Celebrating Game-Changing Accomplishments at University Hospital in Haiti
Posted on Jan 13, 2020
Nearly seven years have passed since University Hospital in Mirebalais opened its doors and began transforming health care for more than one million people across Haiti's Central Plateau. Since March 2013, thousands of patients have had access to specialized care provided by clinicians working with Zanmi Lasante, as Partners In Health is known locally.
University Hospital has also been home to a growing medical education program, which has graduated 123 residents from a variety of specialties, including emergency medicine, surgery, and pediatrics, to add to the growing health care workforce in Haiti.
For a deeper dive into University Hospital's many accomplishments, check out the below image, a bird’s eye view of the campus. Hover over various sections to learn more about how hospital staff save lives every day by providing high-quality care to all patients, regardless of their income.
A Safe Haven for Mothers and Babies
When University Hospital opened in 2013, staff frequently saw full-term pregnant women sleeping overnight on cement sidewalks waiting for labor to begin. Many of them lived far from care and wanted to be near the hospital as their due date approached. Mothers of babies in the neonatal intensive care unit also slept outside to be available for feedings. These everyday scenes were a testament to the mothers’ determination to receive high-quality care for themselves and their newborns. They also were the inspiration for Kay Manmito, the maternal waiting home PIH built on the grounds of University Hospital.
Kay Manmito, or “Mother’s Home” in Haitian Creole, hosts women with complicated pregnancies and mothers of premature and NICU infants, guaranteeing them a facility-based birth and providing them with free prenatal care, meals, psychosocial support, and health education. In 2019, Kay Manmito housed 378 women so that they could receive the lifesaving, dignified care they needed, from blood pressure monitoring to C-sections. These patients were among the 15 women, on average, who delivered each day in the neighboring hospital’s maternity ward. For expectant mothers like Natacha Jean Paul, whose risky pregnancy brought her to the facility, “the care found here is priceless.”
Training Haiti’s Next Generation of Clinicians
Brain drain has long stymied Haiti’s health care system. Doctors and nurses have historically had few options for specialized training within the country, and 80 percent of those who do train in Haiti leave within five years of graduation to practice abroad. The few clinicians with specialized training who remain in Haiti typically work in the capital of Port-au-Prince, far from where most patients—particularly the rural poor—can access care.
Medical education is integral to University Hospital, which was built as a teaching facility where Haitian clinicians could train in advanced specialties. Since opening, the hospital has begun offering residency programs in pediatrics, surgery, obstetrics and gynecology, neurology, nurse anesthesiology, and family, internal, and emergency medicine. To date, 123 clinicians have graduated from these programs, including the family medicine residency at PIH-supported St. Nicholas Hospital in St. Marc. Nearly 98 percent have chosen to work in Haiti and 60 percent with PIH-supported facilities, strengthening local health systems and caring for the most vulnerable patients.
Cancer Care for All
Cancer affects people around the world proportionately, yet access to treatment is disproportionate, as lifesaving chemotherapy and surgeries are often unavailable or inaccessible in poor countries. University Hospital’s oncology department is changing this reality. There, patients from across Haiti receive the diagnoses, specialized care, and psychosocial support they need to survive.
Last year, University Hospital provided cancer treatment to 652 patients, the majority of them women with breast cancer. Cita Cherie* is one such patient: She has been receiving palliative chemotherapy for an advanced stage of breast cancer since the hospital opened. “If it were not for the Mirebalais hospital, I would not be alive today,” Cherie says. “I get all my medication for free, and when I come to the hospital, the doctors take really good care of me. They welcome me and they really value me.”
*Name has been changed at patient’s request.
A Lifesaving Laboratory
The Stephen Robert and Pilar Crespi Robert Regional Reference Laboratory, which PIH opened in 2016 across from University Hospital, has transformed health care for more than 1 million people. The 15,800-square-foot facility contains a clinical lab, a pathology lab, and Biosafety Level 2 and 3 laboratories, allowing staff to quickly and confidently diagnose and monitor infectious diseases and noncommunicable diseases like cancer. Highly trained technicians use advanced tools to improve the quality and timeliness of diagnostic services, meaning more patients receive better care in less time.
Rehab for the Body, Mind, and Spirit
The Center of Excellence in Rehab and Education is the first public facility of its kind in Haiti. Here, patients from all walks of life come for outpatient physical therapy sessions, and a select few remain for extended stays to recover from trauma. They are stroke survivors and amputees, accident victims and people living with various forms of disability. They come for physical transformation, and often leave with a mental and emotional lift as well.
Staff and patients interact in one of the most pleasant spaces on the University Hospital campus. The L-shaped facility fills with natural light and bright tile mosaics decorate the walls, some with Haitian proverbs worked into the design. One, appropriately, says: “Piti piti zwazo fè nich li,” or “Little by little the bird builds its nest.”
A Hub of Activity
University Hospital’s emergency department buzzes with activity. The suite of rooms rarely has an opening in its 16 beds, and two rows of chairs regularly fill with awaiting patients. Renovations are currently underway to expand the space to 36 beds and add on bathroom and shower facilities for patients on longer stays.
There are the typical emergencies, from broken bones and lacerations to heart attacks and motorcycle accidents. But there are just as many patients who come following acute episodes spurred from chronic illnesses, such as diabetes and heart failure.
The emergency department is often the first stop for University Hospital patients, who come from across the country at all times of day. They are greeted by seasoned clinicians and medical residents on rotation through the ward. So far, 16 emergency medicine residents have graduated from the program since its launch in 2013.
