Q&A: SE Liberia's Only Surgeon Describes Lifesaving Role(s)
Posted on Aug 27, 2019
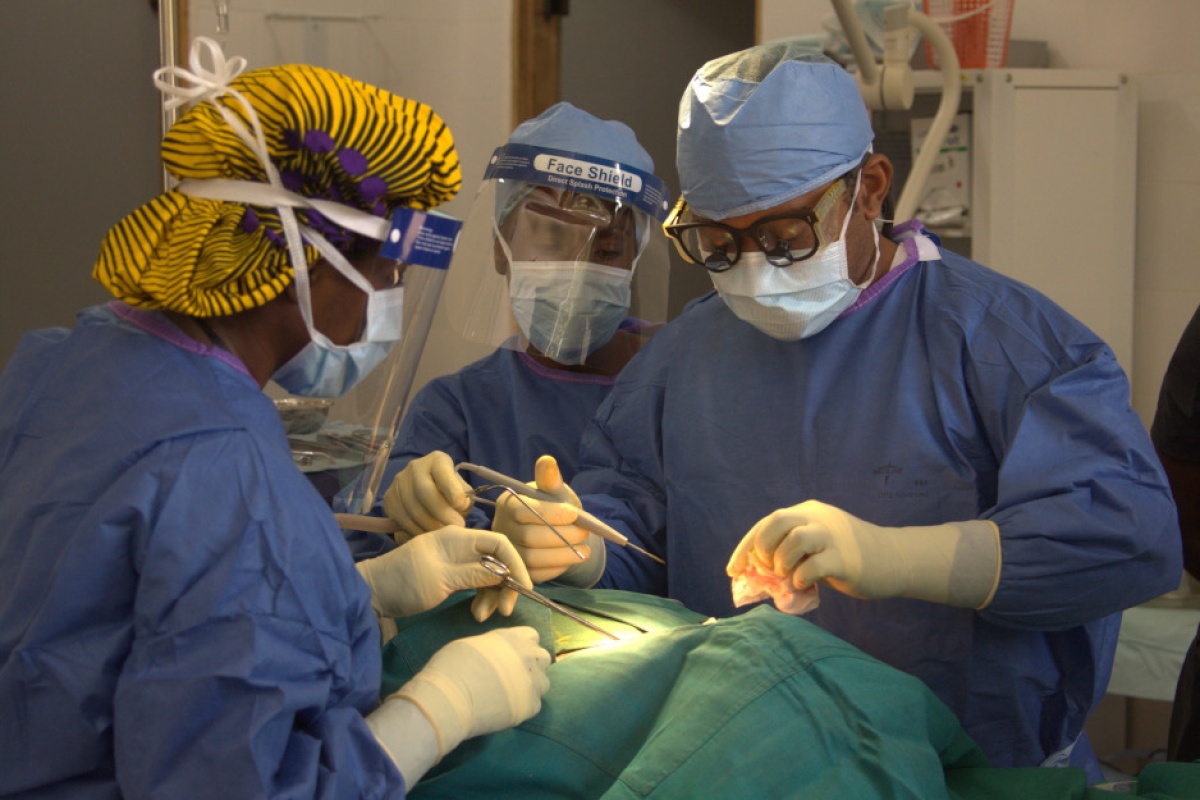
Dr. Gerald Ekwen is not only the sole general surgeon at Partners In Health-supported J.J. Dossen Hospital in Harper, Liberia. He’s also the only surgeon in all of southeastern Liberia, where in Maryland County alone, PIH serves a population of about 170,000.
People also come to J.J. Dossen from neighboring counties and neighboring countries, such as Côte d'Ivoire. Ekwen has boosted obstetric services, too, helping his PIH colleagues track and reduce maternal deaths and increase the rates of women giving birth in a health facility, rather than at home.
PIH’s medical director for Maryland County, Dr. Abdissa Kabeto, said nearly 70 percent of expected deliveries occurred in a health facility in 2018, up from 35 percent just three years earlier—a vital improvement in Maryland, where PIH also supports the Pleebo Health Center.
“The southeast of Liberia is underrepresented and underdeveloped, and requires a lot of support from all of us,” Kabeto said.
Ekwen is an essential part of those efforts. He began his surgical career in 2014 at hospitals in his native Cameroon, and now works with 12 operating room nurses or support staff at J.J. Dossen, performing about 15 surgeries per week. Since Ekwen joined the PIH-Liberia team in 2018, he has conducted about 400 lifesaving surgeries, covering everything from endoscopies to emergency procedures.
His work addresses a need that extends far beyond Liberia. Five billion people worldwide lack access to safe surgeries, according to the World Health Organization. The shortage is most severe in low- and middle-income countries, where nine out of 10 people have no access to basic surgical services.
Ekwen sat down recently to talk about surgery in a rural setting, a daily routine that often extends late into the night, and how he couldn’t find J.J. Dossen’s operating room during an eventful first day on the job.
Why did you become a surgeon?
After working in rural Cameroon for a while, I saw the challenges and burdens of surgical diseases in rural settings. I realized that, to make a difference in people’s lives, I needed to do more than just prescribe drugs. I needed to do surgeries also. That’s what caught my attention and my interest. I saw people suffering from treatable conditions because there was no surgeon.
