uptick in demand mostly requires more health care workers—medical assistants, nurses, clinical officers, and physicians—to diagnose and treat patients effectively,” said Emilia Connolly, chief medical officer for PIH in Malawi. “But the need also is great for rapid malaria tests, reagents for lab testing, blood transfusions, medications for malaria and its complications, and other hospital supplies.”
Lisungwi Community Hospital, and the Tigones’ home in Luwani, sit on parched flatlands that formed broad, paintbrush swaths of brown and yellow in late September. Grassfires seemed likely. Even the cooler, breezier mountainsides were dotted with smoke plumes, as farmers used controlled burns to clear land ahead of the coming rainy season.
But the rains had not yet arrived, and dry heat remained dominant. Thirsty, malaria-bearing mosquitos were seeking bites everywhere they could.
“Each and every day,” said Audings Winga, a Ministry of Health nurse at Lisungwi, describing the frequency of malaria-related visits at the hospital.
Fifty to 70 a day, to be more specific. That’s the daily amount of malaria tests cited by Allan Chimpeni, a Ministry of Health lab scientist at Lisungwi who works down the hall from the ward where Winga cared for little Chisomo, as Flora and Thomas stood by.
Chimpeni did Chisomo’s malaria test that morning. Malaria tests take about five minutes, he said, and require a blood sample placed on a small test strip.
The entire lab team at Lisungwi consists of Chimpeni and three technicians: Davie Chabwera, Yohane Ngwira, and Cidreck Murameya. In addition to malaria tests, their work includes blood counts, urine analysis, parasitology, tuberculosis screening, and more.

“The workload is very high here,” Chimpeni said.
It will soon get even higher. When the rainy season arrives in December, he expects the number of daily malaria tests to double.
“Severe malaria can happen any time of the year, but we see it much more in the rainy season, with more cases overall,” Connolly said.
Children are hit especially hard.
“I would say, on average, the number of children admitted to the hospital triples during the rainy season, mostly for malaria,” Connolly said.
On this September morning, the results of Chisomo’s test confirmed his parents’ fears. Despite the fact that they had placed a mosquito net around his bed, the 7-month-old’s diagnosis was severe malaria.
Winga quickly put Chisomo on medication, initially through an IV. By early afternoon, about eight hours after the family had arrived at the hospital, Chisomo was quietly breastfeeding, appearing much healthier and acting happier.
Relief was evident on the faces of Flora and Thomas, who sat next to each other on a hospital bed while holding Chisomo. Thomas, 45, is a bricklayer who has lived in Luwani all his life. The community is about a 10-minute drive from Lisungwi Community Hospital. Flora, 37, was born in Blantyre, Malawi’s commercial center and second-largest city, and sells vegetables in a local market.
They planned to stay at the hospital overnight with Chisomo, in case any complications arose.
Winga said Chisomo should be healthy the following morning. His free treatment would continue for four days, with a dose every 12 hours. Chisomo was just large enough to take pills orally, Winga said, so the initial IV would not be needed again.
The Lisungwi staff that screened, diagnosed and treated him so quickly had great news to confirm the next day: Chisomo, indeed, had been discharged in good health, and his parents had brought him home.



