The Road to Safer Childbirth in Sierra Leone
Ambulance referrals are connecting pregnant women to emergency care at the newly opened Maternal Center of Excellence in Sierra Leone.
Posted on May 12, 2026
Before ambulances became widely available in Sierra Leone, pregnant women experiencing emergencies often faced impossible choices about how to reach care.
In remote places, some women traveled for hours over rugged dirt roads by taxi or motorbike while in labor, others walked. For women experiencing complications during childbirth, those delays could be deadly.
By the time an expectant mother reached a clinical facility, her condition would likely have deteriorated. And, worse still, the challenges to receive care often continued: facilities outside of Partners In Health’s (PIH) network sometimes charge a fee for basic lifesaving services, such as blood transfusions.
At PIH-supported clinics, free health care services have been provided since 2014, when PIH began working in the country. Still, accessing care during emergencies remained challenging for those living in hard-to-reach areas for several more years.
Ambulances begin a new era of care
Twenty years ago, Sierra Leone was the deadliest place in the world to give birth. Women died from hemorrhage, preeclampsia, and obstructed labor. While the country’s maternal mortality rate has fallen dramatically in recent years, lifesaving maternal care depends not only on skilled clinicians and operating rooms, but on whether patients can safely reach them in time.
In October 2018, a national network of ambulances began operations.
The initiative, led by the National Emergency Medical Services (NEMS), operates in every district in the country. PIH Sierra Leone directly supports the work in Kono District.
“There’s a huge difference between 2018 and now,” says Joyce Senesie, regional operations coordinator for NEMS. “Since the intervention of the ambulance, we've reduced maternal death.”

The number of emergency referrals to PIH-supported Koidu Government Hospital (KGH) quickly increased after the ambulance service launched. Renowned for its quality of care, KGH, located in rural Kono District, provides free health services for patients that come from around the country as well as neighboring countries, Liberia and Guinea.
Ambulances meant faster and safer emergency transportation. In 2025 alone, ambulances brought 562 pregnant women to KGH. Today, these ambulances are still pulling through the same gates they always have at KGH, only now, they turn toward the newly opened Paul E. Farmer Maternal Center of Excellence (MCOE), a cutting-edge maternal and neonatal referral facility built on the hospital’s campus.
On Feb. 14, 2026, the MCOE opened its doors to its first patients—and that afternoon, the first ambulance arrived at the facility carrying Sia Jimissa, a 33-year-old pregnant mother of three.
Referrals save lives
Throughout her pregnancy, Jimissa attended prenatal appointments for routine care at her local clinic—approximately a two-hour drive away from KGH. On the morning of Feb. 14, she began experiencing contractions and went to her clinic to give birth as planned. However, after three hours of labor there, the clinical staff identified complications and called an ambulance to refer Jimissa to the MCOE.
Like many women across the world, Jimissa had expected to deliver close to home, surrounded by familiar staff and loved ones. But when complications arose, she needed access to surgical care that her local clinic could not provide. Staff at her clinic were well-trained in how to refer her case.
They called a central ambulance dispatch center. And as they waited for the ambulance to arrive, called the maternity team at the MCOE to share the reason for Jimissa’s referral; important medical details that would enable the team to dive directly into administering appropriate care once she arrived.
“From the caller to the dispatching of the ambulances to the maternity team, they are always ready to receive emergency services,” says Senesie. “They know how to identify dangers, and they know where to stop and [refer].”

For Jimissa, the referral was unexpected. She later described feeling frightened that her labor was no longer progressing normally, and anxious about being transferred to a hospital she had never visited before. Jimissa boarded the ambulance alongside her elder sister.
It was one of five stationed across Kono District, which serve the entire district and are linked to PIH-supported health centers, such as KGH and the MCOE.
Upon arrival at the MCOE, all patients go through a triage process, whereby clinical staff quickly assess a patient’s needs to identify the next steps and prioritize emergencies.
