Facing COVID-19, Preparedness is Key in Sierra Leone
Posted on Apr 17, 2020
In mid-March, when Dr. Chiyembekezo Kachimanga stood in front of a hushed crowd of Partners In Health (PIH) staff members and began talking about COVID-19, the disease had not yet made its way to Sierra Leone--but he knew it soon would, and time was short.
“It’s a very difficult pandemic; countries that are richer, that have more resources, are struggling,” Kachimanga said to PIH clinicians, community health workers (CHWs), and administrators, based in the country’s rural Kono District.
“This disease is real, it’s spreading fast, and we are all trying our best so that it doesn’t come to Sierra Leone.”
Known as Dr. Chembe, Kachimanga is PIH’s director of clinical programs in the coastal, West African nation. Sierra Leone, of course, is no stranger to pandemics—the country and its neighbors battled Ebola from 2014 to 2016.
The most recent battle began in early April, when Sierra Leone confirmed its first case of the novel coronavirus—one of the last nations in the world to do so. The news was expected, given that the virus had presented elsewhere in West Africa weeks before. Yet it was jolting, nonetheless, in a country with limited ICU capacity, very few ventilators, and a majority of people whose incomes and lives would be direly affected by the strict social distancing measures seen in other countries.
That’s why Dr. Chembe and PIH’s entire Sierra Leone team stressed preparation and proactive measures from the start, weeks before COVID-19 arrived. In Kono and nationwide, PIH’s efforts have included clinical training and community engagement, system building for specialized triage and isolation at PIH-supported Koidu Government Hospital (KGH) and Wellbody Clinic, long-term ordering of necessary medical supplies, and government accompaniment.
All those measures mean that Sierra Leone, even with its socioeconomic vulnerabilities, is uniquely prepared to halt further spread of the novel coronavirus.
“Though the resources we have are more scarce than other countries’, the steps already taken across Sierra Leone point to how seriously the country takes the outbreak,” said PIH-Sierra Leone Executive Director Jon Lascher. “And for those of us who fought Ebola, the memory of that struggle and the lessons we all learned can help.”
With approaching 30 confirmed cases as of mid-April, Sierra Leone is still in the earlier stages of the global COVID-19 pandemic, though case numbers continue to steadily rise. Throughout the country, the goal has shifted from preventing the virus’ introduction to preventing a serious outbreak. But PIH’s mission remains the same: working with the Ministry of Health to support Kono District and all of Sierra Leone with the resources needed to care for all patients, coronavirus or otherwise.
Training, Information, and Compassion
