PIH Making Strides Against TB, Stigma in Kazakhstan
Posted on Jan 17, 2018
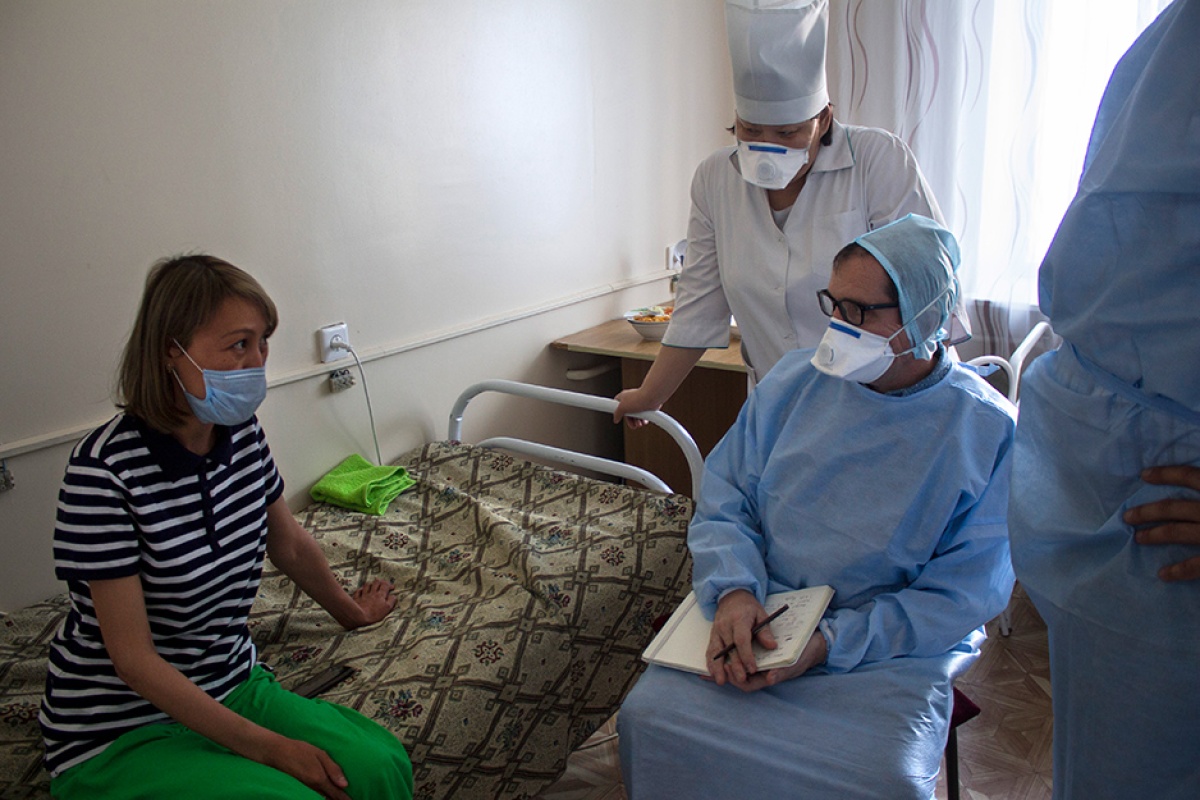
Partners In Health and collaborators are taking big steps forward in the fight against tuberculosis in Kazakhstan, where increasing use of the first new TB drugs in decades, an innovative clinical trial, and digital technologies that better connect patients to caregivers all are raising hopes for more successful treatments.
Strong initial results—meaning, more patients getting better—represent a turning point in the former Soviet republic. Kazakhstan lies in the heart of a Central Asian region where severe, multidrug-resistant (MDR) TB is rampant. MDR-TB is a particularly cruel and hard-to-treat version of TB, which became the world’s deadliest infectious disease in 2015.
Askar Yedilbayev, PIH program director for Kazakhstan and Russia, said more than 6,000 people in Kazakhstan are diagnosed with MDR-TB every year.
All of them face significant societal hurdles when confronting the disease.
Shynar Maretbayeva, PIH medical coordinator and drug procurement specialist in Kazakhstan, said MDR-TB has been so deadly there, for so long, that many people believe it’s impossible to cure—fueling a sense of hopelessness for those who contract it. Stigma about the disease is so deep-rooted in the country that a diagnosis can leave people socially and professionally ostracized, PIH staff said.
That means successful changes to treatment can have magnified, far-reaching impacts in the vast country of more than 18 million people, bordered by Russia to the north and China to the east.
