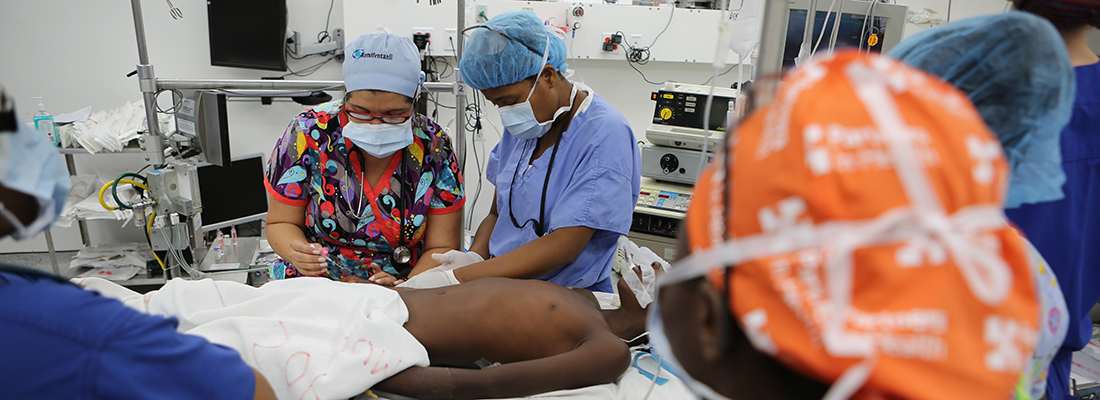
Surgery
Five billion people worldwide lack access to safe surgeries, according to the World Health Organization. The shortage is most severe in low- and middle-income countries, where nine out of 10 people have no access to basic surgical services. In Haiti’s Central Plateau, just two orthopedic surgeons serve 500,000 people.
Without surgical care, easily treatable conditions can become dangerous--or worse, fatal. Procedures such as cesarean sections could prevent the vast majority of maternal deaths. Surgery is also a cost-effective health intervention—repairing a cleft palate can prevent a speech problem down the road.
Improving surgical care, training, and research are key priorities in global health—and PIH is a leader in each of these efforts.
Since 2013, 11 surgical residents have graduated from University Hospital in Mirebalais, Haiti; another 18 are in training. Nearly 120 surgeries performed monthly in Sierra Leone’s Koidu Government Hospital; half are lifesaving C-sections. More than 4000 general surgeries and 10,000 C-sections performed globally each year.Our Impact



Global Collaboration
We collaborate with experts around the world to improve surgical care. As a longtime participant in The Lancet Commission on Global Surgery, launched in 2013, we work with other health and policy experts to ensure that all people have access to affordable, high-quality surgery and anesthesia.
We live these goals at many of our supported health facilities, where clinicians offer surgical care, including: orthopedics, otolaryngology (ear, nose, and throat), plastics, pediatrics, urology, obstetrics and gynecology, and general surgery. Staff at the internationally accredited University Hospital in Mirebalais, Haiti, work alongside international teams to perform especially complex surgeries, such as the separation of conjoined twins, pediatric cardiac surgery, and neurosurgery.
Investing In Surgeons
We are also working to train the next generation of surgeons. Our programs across multiple countries offer surgical mentorships, residencies, and advanced education for local physicians. The Paul Farmer Global Surgery Fellowship and the Global Health Equity Residency teach surgeons how to provide care in resource-poor settings, with the ultimate aim of producing surgical researchers and policy advocates.
In Rwanda, surgery is an integral component of studies and training at the University of Global Health Equity (UGHE), a PIH initiative launched in northern Rwanda in 2015. Students enrolled in the 6.5-year medical program earn bachelor’s degrees in medicine and surgery and a master’s degree in global health delivery. The rigorous program includes instruction from renowned surgeons who have worked in a variety of settings around the world.
