PIH Shares PPE Conservation Strategies Amid Local, Global Shortages
Posted on Apr 9, 2020
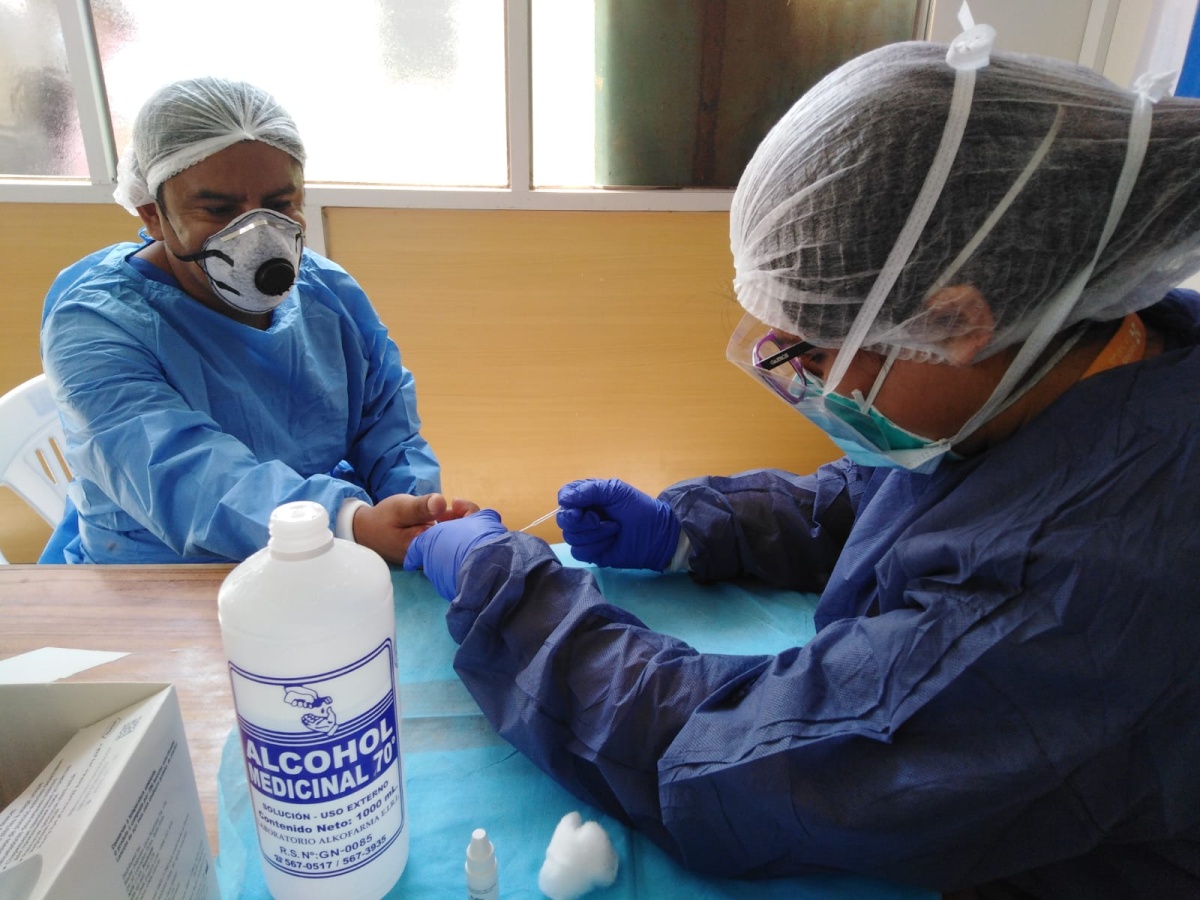
The first thing Cory McMahon will tell you is that shortages of personal protective equipment (PPE) for caregivers responding to COVID-19—and the conservation strategies that are emerging as a result—are not situations that anyone would hope for.
“I think my hope instead would be that we have enough PPE and don’t have to do something like this,” said McMahon, director of nursing and midwifery for Partners In Health (PIH). “These are not ideal situations for anyone.”
As hospitals and health facilities in Boston, across the U.S., and around the world are handling surges of COVID-19 patients while facing critical shortages of PPE—the vital masks, gowns, gloves, and eye protection needed by frontline caregivers—medical staff are making difficult decisions and doing all they can to ensure safety while providing high-quality care.
"Our nurses and doctors are always innovating to provide the best patient care possible," McMahon said. "This situation has forced everyone to develop creative solutions to ensure the safety of our health care workers."
To support those efforts, PIH is sharing the strategies and guidelines that clinical staff and colleagues are developing during the COVID-19 response. Staff will post the guidelines at PIH-supported hospitals and health facilities in the 11 countries where PIH works, and make them available for health organizations anywhere. The guidelines include PPE recommendations from the World Health Organization (WHO), the Centers for Disease Control and Prevention (CDC), and from local hospitals in Boston, where several PIH staff and colleagues are working and providing care for COVID-19 patients. These clinicians have already had to improvise and innovate with PPE to ensure the safety of caregivers.
McMahon said the pandemic’s impacts are unprecedented.
“The level of patients that we’re seeing at one time is not something that we’re used to absorbing, at a global level,” McMahon said. “What we’re seeing locally, whether it’s Boston or New York right now, that is going to be the same thing for us, in the countries where PIH works, if we’re not able to stop the spread. And possibly even more so, because they have less capacity to absorb” surges of patient numbers.”
McMahon added that hospitals everywhere already were functioning at capacity, in terms of both staffing and equipment, before COVID-19 began to spread.
“So it’s not like there is extra capacity waiting in the wings for this kind of pandemic,” she said. “Because of that, hospitals everywhere have started to think about their strategies, in order to absorb this.”
Details of PIH’s strategies continue to evolve, as patient and supply levels change. But at the strategies’ core are bedrock principles for conserving and—when appropriate—reusing PPE: reduce individual PPE use through careful planning, and minimize the number of people using PPE.
PPE Conservation Strategies
- When evaluating patients with concern for Coronavirus Disease 2019 (COVID-19), providers should wear a surgical mask, gown, gloves, and eye protection. This is a (WHO) and (CDC) recommendation.
- N95 masks should only be used for aerosolizing procedures with COVID-19 patients, such as nebulization, non-invasive positive pressure ventilation, and intubation.
- When possible, concentrate patient care activities to minimize sets of PPE needed. For example, take vital signs and give medications at the same time to use one set of PPE instead of returning a second time and using a second set of PPE.
- Minimize people in an isolation area, or for a patient needing PPE, to the caregivers involved in direct care of those patients.
- Limit the number of observers and non-essential personnel in operating rooms to reduce the use of masks and gowns.
- As needed, consider the extended use of masks between patients (meaning, care providers keep their mask on continuously, rather than removing between patients).
- Eye protection can be cleaned with a bleach solution and reused between patients.
- To ensure that global PPE shortages do not negatively impact care of any kind of patient (including TB patients and surgical patients), it is important to conserve the use of PPE in all clinical areas, as well as COVID-19 response areas.
Caring for Caregivers
PIH also will continue to stay updated on new and emerging data for decontamination methods that may extend the use of PPE, and other safe reuse options.
The PPE guidelines are part of PIH’s unyielding dedication not only to care, but also to caregivers.
“I think as frontline people fighting this…they’re always putting the patient first, and emphasizing that patient care isn’t suffering because of this,” McMahon said. “To me, that’s why it’s our responsibility to make sure that our people who are on the frontlines are protecting themselves—because they’re always putting the patient first, despite whatever risk is coming their way. And that is so important.”