Yedilbayev said he sees huge potential in incorporating bedaquiline and delamanid—the first new TB drugs developed in about 50 years—into MDR-TB treatment regimens in Kazakhstan.
“This is revolutionary, to bring these new drugs to the most desperate patients with drug-resistant TB, and then see their response to therapy,” he said.
PIH’s small Kazakhstan team includes about 20 people, primarily based in Almaty, the country’s largest city. The team is working with Kazakhstan’s government and international aid groups to bolster TB services on multiple fronts, in nine regions across the country. PIH’s work there is supported through two main channels: the Unitaid-funded, multi-country endTB partnership, and USAID’s TB Care II program.
Significant impacts locally could, ultimately, change how the disease is treated globally.
“It’s pretty exciting. We’re really going to change the world with a completely novel MDR-TB treatment,” said Dr. Michael Rich, PIH project co-leader and clinical investigator for endTB.
Local action
PIH is working closely with the Kazakhstan Ministry of Health in its fight against MDR-TB. PIH provides technical assistance and management, clinical accompaniment of Ministry of Health care providers, and more—everything except actual treatment, which in Kazakhstan can be given only by nationally certified doctors.
Expand New Drugs for TB, known as endTB, began in 2015 to foster innovation in places where MDR-TB is deadliest. The $60.4-million project is a partnership between PIH; Médecins sans Frontières; Interactive Research & Development, a global health delivery group; and financial partner Unitaid, a World Health Organization (WHO) partnership that invests in the international fight against TB, HIV, and malaria.
The project aims to enroll at least 2,600 patients in 17 countries on new TB drugs, while meticulously documenting the drugs’ effectiveness and safety, by 2019. Yedilbayev said the partnership had enrolled nearly 1,400 patients across 15 countries as of September, including 320 patients in Kazakhstan.
“Basically, these were all patients that were just incurable,” said Dr. K.J. Seung, co-leader of the endTB partnership.
Those outcomes are changing.
“Many patients who were previously considered untreatable are showing culture negativity, which means they are responding to therapy,” Yedilbayev said.

‘Prepared to die’
One such patient is a 29-year-old Kazakhstan man, given the pseudonym Dmitry Makarov.
PIH data manager and drug safety specialist Yekaterina Sakhabutdinova said Makarov was diagnosed with TB in 2013, after likely contracting the disease at home, from his stepfather. Initial treatments failed because of Makarov’s resistance to first-line antibiotics, and doctors soon gave him a diagnosis of MDR-TB.
Makarov was unemployed, lived with his mother, and had behavioral and psychological disorders along with substance addiction, Sakhabutdinova said. The patient argued with health care workers and resisted the painful, lengthy treatment, which he could not complete before he was discharged from hospitalization.
His condition worsened and his MDR-TB developed into extensively drug-resistant TB, or XDR-TB, an even more severe strain of the disease. By March 2016, the only care Makarov was getting was palliative.
“He was prepared to die,” Sakhabutdinova said.
Regional crisis
Makarov’s case reflects a regional MDR-TB crisis that Seung said goes back decades, and extends far beyond Kazakhstan’s borders.
The fall of the Soviet Union in the early ‘90s undermined state-funded health care systems across the region, drained stocks of medicines, and left countless patients without care, creating conditions that exacerbated a devastating scourge of MDR-TB.
Carole Mitnick, PIH’s director of research for endTB, added that the regional epidemic also “is fueled by the revolving door of the prisons.” Most inmates face extremely crowded conditions that are highly conducive to TB transmission. Inmates who develop active TB upon returning home can then spread the disease there, she said.
Seung said that while, “every part of the world has different sorts of drivers of the epidemic,” prison conditions and recent history in Russia, Central Asia, and Eastern Europe have raised particular concerns in the global health community about MDR-TB in the region.
In its Global Tuberculosis Report for 2016, the World Health Organization (WHO) said about 25 percent of new TB patients in Kazakhstan were diagnosed with MDR-TB, and more than 40 percent of patients who initially were diagnosed with TB then progressed to MDR-TB.
The WHO listed those figures for 30 countries with high burdens of MDR-TB. Among those countries, Kazakhstan’s 25-percent figure was third-highest, tied with Ukraine. The 40-percent figure was the ninth-highest on the WHO list, below neighboring or nearby countries including Uzbekistan, Tajikistan and Kyrgyzstan.
The only country that had a similarly high rate of TB patients who progressed to MDR-TB, but was not in Central Asia or Eastern Europe, was Somalia, at 47 percent.

‘Truly miracles’
To combat the crisis, PIH and collaborators are studying novel treatment methods in Kazakhstan.