“These sometimes can be really hard decisions. Because you can have a baby that is in real fetus distress, but another one that is actually the mother [in distress], so you're having to constantly decide,” explains Isata Dumbuya, director of nursing and midwifery for the reproductive, maternal, neonatal, child and adolescent health program at the MCOE.
The triage team determined that Jimissa had prolonged labor and that her baby was in distress. She was moved swiftly to an operating theater.
Ending preventable maternal deaths
The MCOE has three operating theaters built for advanced surgical care. There, Jimissa underwent an emergency C-section with no complications, and she delivered a healthy baby boy.
For years, the delay between a clinician identifying the need for an emergency C-section and actually performing one could stretch dangerously long. But today, ambulance referrals, improved coordination, and immediate access to operating theaters at the MCOE are helping reduce those delays dramatically.
Ambulances play a key role in getting women like Jimissa from distant communities to care quickly. Equipped with four-wheel drive, the vehicles are designed to navigate uneven terrain. To ensure 24/7 availability, each ambulance has a rotating staff of three drivers and three paramedics—all of whom are trained to handle a delivery that happens en route to the hospital.
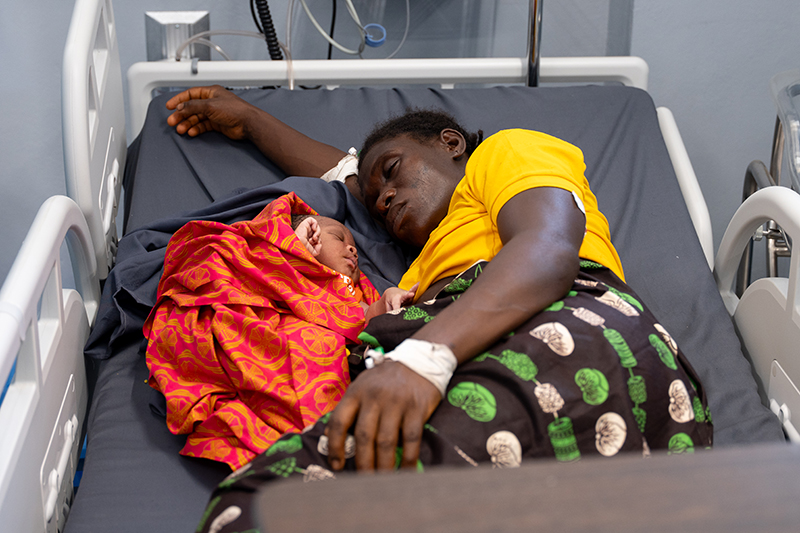
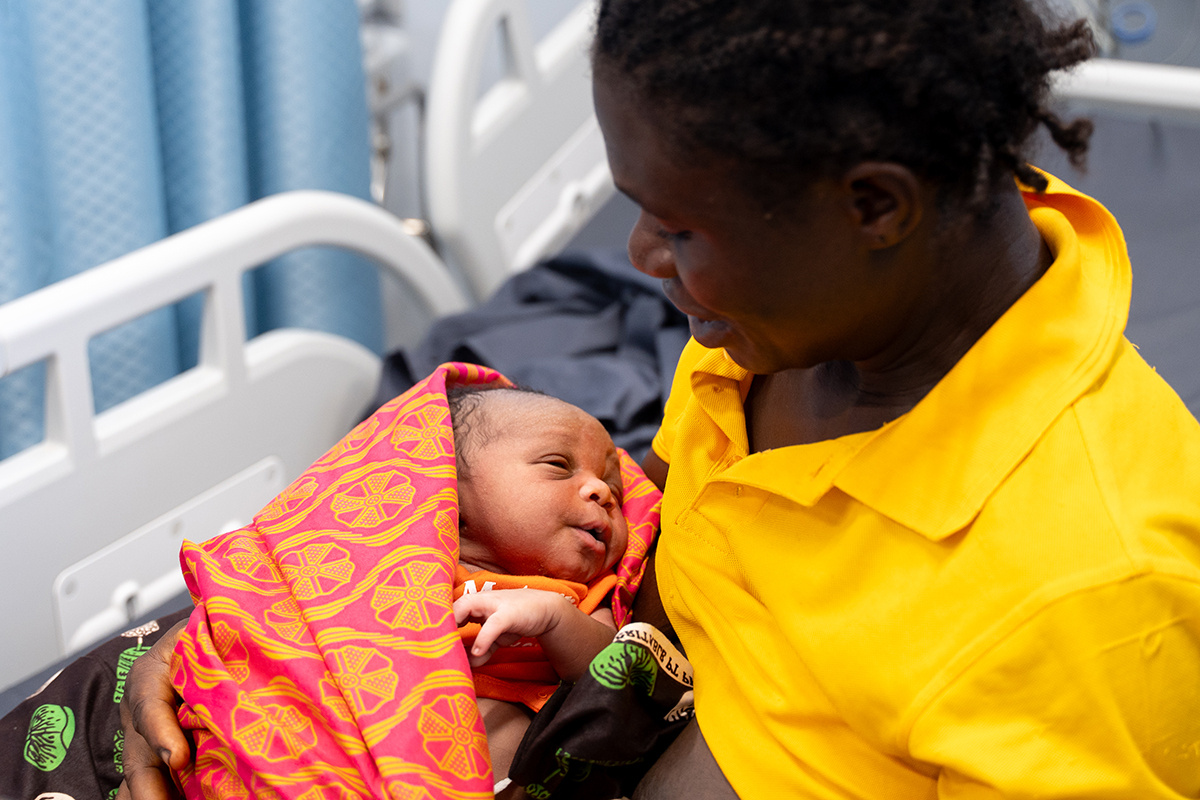
Jimissa’s son was among the first babies born at the facility. As of May 1, there have been 901 babies delivered and 2,871 women have received care at the MCOE.
“We should have zero preventable maternal death, zero preventable newborn death,” emphasizes Senesie. “And with NEMS and the MCOE, I believe we can achieve it.”
In 2025, improved ambulance availability resulted in a 5% increase in referrals through NEMS, and will likely increase this year because of the MCOE.
