Research: Integrated Care Improving Outcomes for Patients in Rural Malawi
Integrating care for HIV and non-communicable diseases such as hypertension, diabetes, and mental illness is making treatment more accessible and effective in Neno District
Posted on Dec 23, 2020

Bringing patients for hypertension, diabetes and other non-communicable diseases under one roof for treatment that’s intertwined with HIV care is significantly improving outcomes in rural Malawi, a new study shows.
Partners In Health and Malawi’s Ministry of Health launched their Integrated Chronic Care Clinic, or IC3, in 2015 in Neno District. The IC3 model integrates HIV care with treatment for non-communicable diseases, or NCDs, which can also include asthma, epilepsy, mental illness, and more.
PIH has worked in Malawi since 2007, is known locally as Abwenzi Pa Za Umoyo, and supports 12 health centers and two hospitals across Neno District. Dr. George Talama, the team’s primary health care clinical manager, said building integrated care on the foundation of a successful HIV program was a natural progression.
“We thought, if we could leverage from our HIV platform, we could expand access to care for NCDs,” he said. “Since NCD care was being delivered only at (PIH-supported) Neno District Hospital and Lisungwi Community Hospital, while HIV care was being provided at all 14 health facilities and with better outcomes, we hypothesized that introducing NCD care to this already existing HIV care platform would increase access to NCD care and improve outcomes.”
And providing care to clients diagnosed with both HIV and an NCD—on the same day, at the same clinic—would ease burdens on NCD care and make it easier to access, Talama added.
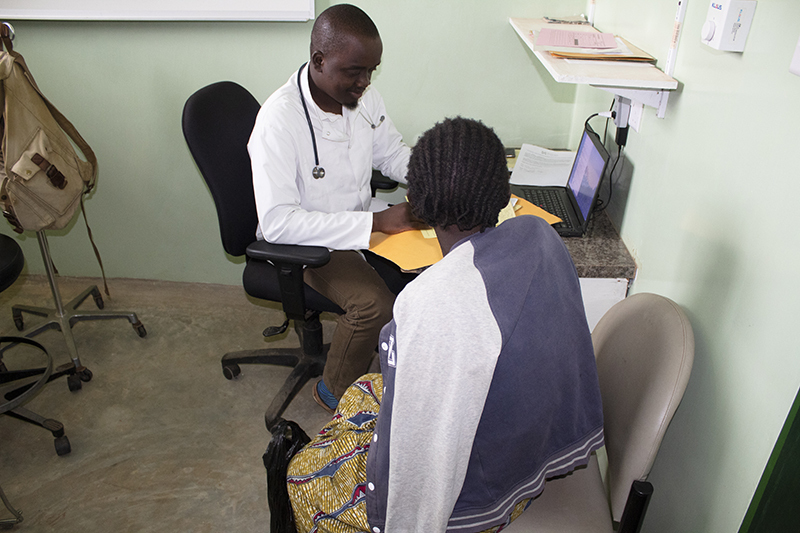
The study was published in October in the journal BMJ Open and features several PIH co-authors. It shows that PIH’s integrated clinics are improving the accessibility of NCD care by allowing patients to have all of their chronic conditions treated on the same day at their nearest health facility. The model also makes better, more efficient use of staff time and clinical space.
Impacts of Integrated Care
Over the study’s three-year period, from 2015-17, integrated clinics at 14 primary care facilities enrolled a total of 6,233 new patients, nearly half of whom presented with one or more chronic NCD. After just a year, retention in treatment stood at 85% of patients with HIV, and 72% of patients with an NCD. Those numbers compare to retention rates as low as 25% found in other studies from similar settings.
IC3 patients in Neno not only were staying in regular treatment; they also were getting better.
Most clinical measurements—such as blood pressure, asthma severity, blood sugar, or number of seizures per month, for patients with epilepsy—showed statistically significant improvement over the course the study. One year after enrolling in IC3 care, more than half of hypertension patients had controlled blood pressure, and patients with epilepsy were reporting fewer seizures overall—with more than 40% regularly reporting no seizures since their previous visit.
Meanwhile, HIV patients continued to show excellent outcomes with continued high-quality care, despite the addition of NCD clients to the clinic.
Hypertension, asthma and epilepsy were the most common diagnoses for patients in the study.
While the concept of integrating HIV and NCD care is not new, the IC3 model is having an outsized impact in Neno. Earlier this year, PIH opened a brand-new, expanded IC3 building adjacent to Neno District Hospital, to better serve growing numbers of patients.
The need is stark. NCDs are a leading cause of death and disability globally, and especially in underserved areas like Neno, where accessing care can be difficult and materials needed to diagnose and treat hypertension, diabetes, and more, can be scarce.
“Before IC3, I was the only one providing NCD care at Neno District Hospital,” said Bright Mailosi, a clinical officer with Abwenzi Pa Za Umoyo. There were many challenges at that time, he added, citing staff shortages, an unreliable supply chain and a high rate of default, or patients leaving treatment.

With the launch of IC3, Mailosi was trained to administer antiretroviral therapy and provide HIV care. At the same time, the HIV team learned about NCDs, including how to diagnose different conditions and counsel patients.
Mailosi said patients aren’t always as informed about NCDs as they are about HIV.
“People hear HIV, and they know what that means,” Mailosi said. “For so long, it was a death sentence. But with NCDs, they may not take it so seriously. So you have to take more time to explain the diagnosis, and the medication, and why it’s important that they take it every day.”
As IC3 continues to scale up in Neno and across Malawi, maintaining supplies of medications will be a critical consideration, as will the increased workload for health center staff.
“There are districts that are already overloaded with clients in need of care for HIV,” Talama said. “For those providers to take on NCD clients as well—that could be quite a lot.”
Nonetheless, Talama said the IC3 has been a huge success so far, and the study indicates the model can serve as a blueprint for integrated HIV and NCD care across Malawi and beyond.
Before IC3, Talama noted, there was only one facility in Neno providing care for NCDs.
“Now all 14 (PIH-supported) health facilities are able to provide NCD care,” he said. “Everyone can see the benefits.”


