Heart Patient, Advocate, and Soon-to-be-MD
Posted on Sep 28, 2019

As we come together for World Heart Day on September 29, we celebrate Erneste Simpunga and other people living with a range of heart diseases within the communities where we work.
Simpunga, 29, was diagnosed with rheumatic heart disease at age 16, in his home country of Rwanda. After a lengthy journey to surgery, he had two heart valves replaced in July 2008, at Brigham & Women’s Hospital in Boston. The experience inspired him to become a doctor, and on November 8, 2019, his 30th birthday, he’ll graduate from the University of Rwanda’s School of Medicine and Pharmacy.
While he hopes to conduct his residency and his fellowship in the U.S., Simpunga’s long-term goal is to work in Rwanda, as a cardiologist, cardiac surgeon or professor of clinical anatomy. Rwanda currently has about seven cardiologists for its population of 12 million.
In the years following the surgery that saved his life, Simpunga has been an ardent patient advocate. He’s spoken at events including the 10th anniversary of Partners In Health’s work in Rwanda; the 2016 Team Heart Boston Gala; a global forum on noncommunicable diseases (NCDs) in Sharjah, United Arab Emirates; and at related events in Kigali, Rwanda’s capital.
He is a member of Rwanda’s NCD Alliance, and has served on the first advisory committee for the alliance’s “Our Views, Our Voices” patient advocacy initiative.
Here, he shares some of his incredible life story.
Frightening news to hear
In May 2006, when I was 16 and in secondary school, I got a very somber diagnosis from one of the two cardiologists in my home country of Rwanda.
He told my father not only that I had rheumatic heart disease (RHD), but also that because of the disease, one of my heart’s four valves needed to be replaced. A second valve needed surgery or even a replacement, as well.
It was frightening news to hear—but my family and I had known it was coming.
By the time I was able to see that doctor, a cardiologist in the capital city of Kigali, I had been suffering debilitating symptoms of RHD for more than two years.
The summer of 2005 was when I finally determined that something was seriously wrong with my health. I then stayed for some time at the health center closest to the small community where I grew up, in Rwanda’s Eastern Province. Care providers at the health center gave me several inaccurate diagnoses, before, eventually, I was referred to a district hospital, and then finally to the University Teaching Hospital of Kigali.
There, we learned that there was a long line of patients waiting for treatment ahead of us, and a cardiologist could see us in four months if we used health insurance to pay for the visit.
I was very thin, with a hugely distended abdomen and built-up fluid in my legs. I was short of breath nearly all the time, even when I was at rest. I couldn’t walk briskly uphill for more than 30 seconds—as I had to do on my daily walk to school. Rwanda, itself, is known as the Land of 1,000 Hills. Because I had to move slowly, walks that used to take me just 10 minutes now took more than an hour—and if I tried to walk any faster, I would get heart palpitations and sometimes faint.
An unbearable cost for care
Knowing all of that, my family decided to see the cardiologist at his private clinic, rather than wait, and to pay 100 percent of the cost.
That cost quickly grew.
The cardiologist said our family would need to find about $15,000US, because the surgery I needed couldn’t be performed in Rwanda, and I would have to go to India.
He added that, in most cases, the outcome was really good, especially for young people like me—even though my condition seemed advanced.
We looked at him for a moment, in silence, as we took in that news. Then, my dad said:
“Doctor, this is my first time to hear of such a disease. We used to think my son might have HIV or tuberculosis, given how thin and tired he is. Are you telling us the truth, that this is a heart disease? Are there any other patients like him?”
The doctor insisted on his diagnosis, and reiterated that a good outcome was likely if proper treatment began as soon as possible. However, we had to tell him that our family could not afford the cost.
The doctor said another option, then, would be to wait for visiting teams of foreign doctors who could perform the surgery I needed, and who would come to Rwanda and treat local patients through future partnerships with the Rwanda Ministry of Health. But that could take a year or two, or more. The doctor’s concern was that the longer we waited, the less potential I had to be a candidate for treatment from those teams, because my condition could worsen.
Rwanda already was working with an Australian cardiac surgery team, by chance, and had been for two years—but that was a pediatric team. At 16, I was too old for pediatric treatment and would have to wait for a cardiac surgery team that was treating adults.
That was just one example of the many hurdles that arose.
So, the doctor and my family made a plan, while we waited.
“I will put him on daily medications and I will need to check on him while we wait, possibly every month,” the doctor said.
The long wait for surgery
Luckily, I did well on the medications, which included about 180 pills a month and penicillin injections. I later learned that other patients with a similar disease, and similar treatment, were not so lucky—some saw their conditions worsen despite the medications, and needed hospital visits up to twice a month.
I remained on the medications, awaiting surgery, for two years.
