Dr. Michelle Morse: Leading a New Generation of Global Health Clinicians
Posted on Apr 1, 2019
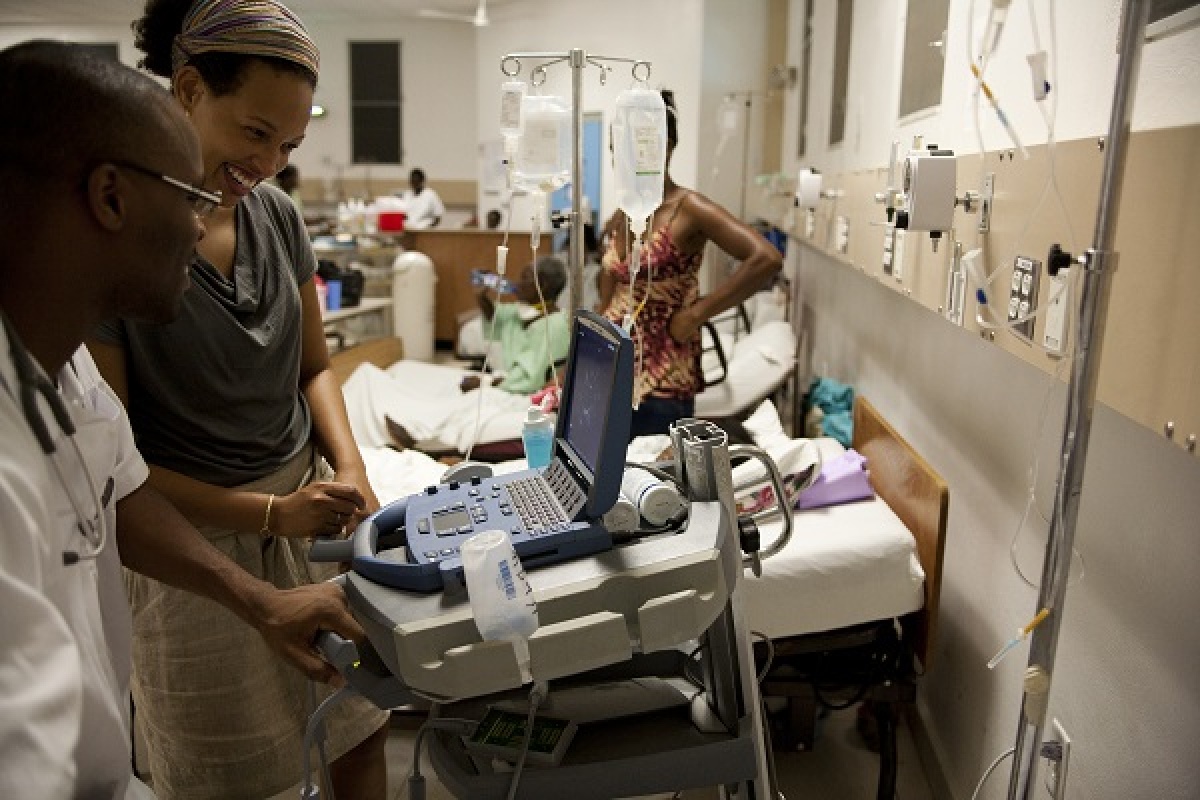
Dr. Michelle Morse is Partners In Health's former deputy chief medical officer and founding co-director of Equal Health. She was among four speakers at PIH's inaugural Evening for Equity on April 2 at the John F. Kennedy Presidential Library and Museum, where she spoke about how history and societal structures influence the provision of health care, and explore the new generation of global health clinicians. Watch a video of her talk HERE.
This story was originally published on January 27, 2014.
Dr. Michelle Morse splits her time seeing patients in Boston and Haiti, working two jobs that each could easily exceed full-time.
But she doesn’t think of herself as remarkable.
Morse, Partners In Health’s deputy medical director for Haiti, believes such global health work should be the norm for American doctors. Like many physicians who commit part of their time to service at PIH, she believes U.S. academic institutions have a responsibility to train health care professionals in poor countries.
“Physicians who choose to work internationally are idolized for their sacrifices and selflessness, but these physicians should not be exalted, nor considered exceptional,” Morse wrote in her application to the global health equity residency at Brigham and Women’s Hospital, a partner of PIH. “International medical work should become the rule.”
Since completing her residency in global health in 2012, Morse has become an attending physician at Brigham and Women’s Hospital, providing hands-on clinical training and mentorship to residents, just as she received from more senior doctors when she was a doctor in training.
In her role with PIH, Morse has helped establish innovative residency programs for young Haitian doctors, in an effort to improve the quality of care in Haiti. When not seeing patients at the Brigham, she’s in Haiti, providing instruction to Haitian residents at University Hospital in Mirebalais, the teaching hospital PIH built in partnership with the Haitian Ministry of Health after the 2010 earthquake.
When PIH co-founder Dr. Paul Farmer began his career in global health at Harvard Medical School and the Brigham, just a handful of his classmates were interested in working internationally. His constant travel between Haiti and Boston earned him the nickname “Paul Foreigner” to his classmates, as Tracy Kidder wrote in Mountains Beyond Mountains.
