Research: Bringing Lifesaving Hepatitis Care To Rwanda
PIH provides new drugs, influences nationwide program
Posted on Jul 28, 2022
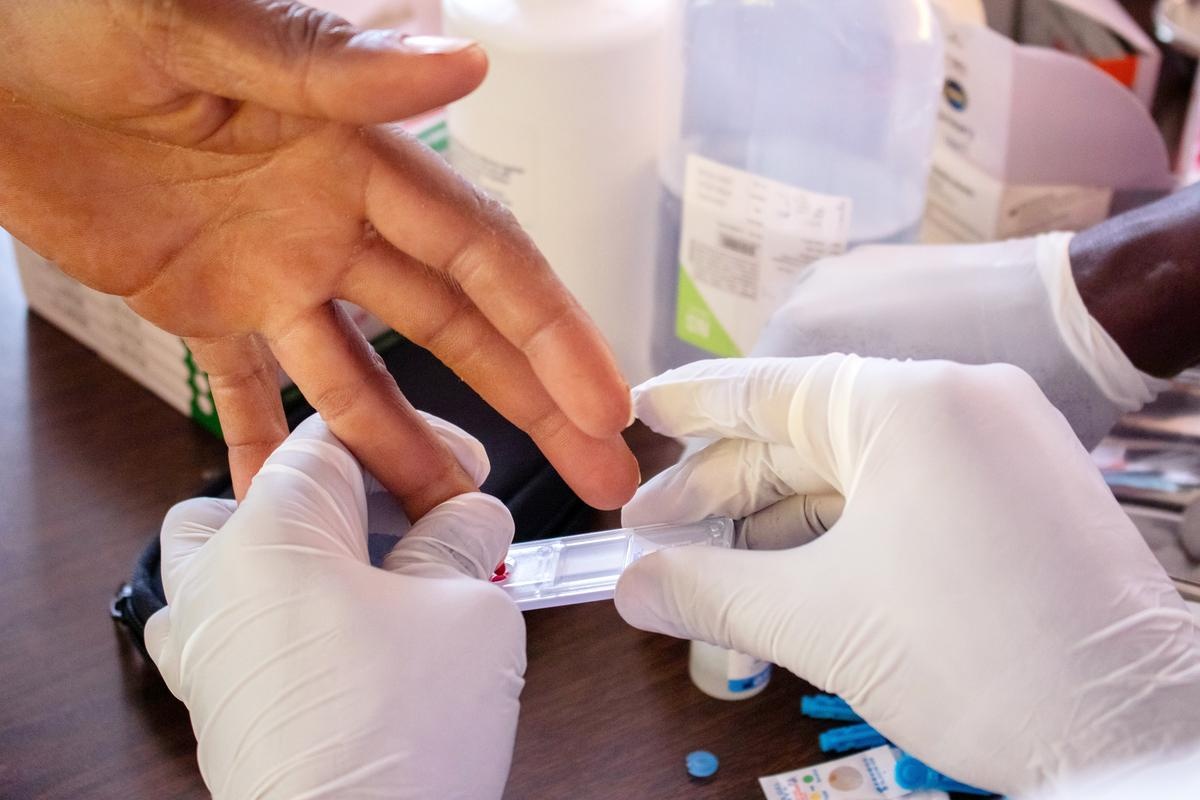
Some got it from needle injuries. Others got it from donating blood. Still others didn’t know the source of their infection. But for years in Rwanda, hepatitis C was a death sentence.
Then, in 2015, a medical breakthrough arrived: a pill that could cure the disease.
“For the first time, there was a bit of hope,” says Dr. Fredrick Kateera, chief medical officer of Inshuti Mu Buzima, as Partners In Health is known in Rwanda.
The pill came to Rwanda through years of advocacy and research by Partners In Health in collaboration with the Rwandan Ministry of Health, the Rwandan Military Hospital, and the Rwandan Biomedical Center—efforts that have since inspired a nationwide hepatitis elimination program and research published in The Lancet.
“During the COVID pandemic, it was easy to forget about the everyday pandemics that were going on in the world,” says Dr. Neil Gupta, former chief medical officer at Inshuti Mu Buzima and faculty at the Brigham and Women’s Hospital in Boston. “Hepatitis is a big one of those.”
