Transcending COVID-19 Through Investment in Mental Health
Caring for Ourselves, and Each Other, on World Mental Health Day 2020
Posted on Oct 9, 2020
Dr. Giuseppe (Bepi) Raviola, director of mental health at Partners In Health, shares below how PIH has invested in and incorporated mental health into COVID-19 care around the world, and reflects on the importance of self-care during moments of stress and crisis.
October 10, World Mental Health Day 2020, is this year dedicated to “Mental Health for All—Greater Investment—Greater Access. Everyone, everywhere.” It comes during a year like no other. For many people, it has added the highest levels of stress, strain, and trauma they have ever experienced. The current moment calls for each of us to take individual steps to buffer our mental health, and to together stand up for greater investment in mental health, wherever we live.
Major public health challenges, climate change, racial and political justice movements, as well as the complex evolution of our use of technology are converging now to challenge our conception of “mental health.” Pandemic anxiety takes many forms–physical, emotional, cognitive, spiritual, and existential.
How do we intervene with the stress we are experiencing, and that embedded threat response?
We are each managing our own very personal manifestations of acute and chronic stress that dig deep into our biology, and trigger both our innate and unique threat responses. This is overlaid on our past life histories and experiences, which have already been embedded physically and psychologically, and in the ways that we live our day-to-day lives. For some people, the threat response can inspire constructive action and even inspiration. For some it can evolve to a state of depression. And for others, it can unfortunately increase the capacity for violence.
With personal, professional, political, and economic norms so challenged, we’re justified in this moment to have a sense of existential crisis as individuals, communities, and as a species.
How do we intervene with the stress we are experiencing, and that embedded threat response?
Self-Care in Crisis
Mental health interventions include not only biological treatments for mental illness, which do have efficacy, but more importantly encompass the various attitudes, practices, and "interventions" that we each choose and commit to as individuals living within a broader ecosystem of family, friends, local community, and the natural environment.
I’d like to take the opportunity to share with you some points for optimism, both with regard to the steps we personally can take during this difficult time, and also from the perspective of what can be accomplished in the delivery of mental health care.
On the personal side, each of us—without training in formal mental health treatments—can learn to effectively deliver basic components of interventions to others, and to ourselves; these can be spiritual, physical, psychosocial, and psychological. Many different kinds of interventions, including meditation, yoga, acupuncture, exercise, and time outside in nature, have been proven scientifically to be beneficial for our mental health.
There are little things that we each can do to advance our well-being, starting with simply breathing and putting one foot in front of the other.
One particular psychological treatment delivery model, the Common Elements Treatment Approach (CETA), crystallizes evidence on best practices to address a variety of problems. CETA is a proven and innovative approach that addresses substance use, violence, and mental health problems (such as depression, anxiety, trauma, and aggression) in a single intervention. It is comprised of nine highly studied and effective elements: engagement and education about the problem; thinking in a different way; engaging in activities you enjoy; confronting fears and trauma memories; maintaining safety and self-care; substance abuse prevention and intervention; problem-solving; and anxiety management. The World Health Organization has also endorsed several other approaches that are comprised of similar basic psychological and psychosocial skills, proven by research, and implementable in communities.
The variety and robust evidence for these interventions should give us a tremendous sense of optimism. We don’t necessarily need a mental health professional to cope better. We don’t have to have a degree to be helpful to ourselves or others, and a person doesn’t have to have a mental health “problem” to take advantage of these tools. Not everyone needs “mental health care” packaged as a clinical service. There are little things that we each can do to advance well-being, starting with simply breathing and putting one foot in front of the other. The effects of these small personal transformations can ripple to positively impact our children, partners, families, friends, and colleagues—in person, by phone, or on Zoom.
Investing in Global Mental Health
However, we’re still left with a global gap in the dissemination and sustained availability of all of these kinds of tools and interventions. There are various reasons this is true, including:
- limited budgets to support mental health specialists,
- few non-specialists trained and supported to deliver mental health care,
- limited management capacity for training and long-term supervision,
- a lack of adequate primary care to back community-based mental health care and support delivery for more complex situations
This is why investing in mental health is now so important.
We hope that PIH’s approach to delivering mental health care can serve as a point of hope, that provision of care and support is doable in all contexts, relevant in all contexts, and that it’s a worthwhile investment. The kind of work that we do is not simple; however, it is not overly complicated—or expensive—either. While COVID-19 is changing the landscape of health care delivery, now is the time to look at what works, and commit greater resources to delivering mental health care and support to diverse populations.
Over the past decade, Partners In Health’s cross-site mental health programs have prioritized the direct care of people living with mental health conditions, and have served as a real-world example of what can be accomplished when small investments are made in mental health care.

The shocking and difficult experience of scrambling to develop an organized mental health response to the 2010 Haiti earthquake and to the 2013 to 2015 Ebola crisis in West Africa clarified for us the need to develop a clear strategy for cost-effective mental health care delivery that wouldn’t leave us as exposed to the inevitable trauma of these and other unexpected events. In essence we’ve tried, at an organizational level, to put one foot in front of another in the face of huge challenges and burdens from humanitarian disasters and a significant burden of illness in the communities we serve. Incredible progress has been made. Over the last year, for example, more than 104 PIH-supported facilities delivered mental health care, more than 65,000 facility-based mental health visits were made, and more than 12,800 people were treated for mental health conditions across PIH global sites.
