A Mother, Her Twins, and an 8-Hour Ambulance Ride in Mexico
Posted on May 11, 2018

Alejandra Catalina Ramirez was starting to feel big—a completely normal sentiment for a petite woman in her sixth month. This being her third pregnancy, the 29-year-old had naturally begun showing much earlier than she had with each of her two sons. But at the rate she was growing, who knew how large this baby would be after three more months?
She arrived at the clinic in Soledad, Chiapas, for her prenatal appointment in March 2017 and was greeted by three doctors working with Compañeros En Salud, as Partners In Health is known in Mexico. Dr. Ariwame Jiménez had two visitors that day from the main office in Jaltenango—Dr. Martha Arrieta, her new supervisor, and Dr. Mariana Montaño, the maternal health program coordinator.
“Looks like you’ve got two in there!” said Arrieta, who noted Ramirez’s size as she welcomed her to the clinic.
Ramirez lay down on the examining table and lifted her blouse. Arrieta methodically moved the wand of an ultrasound machine over the mother’s rounded abdomen. All at once, the room filled with the steady wub, wub, wub of a mighty little heart. The doctor swished her wand into a different position. Another wub, wub, wub echoed through the exam room.
What had started as a joke suddenly became reality: Ramirez was pregnant with twins and, she would discover in a later ultrasound, they were boys. The mother beamed and didn’t seem surprised—twins ran in her family. She couldn’t wait to return home to share the news with her 28-year-old husband, Norberto Hernandez, and their sons, 7-year-old Alexis and 4-year-old Yoiner.
For good measure, the doctors recommended that Ramirez travel to a more specialized hospital in Huixtla, where technicians could perform a more detailed ultrasound. Thankfully, she did; what she discovered helped save her and her sons’ lives.
Breaking barriers
One-third of women living in Chiapas still give birth at home, usually with the assistance of a traditional midwife, according to Mexico’s National Institute of Statistics and Geography. That number nearly doubles to 60 percent, Montaño said, in the 10 rural communities PIH supports.
Most local health centers are not equipped for deliveries, and the closest public hospital for many Chiapanecans is in Jaltenango, a good three-hour drive down rutted dirt roads cut through the Sierra Madre mountains.
These and other barriers help explain why maternal mortality in the state of Chiapas is among the highest in Mexico, with 81 deaths for every 100,000 deliveries compared to 36 in 100,000 nationwide as of 2015, the year of the most recent government data.
In an effort to save more women’s lives, PIH has been partnering with Mexico’s Ministry of Health to educate expectant mothers on the importance of delivering in a hospital, while also providing technical and culturally appropriate training to local health care professionals. Together they began operating Casa Materna, a maternal home next to the Jaltenango hospital. There, expectant mothers receive pre- and postnatal care at the hands of obstetric nurses and first-year doctors, all supported and supervised by PIH clinicians. At least 21 women have given birth at the home, and clinicians have provided 970 consultations since its doors opened in May 2017.
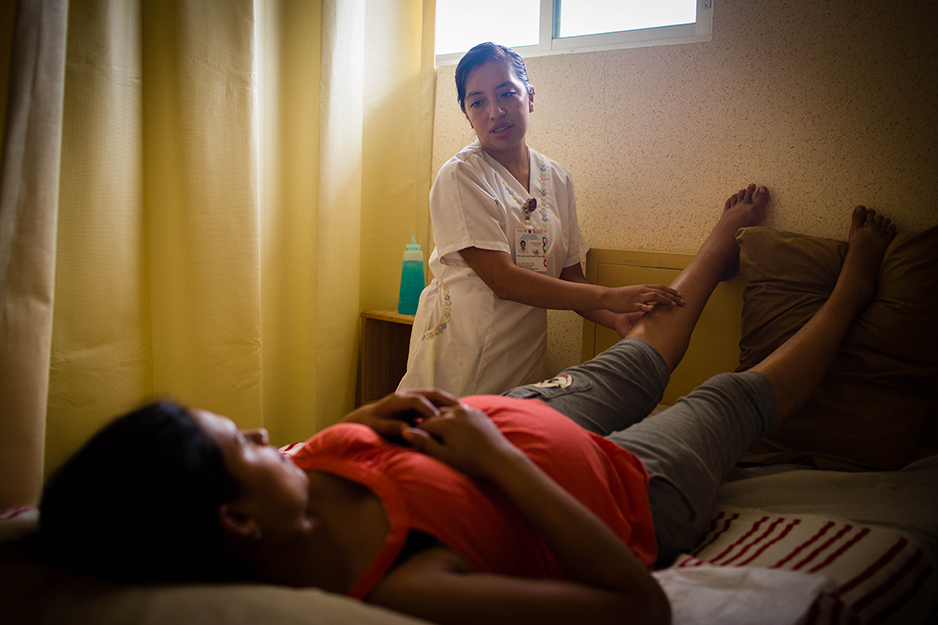
Women who live far from the hospital are encouraged to stay on hospital grounds, for free, as they approach their due date. When labor begins, they walk from the hostel to the hospital for immediate access to doctors and nursing staff. A pair of ambulances stand nearby to transport mothers to a specialized hospital one and a half hours away in Villaflores, should they need an emergency cesarean section.
Together, these measures meet the needs of most laboring mothers. But there still are rare cases, such as Ramirez’s, that test the system.
An epic voyage
Several weeks after her first visit to Soledad, Arrieta returned to supervise Jiménez. Ramirez, now about seven months along, was among the patients the two doctors saw that day. She arrived with her new ultrasound images, which the doctors pored over with growing concern. Ramirez was carrying an excessive amount of amniotic fluid—a risk factor for premature labor. They recommended she undergo a procedure that would remove some of the extra fluid.
The procedure involves a measure of risk—it sometimes causes internal bleeding that can endanger the pregnancy. But for Ramirez, there was equal risk in doing nothing. The doctors informed her that she would likely go into labor within two weeks if she and her husband decided against removing the extra fluid. In that case, they advised, she should head to Jaltenango sooner rather than later to be near the hospital.
Hernandez wasn’t thrilled with either option. He had already missed too much work while traveling with his wife for doctors’ appointments outside the community, and was thinking about their other sons back home. In the end, the couple decided to remain in Soledad and try their luck.