But today, interest in global medicine is more common, and many medical schools and residency programs offer rotations for students to gain experience seeing patients in poor countries. At Brigham and Women’s Hospital, where Morse works, the global health equity residency prepares young doctors for careers in global health. Still, global health isn’t yet the norm, and what physicians do once they’ve become involved is still a subject of debate, one that Morse hopes to influence.
Confronting an unequal world
Morse is a 32-year-old internist with a warm smile and an easygoing demeanor that wins her trust with patients. She grew up in west Philadelphia, where poverty and violence are epidemic, and saw how social inequalities allowed some people to thrive and caused untimely deaths in others.
“I really felt that it was my responsibility as someone who was educated and had opportunities to make sure that I fought to establish equity instead of inequity,” Morse said.
Her early interest was in domestic health disparities among poor, marginalized people in the United States. In medical school at the University of Pennsylvania, she had her first exposure to global health when she worked in a pediatric clinic in Guatemala. She saw how a lack of public health infrastructure, including access to clean water and sanitation, caused needless diarrheal death in children. She saw simple interventions—such as medications to treat parasites—help young patients.
Morse took a year off from medical school to conduct research on tuberculosis in Botswana. It reaffirmed her interest in global health and showed her that making a difference would require even more of her time and energy.
“I came to understand why weeks or months scattered throughout my career in a non-specific poor country are simply not enough of a commitment,” she said. “I only began to understand Botswana’s specific challenges—and formulate workable interventions—at the end of my year there.”
One day in Botswana she was looking into residency programs that offered global health training and found the global health equity residency at the Brigham.
“I’ll never forget that day,” she said. “I knew I had to do it.”
From world-class to resource-poor
As a global health equity resident with the Brigham in 2009, Morse got to see PIH’s work in Haiti firsthand. She participated in mobile clinics, visited patients in their homes, and saw HIV and tuberculosis patients on rounds at community hospitals.
“I absolutely fell in love with Haiti,” Morse said. “Because I had studied French, I was able to connect with people in a great way.”
The 2010 earthquake destroyed much of Haiti’s already-weak medical infrastructure, including the national medical school and nursing school. It emboldened her commitment to improving Haiti’s health system.
As part of her residency training, Morse worked several months per year in the PIH-supported hospital in Lascahobas, a rural community in the impoverished Central Plateau.
She was surprised to find she had more formal training than all of her Haitian colleagues, both doctors and nurses. In the U.S., a resident is considered a doctor in training, and surrounded by more senior physicians.
The Haitian health care team also worked without diagnostic and treatment equipment considered standard in American hospitals, such as electrocardiogram (EKG) tests to examine a patient’s heart.
Having come from a family of educators—both her mother and grandmother were teachers—Morse began to reflect on the role of education and training in providing quality care. Working with a Haitian colleague, Dr. Pierre Paul, she began to focus on medical education at University Hospital, which was in the final stages of construction.
The hospital promised to deliver the necessary infrastructure—space, electricity, diagnostics, and medical equipment, such as medical gas and operating rooms—for high-quality, complex care. But staffing the facility with trained health professionals would be the next challenge.
In the U.S., teaching hospitals play as important a role as medical schools in educating doctors and nurses to deliver care, ensuring there are enough trained health professionals to meet the needs of the population.
University Hospital was designed to provide similar training, both through continuous educational activities and through new medical residencies, helping to fill a critical gap in trained doctors and nurses. In Haiti, only about half of doctors have any residency training at all. In the U.S., it’s unheard of for a doctor not to have completed a residency.
“You don’t learn how to be a doctor in medical school,” Morse said. “It’s during residency that you dive in and begin to understand what it’s all about.”
Morse and Paul researched residency opportunities for Haitian physicians to determine needs and tapped local and foreign experts to put together curricula. University Hospital’s inaugural residencies would include pediatrics, general surgery, and internal medicine—Morse’s specialty. After a year of planning, the first class of residents began their three to five years of training in fall 2013, and subsequent classes will enroll each year.
After they complete their residency training, Morse hopes some will choose to stay at University Hospital, teaching the next classes of residents, as she has done. Others aspire to bring their advanced training to rural areas of Haiti, where care is out of reach for most people.
Between Boston and Haiti
Today, Morse teaches residents in two disparate places—Haiti and Boston—in facilities that are more similar than you might expect.
One fall day in Boston, she was doing rounds at the Brigham’s Faulkner Hospital, seeing patients with problems that included mental illness and drug dependency. One 92-year-old patient with high blood pressure was feeling better and eager to get home to her yoga and enormous appetite for reading. In Haiti, Morse’s patients are more likely to suffer from heart failure, tuberculosis, and other infectious diseases, and many don’t survive to old age.
At the Brigham, Morse often works up to 70 hours a week. In Haiti, she says, it’s even more. But Morse has found that each position makes her better at the other. And straddling academics and service helps her understand the role of academic institutions like Brigham and Women’s can play in the field of global health.
“I think the two jobs are absolutely synergistic,” Morse said. “I want to help academic institutions understand their responsibility toward the global health community and achieving global health equity.”
From her initial interest in health disparities in her west Philadelphia community, Morse has come to take on disparities globally. And she hasn’t let the problem of whether to work domestically or internationally hamper her commitment to universal access to health care. (Learn more about how to start a career in global health).
“The most important piece is to engage. Whether you do that locally or globally is secondary,” she said.