Mitnick, also an associate professor of global health and social medicine at Harvard Medical School, said the endTB partnership is tracking a group of Kazakhstan patients, for example, who are taking one of the new drugs as part of the standard MDR-TB regimen.
Mitnick said Kazakhstan also is at the forefront of studying the use of both new drugs— bedaquiline and delamanid— together. She said 80 percent of 15 patients given both drugs tested culture-negative for TB after six months, indicating a strong response to treatment, and did not see worse side effects than what’s common from traditional regimens.
“We didn’t see any increase in toxicity in new patients who got both new drugs, compared to people who only got one of the new drugs,” Mitnick said. “These are really, really sick people, who get both drugs together.”
Seung said doctors treating people for TB usually can see indicators of success, or failure, after six months.
“It’s still a little early, because treatment is long,” Seung said. “But we’re getting some really good results on the first six months. Really, that first wave (of data) is just starting to come out.”
Rich said conversion rates often hovered around 23 percent for patients with XDR-TB, before the new drugs were introduced. He described the new drugs as “truly miracles” for patients who had not responded to treatment with second-line drugs in the past.
Standard treatment can include daily injections for several months and about 14,600 pills over two years, often with grueling side effects.
The endTB project includes a trial of new, shortened regimens that contain one or both new drugs and require no injections. About 750 patients across six countries will participate in the trial.
Mitnick and Yedilbayev said three patients have been enrolled in Kazakhstan since August, on nine-month regimens.
“It’s the first trial that PIH has ever conducted that really holds the potential to revolutionize treatment for MDR-TB,” Mitnick said.
Rich noted that while about 600,000 people around the world contract MDR-TB every year, and while MDR-TB likely kills about 200,000 people every year, “there’s never been a trial to see which (treatment) regimen works better than another regimen.”
There’s an app for that
Kazakhstan’s 320 endTB patients, overall, represent the largest cohort of the 17 countries in the endTB partnership. But that number is still insufficient in Yedilbayev’s view.
"It's not enough—there is a need to scale up,” Yedilbayev said, adding that PIH has a goal of about 600 patients in the country. “The Ministry of Health has agreed to expand access to new regions,” in western, northern, and southern Kazakhstan, he added.
That expansion will have PIH fighting TB in about 65 percent of the country, or across nine of Kazakhstan’s 14 oblasts, which are administrative regions similar to U.S. states.
Reaching patients in all of those areas will be a herculean task. The high numbers of pills and check-ins that MDR-TB treatment requires can create big hurdles for patients, who often can’t travel to see nurses every day and sometimes stop participating in treatment because of frustration, fatigue from side effects, or insurmountable logistics.

Genevieve Roge, cross-site project manager for PIH STRONG—or, Shorter Tuberculosis Regimen and Operationalization of New Guidelines—is supporting the Kazakhstan STRONG team, which is dedicated to addressing that challenge via a common technology: mobile applications.
She said the STRONG project is testing digital technologies in Almaty, including an app that will give patients instant connections to caregivers. The app will enable patients to check in about medicines and treatment without traveling, and get reminders about upcoming appointments.
“I think the most exciting thing for PIH STRONG-Kazakhstan is that we have enrolled 15 patients in this pilot,” Roge said. “It’s very patient-centered, and very user-friendly.”
Roge said the app is intended to make the grueling, nine- to 24-month slog of MDR-TB treatment more bearable.
It also represents a new component of PIH’s longstanding patient-accompaniment ethic, which has defined PIH’s work for years, at sites around the world and in collaboration with national governments. Accompaniment brings health workers to patients’ homes to provide support and monitor progress outside of hospital settings.
Yedilbayev said MDR-TB teams in Kazakhstan, for example, also use customized accompaniment methods such as video-observed therapy—through Skype, Viber, and WhatsApp—according to what works best for different patients.
Personal outreach has been potentially lifesaving for patients including Dmitry Makarov, the 29-year-old man who was prepared to die of his disease.
Sakhabutdinova said the daily personal contact helped Makarov adhere to therapy. He showed significant improvement within three months and is on the way to recovery, she said.
His story is just one example of endTB’s impacts, and of its potential as studies develop in coming years.
Rich cautioned that the first full set of solid data from the new TB drugs likely won’t be ready until 2022. In the meantime, conversations about work in Kazakhstan already are making waves.
“We’re getting so much knowledge from using the new drugs, under World Health Organization guidance,” Rich said, adding that endTB could begin influencing global guidelines as early as this year. “And a lot of that is due to the work coming out of Kazakhstan.”