A foundation of PIH’s COVID-19 response in Sierra Leone is training and education—making sure clinicians, CHWs, and communities have the information they need to protect their health.
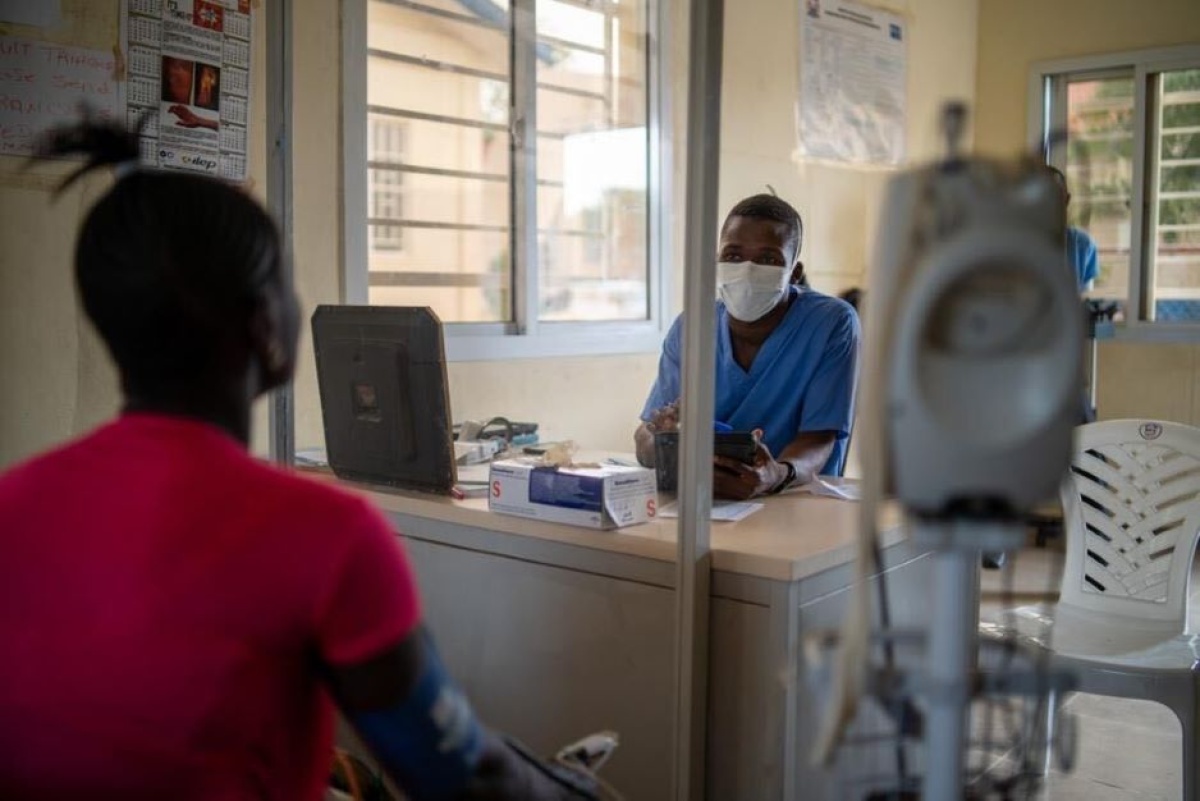
In Kono, PIH is providing coronavirus trainings at KGH and Wellbody Clinic. Clinicians and other health workers know the epidemiology of COVID-19, when to use personal protective equipment (PPE), and how to manage patient care. The trainings are not only about science and health systems; they also are about compassion, as anxiety runs particularly high in the midst of an infectious disease pandemic.
“We are health care workers—we must be examples,” Dr. Marta Patiño, an internist at KGH, encouraged staff during one such training. “This is our role: Kindness. Patience. Information. Empathy.”
Training sessions in communities throughout the district are filling in potential knowledge gaps between households and health facilities. Driving long distances over bumpy roads, PIH staff have been making their way to all 14 chiefdoms in Kono to set up handwashing stations, deliver informational posters, and meet with community leaders on virus prevention methods. These gatherings have been limited in attendance in accordance with national social distancing regulations; the goal is for local leaders to share information with their communities, supplemented by PIH coronavirus prevention broadcasts on Kono radio.

CHWs, meanwhile, have received specific training on how to more safely make their regular home visits and accompany patients to care. New guidelines include meeting with patients outside of homes and using PPE when accompanying people at risk for COVID-19. As trusted sources of health information in the communities they serve, CHWs also have received briefings on how to dispel rumors about coronavirus and, like clinicians, how to help address patients’ fears.
“In situations like this, with a lot of information going around on social media, patients need us to make sure we’re giving them the right information in how they can protect their families,” said Community Based Program Manager Kumba Tekuyama.
And PIH’s impacts are extending far beyond Kono.
Dr. Marta Lado, chief medical officer for PIH in Sierra Leone, recently traveled to Brazzaville, Congo, for a World Health Organization training on COVID-19 patient care. She’s since been supporting Sierra Leone’s government on coronavirus case management and provided training to clinicians at Military 34 Hospital in the capital city of Freetown, where all of the country’s coronavirus patients are being monitored and treated.
Strengthening Sierra Leone’s National Response
Lado remains at Military 34 Hospital this month, as one of the clinicians caring for the country’s handful of patients who’ve tested positive for coronavirus. None of them are in critical condition.