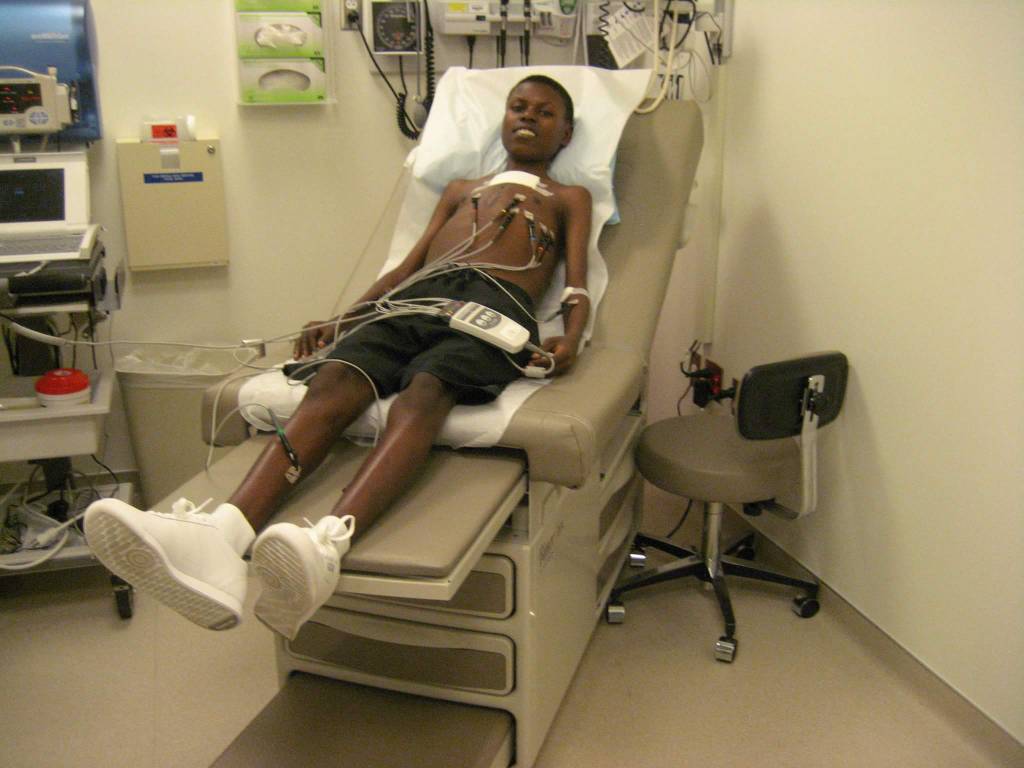
At last, in April 2008, I was presented to Team Heart, a medical nonprofit that’s based in Boston and has worked for more than a decade to build sustainable cardiac care in Rwanda. Team Heart brings volunteer doctors and nurses to Rwanda every year for surgical missions, working with the Rwanda Ministry of Health, collaborators including Partners In Health, and many others.
Their visit in 2008 was Team Heart’s first trip to Rwanda. They planned to see 12 patients. As it turned out, I was the sickest—so sick, in fact, that I wasn’t a candidate for surgery in Rwanda.
However, I was given a second chance. In July of that year, Team Heart and PIH brought me to Boston, where my surgery was performed safely by some of the same doctors who had visited Kigali just months before.
After doctors successfully installed two artificial valves in my heart, I stayed in Boston for three months, living with my lead surgeon and having regular checkups with cardiologists. The extended stay gave me a unique opportunity to attend the 2008 Rwanda Day in Boston, and to meet Rwanda President Paul Kagame and the country’s minister of education at that time. I thanked both of them for supporting the medical partnership that was enabling me to live a healthy life, return to school and so much more.
But challenges still remain.
Replacing two of my heart’s four valves means I have to take three different medicines—totaling about five pills every day—and see a cardiologist at least twice a year, for the rest of my life. One of the medicines is a blood thinner, which requires me to have my blood tested once a month. This is not always easy.
When I returned to Rwanda after my surgery and recovery in 2008, there was only one hospital in the country, in Kigali, that could do the monthly blood test I needed. Resources have grown since then, with the help of the government, and now blood tests are offered in several districts.
I am grateful that the country has continued to advocate for people with heart conditions. There now are about five visiting teams that offer heart surgeries, and the government is providing scholarships for aspiring cardiologists. I am also happy that the country has affordable health insurance and everyone is enrolled in the system.
From patient, to advocate
The major challenge I see is our very poor patient-doctor ratio, especially in specialized areas like cardiovascular medicine. Enormous demand is created when a country has just seven cardiologists and one cardiothoracic surgeon for 12 million people, and while that number slowly is improving, there is still a long way to go. When I was sick more than a decade ago, there were just two cardiologists in Rwanda, for its more than 9 million people at that time.
International help is direly needed. For example, top-ranking medical schools could provide more support for young Rwandan doctors specializing in cardiology. More also can be done to ensure postoperative medications are always available for patients, who need to take them every day to continue feeling well. Additionally, health care providers at the community level must be trained on how to diagnose RHD earlier, to potentially prevent more serious complications down the road.
I know the Rwandan government is aware of these issues, and working to address them. But system-wide change takes time, and more partners are needed to accelerate the process.
Overall, my wish for Rwanda is to have a young generation free of rheumatic heart disease. I encourage anyone experiencing symptoms to not ignore them, and seek out care that they might need. For those fighting the disease and those with lifelong care, like me, my wish is that care and resources across Rwanda one day will equal what is available in developed countries.