Adaptation in the Time of COVID
Over the past several years, our global sites have been collaborating to expand the availability of psychological and psychosocial mental health care and are now prepared for exactly the kind of crisis we now face with COVID-19.
Each site has responded decisively and creatively, with a number of innovative new initiatives. Socios En Salud, as PIH is known in Peru, for example, developed a cell phone-based digital technology, a chatbot, through which people are screened and linked to support, if needed. The chatbot is being piloted and scaled up nationally in partnership with the Ministry of Health. The team adapted the chatbot into Quechua to increase access to essential mental health services.
Following PIH’s engagement with the Commonwealth of Massachusetts in developing the Community Tracing Collaborative, our mental health team encouraged an aggressive approach to training in Psychological First Aid for contact tracers so that they could effectively deliver support and address the mental health needs of contacts and people affected by COVID. Early on, we observed that some contact tracers themselves were enduring significant distress supporting people remotely, as high levels of trauma, economic challenge, and personal loss faced by people affected by COVID were naturally transmitting to the contact tracers. Support groups were developed for the contact tracer corps, and a contact tracer peer manager was elevated from that corps to develop a team of peer support specialists for the program.
Meanwhile, PIH global sites were increasingly expressing concern about the significant distress faced by health care providers whose colleagues and themselves were contracting COVID-19. The peer support model developed in Massachusetts, which benefited originally from the PIH global experience, is now being re-adapted back to the global sites, starting with Lesotho and Malawi, for the purpose of supporting health care workers in distress.
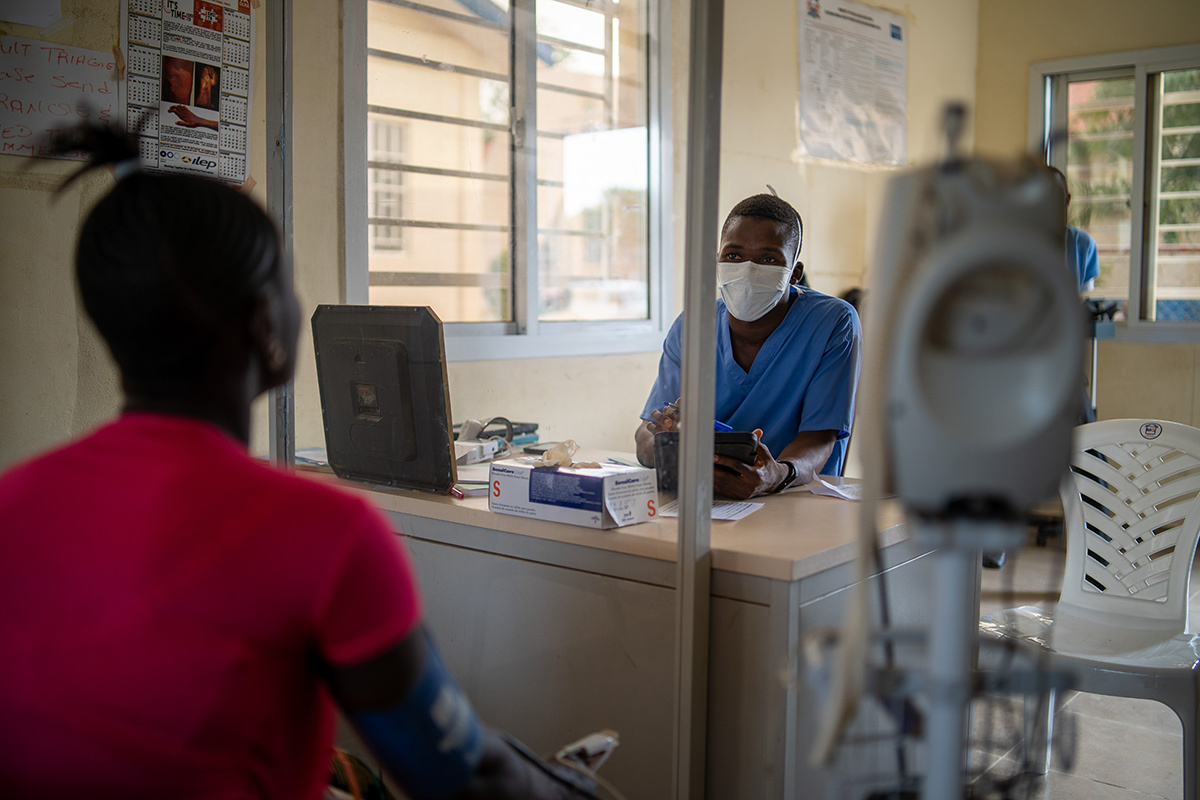
Protecting the mental health of our health care providers, who make essential sacrifices every day, must remain a priority.
Envisioning Improved Care
Taking all this into consideration, this is what I would ask of you on World Mental Health Day 2020:
- Take a moment to define for yourself what it means to have good mental health in the current context of rapid and disruptive social change
- Consider what the future of mental health care in society should look like
- Commit to talking about mental health with friends, family, and colleagues
- Push for the political will and change needed where you live to build mental health practice, services, and programs to meet the challenges of the present—and to come
At PIH we talk about “solidarity” in our work as an acknowledgement of a shared commitment to peace, social justice, and equal human rights—including in health—in the face of poverty, structural and actual violence, natural disaster, and political upheaval. If the effects of historical and psychological trauma have become more apparent through the current COVID-19 crisis, then it must be met by a shared vision for mental health care and support to ameliorate the situation for all. We will continue to work toward this goal, and access to quality mental health care for everyone, everywhere.


