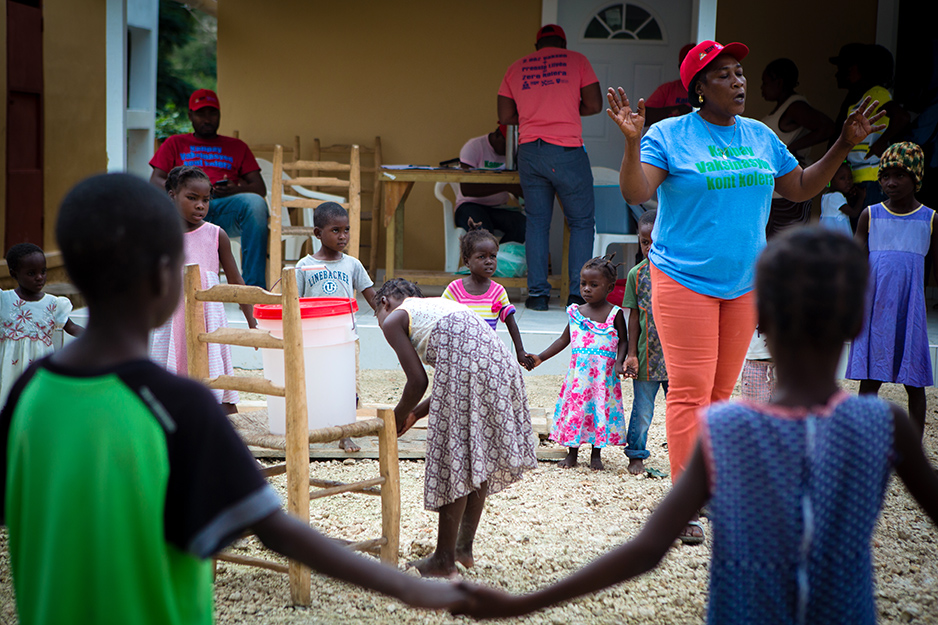A Mission to Stop Cholera in Haiti
Posted on Dec 21, 2017

A soft rain fell outside University Hospital in Mirebalais, Haiti, as the courtyard filled with people on a Wednesday morning. Inside, the day’s first patients sat beneath ceiling fans that pushed thick air around a dim waiting room in the 300-bed teaching hospital built by Partners In Health. They watched as dozens of doctors, nurses, and community health workers, wearing bright red baseball caps and pastel-colored T-shirts, buzzed in and out of a nearby storage room and up and down the hall.
It was November 15, a highly anticipated day for Haiti’s Ministry of Health and Zanmi Lasante, as PIH is known locally. In collaboration with Massachusetts General Hospital's Center for Global Health, they were launching an ambitious cholera vaccination campaign that aimed to cover the entire commune of Mirebalais, or roughly 100,000 people. Each resident was to receive two doses of the vaccine over the course of a month, along with interventions to help treat drinking water at home, and educational messages about good hygiene and sanitation.
Just before 8 a.m., most teams had gathered what they needed: gray coolers filled with vaccine vials, registers to record names, and thick stacks of green vaccination cards they would fill out and hand to patients as a personal record—and reminder—of their two doses.
A supervisor called roll in Creole, then sent teams on their way.
“Moun ki genyen bagay yo, ale!” Or, “Go, if you have everything!”
The vaccinators streamed out of the waiting room to set off on foot, climb into heavy-duty pickups, or hop on motorbikes—three to a seat—for the long days ahead.