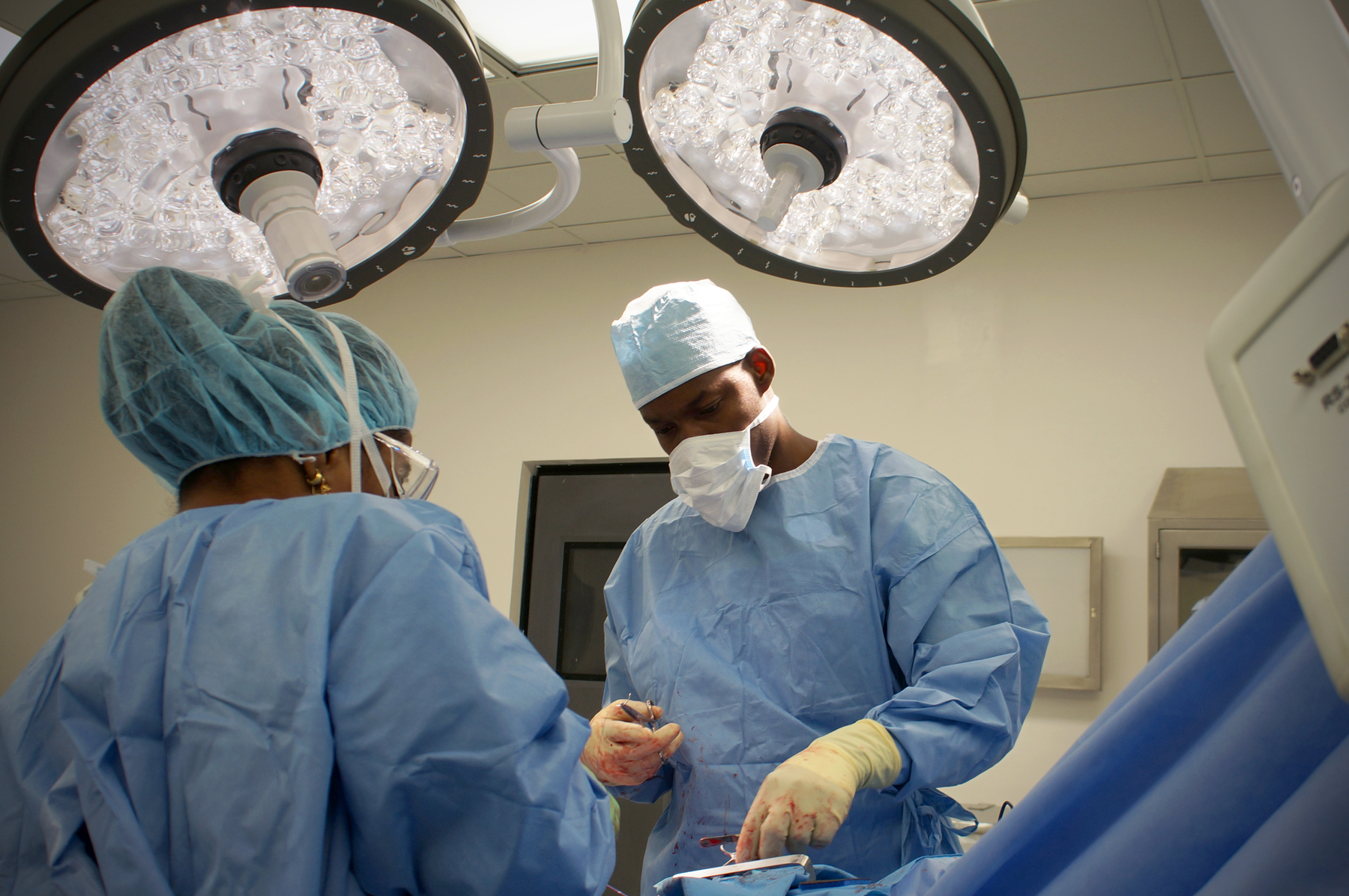
A Cut Above the Rest
University Hospital is home to six state-of-the-art operating rooms, tucked away in the heart of the facility. In 2018 alone, surgeons performed 1,666 lifesaving cesarean sections and more than 600 other women's health-related procedures, such as hysterectomies.
The operating theater hosts routine surgeries, such as appendectomies and the removal of tumors. It has also hosted teams of international surgeons who, in collaboration with PIH clinicians, have conducted cleft palate repairs and—most impressive of all—the separation of conjoined twins.
So far, 19 surgical residents have entered University Hospital’s medical education program, six of whom have graduated so far.
Always a Full House
In the pre-dawn hours, dozens of patients begin arriving at University Hospital’s main entrance to await their turn for high-quality care, at little or no cost. Last year, clinicians conducted nearly 182,290 outpatient visits and admitted close to 4,320 patients, many of whom had traveled hours to be seen by the facility’s top-notch doctors and nurses.
Once patients have registered and had their vitals taken, they sit in one of several waiting rooms for their name to be called. They come for consultations with maternal and mental health, dental services and radiology, oncology and chronic diseases. Those who are admitted may end up in a number of departments, such as labor and delivery, pediatrics, or isolation—should they be diagnosed with an infectious disease, such as multidrug-resistant tuberculosis.
Regardless of why they come, they will receive care within specialties that would otherwise be out of reach for the rural poor across Haiti.