Undetected, Undiagnosed
Hepatitis C is as prevalent in Rwanda as HIV, affecting some 3% of the population—but far less funding and resources are directed to the bloodborne virus, which attacks the liver and, in its most severe form, can cause liver damage, cancer, and death.
Most infections occur through unsterilized medical equipment, unscreened blood transfusions, and the sharing of needles among drug users. Often asymptomatic, the virus can go undetected for years, until serious complications arise.
There are no vaccines against hepatitis C, making prevention and early diagnosis and treatment especially crucial. But for years, patients in Rwanda and other impoverished countries had very little access to screening or treatment—even as these resources existed in the United States and other wealthy nations.
Inshuti Mu Buzima and the Rwandan government were determined to change that.
Since 2005, Inshuti Mu Buzima has worked in Rwanda, strengthening the health system and providing medical care in partnership with the Ministry of Health. In the years since, it has expanded its work to care for patients with chronic illnesses. But there was little that could be done for patients with hepatitis C, other than recommend an injection that was too expensive for most to afford and came with painful side effects.
Then, in 2014, a new hepatitis C drug was approved in the U.S., with cure rates approaching 100% for most patients. Kateera and his colleagues in Rwanda took note.
“Like most of our Partners In Health work, we are always interested in pushing the envelope of providing quality care services to people in developing settings,” says Kateera. “So we got wind of opportunities in the U.S. in terms of more modern medications for hepatitis C and we started off by doing some clinical studies.”
Finding A Cure
Those clinical studies began in 2015 and were led by Inshuti Mu Buzima in partnership with the Rwandan Ministry of Health, the Rwandan Military Hospital, and the Rwanda Biomedical Center. The researchers wanted to know if the new drugs were effective among patients with hepatitis C in Rwanda.
The first study, called Shared One, brought pills—taken once daily, for 12 weeks—to hundreds of patients from across the country. And the results were groundbreaking: out of the 300 patients who received treatment, 87% were cured.
“[It] was really like this long-awaited miracle for patients who had liver disease or were diagnosed with hepatitis C, after many years of searching for a diagnosis and having no possibility of a cure,” says Gupta, who co-led the study with Kateera.
Still, some 13% of patients were not cured. Kateera, Gupta, and their team set out to understand why, leading to two follow-up studies with other drugs, which determined for the first time how to best treat these patients, and amassing a body of evidence in support of making the new hepatitis C drugs free and accessible in Rwanda.
The results from all three studies were published in The Lancet, with the most recent featured in June. And the momentum didn’t stop there.
“We were able to take this information and say look, these drugs really need to be available,” says Gupta.
In December 2018, Inshuti Mu Buzima supported the Rwandan Ministry of Health in launching a nationwide hepatitis elimination program, providing free screening and treatment to over 50,000 patients, expanding the health workforce, and capturing data to monitor progress. Inshuti Mu Buzima also organized mass screening campaigns for at-risk populations, including more than 30,000 refugees from Burundi and the Democratic Republic of the Congo.
“This is very much part of the signature contribution of PIH everywhere we work,” says Kateera. “We think of innovative solutions around key major public health gaps and then we iterate and design a program that answers that.”
Showing The World What’s Possible
Dr. Jean D’Amour, director of infectious diseases at Inshuti Mu Buzima and a researcher on the study, still remembers a time when there were just four doctors nationwide following hepatitis C cases. Since the national program was launched, more than 1,000 doctors, nurses, and other health workers now monitor the disease and connect patients with care.
“All of this was designed to help the government and the population in Rwanda, but at the same time to help others in the world, showing them what was possible,” says D’Amour.
Despite the progress that has been made in Rwanda, hepatitis C remains a largely untreated epidemic across Africa, where 8 million people are estimated to be infected but less than 1% have been tested and treated.
In Rwanda, the national program has encountered hurdles, including the COVID-19 pandemic, which forced screenings for the general population to pause. But at-risk patients continue to receive treatment. And Kateera and his colleagues are hopeful that the program will rebuild its momentum. It’s already serving as a model for programs elsewhere.
The impact in health centers and hospitals is tangible, as patients once without treatment now have access to lifesaving pills.
“For the first time, we had an opportunity to access medications that not only could cure you, but could prevent chronic diseases,” says Kateera. “There was a lot more hope.”


