Psychosocial and Psychological Interventions
To increase access to care we are decentralizing mental health treatment from psychiatric institutions to the community, by training non-specialist providers to deliver mental health services. PIH develops educational materials for psychosocial and psychological interventions, and for implementing psychotherapies across sites, tailored to local contexts and needs. This provides a forum for clinicians to expand their toolbox for treating common and severe mental health conditions. Mental health care providers participate in weekly supervision, mentorship, and virtual didactic training across sites. PIH’s psychological care is rooted in cognitive-behavioral therapy, and interventions are safe, effective, and culturally sound.
Learn more about our psychotherapy work across the globe:
Haiti Zanmi Lasante Mental Health Curriculum Toolkit

The documents in this toolkit were created during Zanmi Lasante’s (ZL) development of a community-based mental health care system in Haiti. PIH created this toolkit to broaden access to the tools used by ZL providers to screen, manage, and treat patients, believing that the same basic service package can be utilized, with appropriate adaptation, in other locations and contexts.
Psychological First Aid

Psychological First Aid (PFA), a WHO intervention designed to reduce the initial distress caused by traumatic and emergency events and to foster short- and long-term coping, was adapted to the PIH context in the wake of COVID-19. The adapted training package was informed by rainings delivered by PIH mental health teams, around the world and in the U.S., since PIH’s COVID-19 response began in early 2020. PFA trainings were conducted across sites for non-specialist providers across clinical teams, leadership, PIH staff, Ministries of Health, and other partners.
World Health Organization's Problem Management Plus
Problem Management Plus (PM+) (Enfrentando Problemas Plus EP+ in Spanish) is an evidence-based psychotherapy for common mental health conditions, including depression, anxiety, and stress-related conditions. PM+ for individuals was first implemented in Rwanda in 2016 and also was successfully piloted at PIH-supported programs in Peru, Mexico, and Malawi. Sites engaged in a cross-site process of sharing PM+ adapted curricula and implementation experiences, and conducted in-person PM+ trainings. The Cross-Site adaptation process is summarized in the publication below. PIH is piloting Group PM+ for women before and after childbirth, as part of a stepped-care model of screening and treatment for depression into Malawi's National HIV Care Delivery Platform. Leveraging PIH’s experience implementing PM+ globally, PIH partnered with The Family Van mobile health program in Boston to pilot PM+ domestically with virtual training. In response to national movement restrictions due to the COVID-19 pandemic, Socios En Salud/PIH Peru co-developed a PM+ virtual training course for community health workers and mental health providers. You can register for the course below.
World Health Organization's Thinking Healthy

Thinking Healthy (Pensamineto Saludable in Spanish) is a World Health Organization (WHO) evidence-based approach describing how community health workers can reduce prenatal depression through cognitive-behavioral techniques recommended by the mhGAP program. In 2016, Thinking Healthy was adapted for implementation by Socios En Salud/PIH Peru to support pregnant women in PIH’s maternal/child health programs. The intervention continues to be delivered to about 300 women in northern Lima to reduce perinatal depression. In reaction to national movement restrictions due to the COVID-19 pandemic, the team developed a Thinking Healthy virtual course to train community health workers and health professionals on how to deliver mental health support for common mental health conditions. You can register for the e-learning course below.
Disclaimer: The WHO is not responsible for the content or accuracy of this translation. In case of inconsistency between the English and the Spanish version, the original English version will be binding and authentic.
Common Elements Treatment Approach

