Cholera Outbreak Spreads Through Southern Malawi
Cyclone’s torrential rains, floods left residents with limited access to safe drinking water
Posted on May 19, 2022
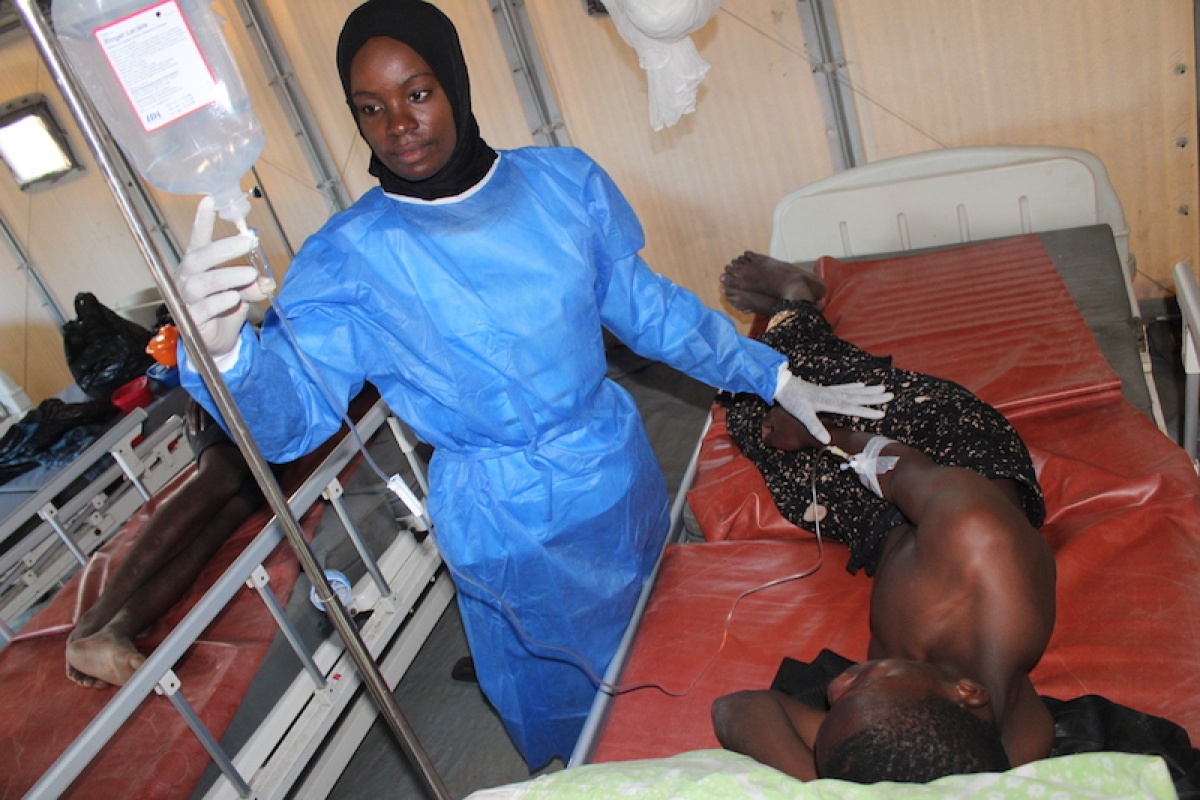
The first case, diagnosed in early March, was a 57-year-old man from southern Malawi. The second, an 11-year-old boy.
Now, cholera, spreading through six districts in the south, has killed 12 people and sickened at least 300 as of May 19, 2022.
One of those sick patients, suffering from severe symptoms, was a 1-year-old girl. She was treated last week at Lisungwi Community Hospital in the Neno District, where Abwenzi Pa Za Umoyo, (APZU), as Partners In Health is known in Malawi, has collaborated with the local Ministry of Health to activate rapid response teams to mitigate the impact of the outbreak and help with recovery efforts.