While Senesie’s primary job responsibility is to provide timely coordination and support for health care staff, it also involves collaborating with expectant mothers in remote communities.
“Our role is not only to dispatch an ambulance, but to make sure that the people know about the ambulance service,” says Senesie.
Despite challenges such as vehicle maintenance and fuel availability, the team’s dedication ensures that women and their families know services are free and accessible.
‘Every one minute is very important’

KGH has long been a vital referral center for high-risk pregnancies and obstetric emergencies. Now, the MCOE is raising the standard of maternal heath in Sierra Leone even higher.
The MCOE radically increased the size and sophistication of KGH’s maternity ward and special care baby unit, expanding it from 48 beds to 120 beds, including a cutting-edge neonatal intensive care unit, the first in Sierra Leone.
Within the first two weeks of opening, all the hospital beds were full.
“No matter what you do, you can never plan enough for these sorts of things,” reflects Dumbuya. “We continue to adjust and change things to ensure that every woman that comes in, every parent, every father that comes in, and every baby that is born here gets the quality and standard of care that they deserve.”
As the team refines protocols, they’re actively improving the referral process in collaboration with NEMS—specifically sorting out roundtrip transportation for women after they’re discharged.
A facility like the MCOE can only function effectively when strong referral networks are in place—and when timely emergency resources, like ambulances with well-trained staff, are available.
Across Kono District, women like Jimissa—who once may not have survived obstetric emergencies—are now reaching advanced maternal care in time. The ambulances represent a rapidly strengthening system of care designed to ensure that childbirth is dignified and no longer a life-threatening gamble.
“For pregnant women, every one minute is very important,” says Senesie.