The Common Elements Treatment Approach (CETA) is an evidence-based intervention that combines treatments for a range of common mental health conditions such as depression, anxiety, substance use, stress-related conditions, and behavior problems in youth. It is grounded in a community-based approach and was developed in low-middle income contexts for non-specialist and lay providers. CETA is being piloted across PIH sites based on local priorities and integrated into existing services through a phased approach. In October 2019 a 2-week training was held in Freetown, Sierra Leone on CETA in partnership with the Johns Hopkins University CETA group. The training strengthened skills in care for common mental health conditions and created space to learn implementation strategies in different contexts. Cross-site visits to exchange knowledge, such as the ones highlighted in the figure above, have greatly enriched bonds across PIH and global mental health collaborators.
Community-Based Psychosocial Rehabilitation
Across PIH sites mental health program implementers have expressed a universal challenge among service users seeking mental health services: service users face barriers to social reintegration. PIH sites have been engaged in Psychosocial Rehabilitation, social reintegration, and recovery efforts for decades. In 2021, a cross-site steering committee dedicated to Psychosocial Rehabilitation (PSR) created and piloted a human-rights centered curriculum and training package titled "Community-Based Psychosocial Rehabilitation." The outline for this curriculum originated from Inshuti Mu Buzima (IMB), PIH’s sister organization in Rwanda, was piloted by PIH Liberia, and can be adapted to fit the local context and population needs.
Women's Circles
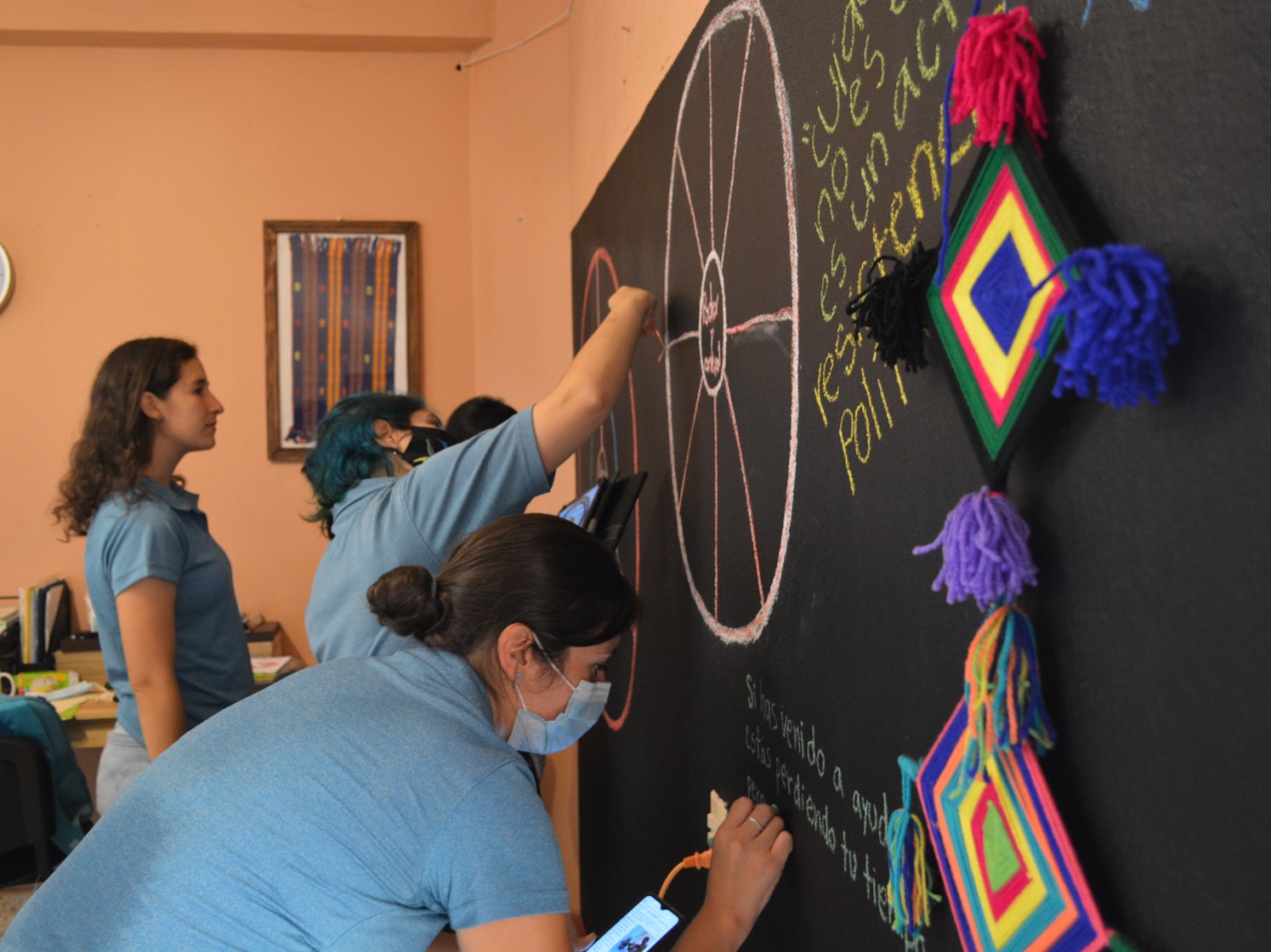
The rural communities of the Sierra Madre of Chiapas have limited mental health services that are culturally appropriate and that enable community cohesion from the sharing of knowledge. In this area there is a high prevalence of violence against women, which is related to a higher number of women with depression and anxiety than men. Women are rarely considered in community decisions, and although there are many women living in similar situations of inequity and violence, there are not enough spaces for them to connect and share knowledge in the absence of patriarchal structures. We co-created women's circles together with four Community Mental Health Workers, named by themselves "Cuidadoras". These sessions consist of 8 sessions facilitated by the Cuidadoras and they use popular education methods to promote mental health with a feminist perspective.
snapshot of women's circles (english)
snapshot of women's circles (spanish)