“All are doing amazingly well,” she said. “Most of them are completely asymptomatic.”

For now, all positive COVID-19 cases are being transferred to Freetown, and national mandates—border closures, a three-month shuttering of Sierra Leone’s airport, and periodic countrywide lockdowns—are aiming to control the potential spread of the virus. Plans for additional treatment centers, for both mild and severe cases, are in the works.
“Mild cases have no need to be receiving hospital-level care, but we have to set up some facilities where those patients can be separated from the community while they are infectious,” Lado explained.
She added that severe cases, meanwhile, will be taken to “treatment centers with modern technology and all the systems we need to deliver critical care to the 5 or so percent of people who are going to get quite sick.”
As Lado helps inform infection prevention and control strategy for the government, PIH is also represented at national- and district-level Emergency Operations Center meetings run by the government.
“Feedback and engagement with the Emergency Operations Center helps embellish and feed into our PIH preparedness plan,” said Momoh Jimmy, director of government relations for PIH-Sierra Leone, one of the staff members ensuring a symbiotic relationship between the national response and PIH’s. “Coordination here and with the Ministry of Health ensures our plan is aligned with government priorities and international standards in the fight against COVID-19.”
As government response efforts feed into PIH’s, the organization offers technical assistance in areas like clinical training, contact tracing, and supply chain, as well as other granular forms of assistance. A PIH driver, for instance, recently took Ministry of Health officials around the country to inspect health facilities’ isolation capacities.
Triage, Testing, and Treatment in Kono
In Kono, KGH had seen three suspected coronavirus cases by early April, but all had tested negative. PIH’s work has focused on preparing supply chains and essential triage and isolation systems, in case of community transmission and a resulting outbreak in the rural district.
Aligning with national protocols, staff at the hospital and at Wellbody have set up a separate triage system for all patients with COVID-like symptoms, who will be admitted in an area that’s separate from other patients, then isolated and tested for the illness. Patients who test negatively remain at the facility for care, while patients who test positively are taken in an ambulance to Military 34 Hospital, in order to contain the disease’s spread as much as possible.
Both PIH-supported facilities recently have seen reductions in the number of patients arriving for care—indicative of patients’ fears, with roots in the Ebola epidemic, of health facilities during the time of a potential epidemic. But with more community education efforts, and the continuation of quality essential health services and accompaniment from CHWs, staff expect patient attendance to soon return to its usual high level.
PIH’s supply chain team has been placing orders with that in mind. Since the majority of medical supplies, equipment, and drugs are shipped to Sierra Leone from other countries, the global COVID-19 pandemic poses threats to all forms of health care. Shipping is limited and more expensive, and items as simple as surgical gloves and aspirin are increasingly unavailable.

But Sierra Leone, luckily, is equipped with comfortable amounts of PPE that are left over from the Ebola outbreak. And one of the first measures in PIH’s COVID-19 response was to order of six months’ worth of stock for pharmacy shelves, surgical trays, and supply closets, for the treatment of coronavirus or any other illness.
Indeed, maintaining routine health services is a key aspect of PIH’s COVID-19 response, as an unintended global consequence of the virus could be diverting resources away from non-COVID health areas in need of equally urgent attention.
“We are committed to making sure our patients have access to the same services they had before coronavirus,” Lascher said.
Tekuyama echoed this message on behalf of PIH’s force of CHWs.
“We’re still going to continue with patient care—because I feel like patients need us even more now,” she said.
As COVID-19 is proving to be not just a new, emergent health problem, but also a reminder of the necessity of holistic health system strengthening, PIH-SL is working hard to ensure every Sierra Leonean’s right to health care.
In one of his recent trainings, Dr. Chembe stressed that message—and the necessity of direct, compassionate measures—to a crowd of community health workers.
“I want you all to be doers of these things,” he said. “If you are doers, you protect yourself, your family, and the community.”