A plague descends
The Aba Kolera, or Stop Cholera, project has the lofty ambition of eliminating the transmission of cholera in central Haiti through hygiene promotion, vaccination, and access to clean water. It’s an innovative approach to address the immediate burden of cholera. Building and maintaining a nationwide water and sanitation system is an important goal that PIH supports, but one that remains some time off.
The 66 vaccination teams were to visit 84 schools, 59 churches, and five health centers in a week’s span, then methodically move door-to-door throughout the entire commune of Mirebalais to ensure complete coverage. The task was ambitious. But so was the team.
“We are trying to change the status quo on cholera in Haiti, and globally,” says Dr. Louise Ivers, PIH’s special advisor, executive director of the Center for Global Health at Massachusetts General Hospital, and the Aba Kolera project’s program director.
Haitians never knew cholera before 2010. Shortly after the devastating earthquake in January that year, the United Nations brought in a group of peacekeepers from Nepal—where the capital, Kathmandu, had recently suffered an outbreak of the disease—and set them up in a camp near Mirebalais with poor plumbing. Contaminated sewage leaked into a tributary of the longest river in Haiti, the 200-mile Artibonite, which is a water source for countless Haitians.
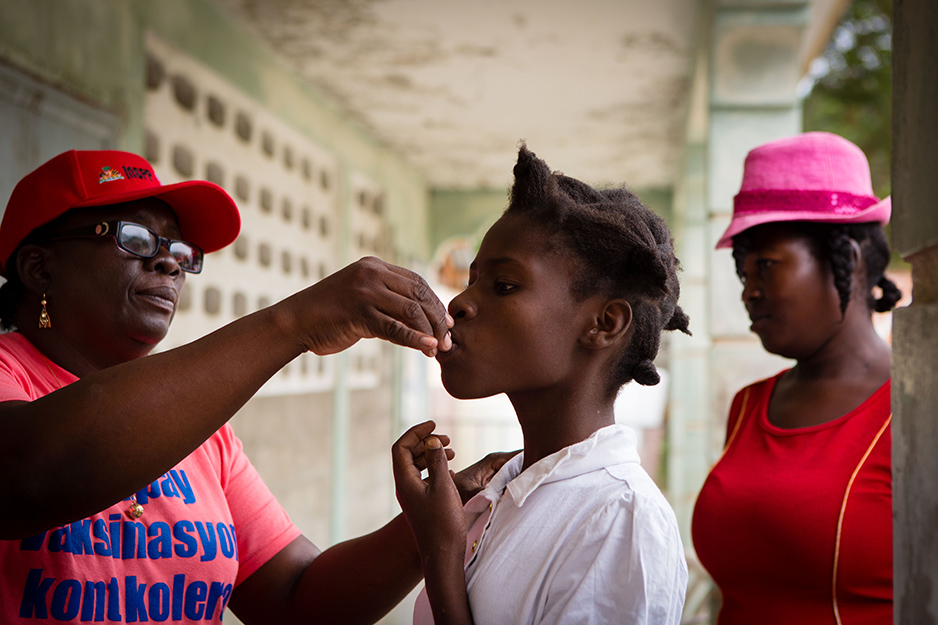
The result was a cholera epidemic of historic proportions. Since October 2010, more than 9,700 people have died and at least another 815,000 were sickened from the disease. Cholera causes such severe vomiting and diarrhea that—if left untreated—a patient can die from dehydration within 24 hours. Haiti’s epidemic has been devastating, and is second only in size and severity to the one currently ravaging isolated, war-torn Yemen.
Battling a new disease
PIH was among the outbreak’s first responders in Haiti. Within several months, staff set up 11 cholera treatment facilities throughout the Central Plateau and immediately began treating the sick. More than 3,300 community health workers were trained to identify symptoms and triage neighbors to nearby health centers. Since those early days, PIH has treated more than 180,000 people. And while the number of sick now pales in comparison to 2010, staff still treat patients for cholera today.
Doctors, nurses, and community health workers also work to prevent cholera infections by teaching about proper water and sanitation practices and vaccinating as many patients as possible, which boosts immunity for up to five years. In 2012, PIH vaccinated 50,000 people in communities north of St. Marc. And following Hurricane Matthew in 2016, leaders traveled to the south to help the government vaccinate 800,000 residents.
When PIH proposed the most recent campaign, Haiti’s political climate was hardly ideal. Former President Michel Martelly left office in February 2016, with no clear successor following a contested election. A series of interim governments passed through Port-au-Prince until President Jovenel Moïse was elected in November 2016, and took office in February.

Dr. Ralph Ternier, director of community care and support in Haiti, and his team had been waiting to start the Mirebalais vaccination campaign since the beginning of 2017, following national committee approval that the city was a cholera hot spot. The delays were stressful. They made connections with each administration and pushed the urgency of the situation. After all, this was part of the national plan to vaccinate the Central Plateau and lower Artibonite. Plus, the nearly 270,000 doses of Shanchol and Euvichol issued from the global stockpile had an expiration date. If they were going to launch this operation, they had to act fast.
Their pleas finally gained ground and, the last week of October, Ternier got a green light from the government. He and his team swung into action—calling on dozens of PIH and government staff, gathering supplies, printing banners, and pushing out radio ads to publicize the campaign. They knew they faced obstacles, such as rough terrain in the middle of rainy season and a mostly rural population. Yet they also knew the cost of not trying—what PIHers call “stupid deaths” from diarrheal disease.
“I strongly believe we are doing the right thing for the people, so we cannot fail,” Ternier said on the eve of the most recent campaign’s launch. “We cannot fail. We cannot.”
Launch day
After sending off the last vaccination teams from University Hospital, Dr. Maurice Junior Chery, assistant coordinator of the cholera program, tapped his smartphone en route to his first stop. As one of 10 supervisors, his job was to check stock and supplies, ensure vaccinators followed protocol, and investigate any reports of patient side effects.
The PIH pickup zipped by cement-block houses with zinc roofs, roadside lottery stands, and makeshift barbershops and slowed at the sight of a campaign banner draped above the road beside the clinic in Sarazin. A couple dozen men and women sat patiently on benches under an awning to escape the gentle rain. The group needed registers, pens, and pencils, and so hadn’t been able to start work. Chery took note and passed word along to the rest of the supervisors. Someone, he assured the group, would arrive soon with supplies.
Heading back toward the city, Chery and his team pulled over at a roadside store, where vaccinators had set up shop under an awning. At least 20 people crammed into the tight space, most of them schoolchildren in tan-and-white-checkered shirts.
Blondine Tirogène pried the aluminum foil from a vial and poured the milky substance into a woman’s mouth. Her colleagues took down patient names, handed each person a green vaccination card, and told them to keep it safe. They would be back in two weeks to administer the second, and final, dose.