“This is bad,” said the child’s mother, who declined to be named. “I was so afraid to look at my child. She has had diarrhea and vomiting before, but this was different.” The child was treated, and the mother, profoundly grateful for the medical attention, was able to take her daughter home today, said Dr. Brown Khongo, secondary healthcare manager at APZU.
Outbreak in Neno
Neno District, one of the hard-hit areas, has had 62 cases of cholera as of May 19, 2022 with one death—a 13 year old boy who was pronounced dead on arrival at one of the health centers in the district.
Cholera is an extremely virulent disease that can cause severe diarrhea and vomiting and can be fatal if left untreated, according to the World Health Organization. It can spread rapidly, depending on the frequency of exposure, the exposed population, and the setting. The incubation period is between 2 hours and five days after ingestion of food or water contaminated by sewage bearing the bacteria, Vibrio cholerae.
Khongo said that, typically, cholera is seen during Malawi’s rainy season, November through April, but years have passed with no cholera at all in Neno. The current outbreak, according to health leaders, is clearly the aftermath of Tropical Storm Ana and Cyclone Gombe that, earlier this year, caused torrential rain and flooding, leaving many people “no access to safe drinking water and sanitation facilities and thus, at risk of widespread disease outbreaks including cholera,” the WHO reports.
The storms impacted over 221,000 households and 945,000 individuals nationwide, officials said; in Neno District, more than 7,500 homes were destroyed.
Chronic Water Problems
The storm’s pounding rain, wind, and subsequent flooding disrupted already weak structures, including water sources, Khongo said. Homes across the region collapsed and most people lost their household items for sanitation and hygiene. “Outdoor toilets collapsed and utensils were lost,” he said. Many families are still sheltering with neighbors while rebuilding their own houses, leading to possible overcrowding and further demands on the few sanitation and hygiene facilities that are available. “This,” he said, “adds to the chronic water problems, especially in Lower Neno (where all cases are coming from now) and part of Upper Neno.”

The main sources of water in the lower region are narrow wells, or boreholes, Khongo said, and there is no piped water supply. But the water from the boreholes and the few personal wells that exist are salty, he said, “so some parts of the community use water directly from the rivers and streams because they are less salty.”
So far, there’s been no testing of water to pinpoint the source of the outbreak, Khongo said: “But the presence of the outbreak is enough to conclude that the water is contaminated.”
Responding to an Emergency
The APZU team, working with Ministry of Health colleagues and others, has mounted a strong emergency response, including setting up a cholera treatment center at Lisungwi Community Hospital with 20 beds, running water, and medicines and other medical supplies. So far, over thirty patients have been admitted to the center with seven currently being managed.

The team is also conducting:
- Epidemiological assessments to map areas reporting cholera cases;
- Contact tracing for all confirmed cases in the community;
- Risk communication and community engagement;
- Safe water and household chlorine distribution.
APZU continues to fill medical and other gaps, for instance, by helping to procure more cholera treatment and test kits and mobilizing a cholera vaccine plan, among other efforts. This is not new for PIH: successful cholera vaccination campaigns were launched previously in Sierra Leone and Haiti. Indeed, PIH's work in Haiti during a 2010 cholera outbreak, rapidly mobilizing to treat more than 145,000 Haitians and vaccinate another 45,000, was key to the development of a global stockpile of oral cholera vaccines by the World Health Organization and other partners in 2012.
Climate Change and Infectious Diseases
Of course, no single storm or cyclone can be blamed on the warming climate. But scientists and climate experts acknowledge that climate change does affect the frequency and intensity of extreme weather events, which in turn can create human disasters, particularly for the socially vulnerable. More (and more intense) cyclones lead to flooding and water contamination from runoff or sewage, which can lead to the spread of contagious diseases, such as cholera.
Dr. Kelsey Ripp, an internist working on climate change education for medical students at the University of Global Health Equity in Rwanda, a Partners In Health-supported university sees global health and climate change as intimately intertwined.
“We often call climate change a threat multiplier,” said Ripp, “because it worsens various health problems by exacerbating other widespread contributors to ill health, such as poverty.”