That luck turned sour within days of Ramirez’s last appointment. Her water broke when she was 33 weeks along, roughly two months early. Panicked, they left their sons in the care of Hernandez’s mother and hailed a taxi to Jaltenango.
Meanwhile, Montaño and a social worker based at the hospital worked their contacts to find a facility that could perform an emergency c-section and provide intensive care for premature infants, both of whom—the clinicians assumed—would require incubators. San Cristóbal was full. Comitán said no. Finally, Montaño got a green light from a hospital in Tapachula, but officials there requested that a doctor and nurse accompany the couple in the ambulance.
Arrieta, who was supervising another PIH doctor in a neighboring community, fielded the call from Montaño: Would she be able to go along for the ride? “Sí!” came the response.
Within hours, Arrieta arrived in Jaltenango and, along with a nurse from the hospital, jumped into the back of the awaiting ambulance. Hernandez was already in the passenger seat. Ramirez lay on a gurney, losing amniotic fluid and enduring waves of early labor pains.
The anxious crew took off for the eight-hour ride south. None of them had ever traveled to the Tapachula hospital, but that didn’t matter at the moment. They would get there. They had to.
The boxy vehicle swayed back and forth over the mostly paved roads. A mountain range rose between them and their destination. Up they went, then down, navigating switchbacks along narrow two-lane highways. Arrieta stood the entire way, her legs straddled behind Ramirez’s gurney to keep it in place. She could hear Hernandez vomiting out the passenger window the entire drive.
On the morning of April 29, the group arrived at the Tapachula hospital and wheeled the laboring mother into the emergency room. Nurses assured Arrieta that the family was in good hands. The journey had been a harrowing adrenaline rush. Now, with her task complete, Arrieta felt drained—and reluctant to let go and return home.
Ten hours later, though, Arrieta arrived back in Jaltenango, filled with a sense of despair. What if they hadn’t succeeded? What if, despite all their best efforts, the worst had happened?
But Arrieta didn’t need to worry. Montaño was there at the office, waiting with good news. Ramirez was recovering after her c-section, and both boys were alive and hooked to oxygen and feeding tubes. Gabriel had come first, weighing in at 3 lbs. 5 ozs., and Emanuel had come second, at just over 3 pounds. They wouldn’t be able to return home until they could breathe on their own and had gained a significant amount of weight.
Ramirez was discharged within days, but she and her husband had nowhere to stay. They knew no one in Tapachula, couldn’t afford housing, and needed to be near their sons for regular feedings.
So, like many families of the hospital’s in-patients, the couple slept outside. They accepted food and café con leche from a local order of nuns who visited daily. They called home regularly to check on their older sons. And they tried their best to remain patient as days spun into weeks, and their small sons grew stronger.
Ramirez knew exactly how long they had followed this routine: “One month and 10 days.” Finally, on June 4, doctors examined the twins and declared them well enough to return to Soledad. With help from PIH, the family paid for public transportation for the long ride back home.

Together, in Soledad
The sun dipped slowly behind the lush, coffee-growing mountains ringing Soledad, where children in school uniforms and heavily laden donkeys trudged past Ramirez’s red mud-brick home. The heat of the day was finally relenting on a late afternoon in November.
Ramirez sat on her cement stoop, her long black hair wet and tied back into a ponytail. She balanced one 5-month-old son on each knee. Gabriel and Emanuel wore caps and footie pajamas, both so plump they looked like small Stay Puft Marshmallow Men. Alexis and Yoiner were in constant orbit around their mother, who seemed completely unfazed by their questions and commotion.
One of the twins began to fuss as feeding time drew near. They both slept well, Ramirez said, but Emanuel was “more difficult” than his older brother. Months had passed since those frantic days in April, when she and her husband feared they would lose their twins.
“It was such a dangerous time,” Ramirez said. She thanked PIH for supporting her family through it all. “I don’t know what would have happened.”
The rest of her sentiment—if PIH doctors hadn’t been there—was understood.