Everything running smoothly, Chery and his team hopped back in their pickup and headed to the other side of Mirebalais. They veered off the main road to pass sugar cane fields and banana trees, rumbled through a small stream, and climbed up a chalk-white hill to the public school in Crete Boule.
But no one was there, except for the team’s leader, Jomert Lapointe. School was closed due to the rain, so his team was searching for an alternative vaccination spot. (Such closings are common in the wet season, as officials don’t want schoolchildren fording rain-gorged streams.) Chery’s team unloaded supplies into the storage room and headed back to town.
That night after dinner, Ternier sat with Chery and other supervisors, including Dr. Kenia Vissieres, director of the cholera program, Dr. Myrtha Thermidor, the Ministry of Health's deputy director of the general vaccination program, and Miss Esther Mahotiere, the nutrition program coordinator. They rehashed the first day, discussing minor hiccups and sharing early victories.
Some vaccinators had trouble opening vials. Others had used pencils instead of pens to fill out vaccination cards—a problem, because the information could rub off more easily. Despite these small challenges, they had already reached thousands of people.
Pa pike bebe
The next day dawned cloudy, yet dry—a good sign for turnout. The first stop for Chery and his team was the public school in Fond Michel, where they moved tables under the awning of a dilapidated building. Children dressed in checkered white-and-navy shirts and navy slacks or skirts gathered in pockets around the schoolyard and stared at the visitors. They laughed and spoke loudly, interrupting the one teacher attempting to give a lesson inside.
Rose Marie Renati, a PIH health agent, lined up the children. The first ones put on brave faces, despite worry lines creasing their brows. They each gave their name, age, and address, then tilted their head back to receive the salty tasting vaccine.

“Gade sa,” said Thermidor, handing one boy his vaccination card and telling him to put it in his backpack.
Having seen everyone, Miss Ketty Tout-Puissant, PIH’s nurse coordinator for community activities in Lascahobas, gathered the children into a classroom to teach a catchy anti-cholera tune. Some children continued singing the chorus even after the vaccinators had packed up.
The team’s next stop was a nearby orphanage. Two caretakers and 30 children emerged from ramshackle buildings, some in worse shape than others, to greet the visitors. As the nurses and doctors set up their supplies, Driver Holiere Robuste organized the children into a line and coaxed the youngest ones to join.
“Pa pike bebe, pa pike,” said Robuste. Or, “It’s not a shot, baby. It’s not a shot.”
After the last child was vaccinated, and a few neighbors as well, Renati placed the children in a circle around a five-gallon bucket of water and a bar of soap. She picked a young girl from the crowd and both methodically washed their hands, while Renati preached the benefits of good hygiene. Each child then took turns sudsing up. They giggled as bubbles slipped off their slick hands.
The rest of the afternoon flew by. The team stopped by a church in Fond Cheval, where Tout-Puissant advised vaccinators to write only in pen, not pencil. Then it was off to a church neighboring the St. André School in Trianon, where schoolchildren received their vaccinations alongside a stone altar, under garlands of fake flowers. At Dramane, young and old formed a line that curled around a mud-and-stone house abutting the dirt road.
Past sugar cane fields and rolling hills, a crowd filled the Church of the Nazarene in Penier Siwal to wait for a vial from their neighbor, Jean Roland Doux—an elderly man who embraced his job with efficiency and panache. Loudly, he called out patients’ names and emptied vaccine into their mouths with a flourish.
At each rally point, residents arrived en masse and waited patiently for their turn. They knew the importance of the cholera vaccine; surely, many of them had lost friends and family to the horrible, and completely preventable, disease.
By the campaign’s last day, the team had reached more than 88,000 people. It was a major milestone, but no one could celebrate quite yet. They had another round to go.
On December 10, the same crew of vaccinators grabbed supplies, coolers, pens and pencils and repeated their first performance for another seven days. When all tallies had been counted, the team had twice vaccinated at least 80,000 people—or nearly the entire commune of Mirebalais.
Ternier and his crew had done the right thing. They had persisted, despite the obstacles. They did not fail their mission. They did not.