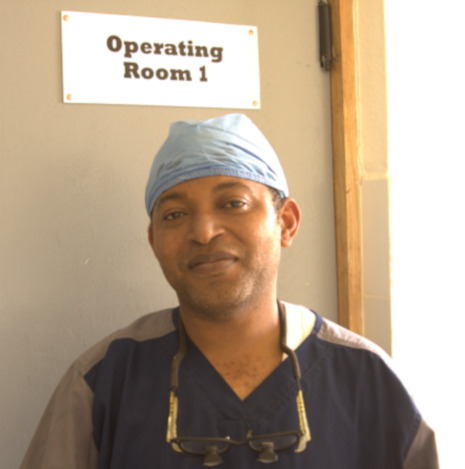
How is practicing surgery in a rural area different from an urban setting?
Here in rural Liberia, you’re expected to work as a urologist, as the orthopedic surgeon, the gynecologist, the obstetrician, and the general surgeon. There are even times when you’re called to do internal medicine and infectious disease care.
Many times, you find that you are alone in terms of support. You have to either connect to others through email or phone to discuss cases. When you work in a city or in teaching hospitals, you have all of these people around you. So when you have a case, you put your heads together and come up with a solution. In a rural setting, there’s no other surgeon, so you have to make the decision.
Working in a place with limited resources, you can make quite a huge difference in people’s lives. If you hadn’t been there, lots of people would have died, or would have had disabilities, because there was no surgeon. You are needed more than in a city.
You’ve certainly been needed, and welcomed, here. What brought you to Liberia?
I had read about the work of PIH in Rwanda and their push for global surgery equity. Our visions intersected in many areas, including the provision of a preferential option for the poor in health care. While reading through the PIH website, I came across a new job listing for Liberia. I saw it as an opportunity to positively impact lives where I was needed most. The opportunity to build local capacity also prompted my interest and, ultimately, my decision.
I hear you had a case from the moment you arrived in Harper. Can you tell me about that day?
In the morning, I was going around the hospital with PIH’s medical director for Maryland County, Dr. Abdissa Kabeto, to introduce myself to the team. We had just finished in the x-ray unit and were in the PIH office in the hospital, talking with another director, when we heard shouts from the ER. We were like, “That is not normal. People are screaming and shouting. Is someone dead? What’s happening in the ER?”
We stepped out to see what was happening, and there was a crowd gathering. We saw a man in a pool of blood, sitting on the floor in the ER. What really scared me was that I had just seen him a few minutes ago in the x-ray room. They said there had been a small explosion, and a piece of metal got into his hand and caused a laceration of his artery.
He was pouring blood, so I had to jump in immediately. I couldn’t allow him to just die in front of me. I compressed the artery and wrapped it in a bandage. But I didn’t know where the operating room was yet, so I asked, “Can you take me to the OR?” We rushed into the OR, and I borrowed some scrubs. They were too big for me, but I just put them on. It was an emergency.
We finally got the artery and bleeding controlled. A major challenge now was how to reconstruct the artery; since I’d never worked here before, I didn’t know what instruments I had, what sutures. So it was a little challenging for me on the first day. But despite the stress and the tension, we composed ourselves, repaired the artery, and saved the life of this patient.
What does a typical day look like for you?
I start around 7:30 a.m. I’m already in the hospital and want to see patients. I begin by going to the ER to get a quick round of what happened overnight and see any patients who came during the night—those having abdominal pain or surgical emergencies that the ER staff have not identified.
Then I do ward rounds. Afterwards, on Mondays and Wednesdays, I go to the surgery clinic, where we see patients for consultations. New patients are first, then we have those who are pre-op, and lastly those who are post-op and coming for review. Tuesdays and Thursdays are mainly elective days.
By 4 p.m., we often start getting emergency cases. For some reason, patients often come later in the day or at night. You see the ambulance start dropping patients. We operate until maybe 9 or 10 p.m. on Tuesdays or Thursdays. Sometimes until 2 a.m., if it’s a particularly complicated patient.
On Fridays, I try to scale down and give some breathing space for the OR team to recover, because obstetrics has a lot of emergencies and cesarean sections on Thursdays.
You have an impressive track record of ensuring safe surgeries at J.J. Dossen Hospital. To what do you attribute this success?
Our team is working hard to make sure our surgeries are safe. Sometimes I see the OR team, after I’m done with a case, sitting there and waiting with a patient. They become the recovery or ICU nurse, sitting there until the patient comes around, before they transfer the patient to a ward. This is making a lot of difference in reducing deaths.
I’ve seen our anesthetist stay with a patient until 2 a.m., sitting with him after a surgery that finished at 9 p.m., giving him fluids and making sure he has oxygen, until he was fully awake and transferred to the ward. Our team follows patients even when they’re on the ward, through phone calls and text messages. All of this is helping to ensure the patient has continuity of care. That is what is making the difference.
Surgery is a team sport. You have to rely on your anesthetist, your scrub technicians. You have to motivate your ward nurses. That is what we can say we are winning on. We’re getting more involved in the management of the patient. Team members begin to feel like it’s our patient. If the patient gets well, it’s our success—not the surgeon’s.
How do you maintain your optimism in the face of difficulties?
Touching and transforming people’s lives, and bringing high-quality health care to those who are truly in need, is a great thing. Many times, all they can tell you is “thank you,” but that’s more than enough. My perspective on life, doing to others what I expect to be done to me, and my deep love for fellow humans all keep me optimistic, in the face of any difficulty.


