Major Milestones in PIH History
A timeline highlighting key moments from the past three decades
Posted on Feb 21, 2022
Three decades ago, Partners In Health was formed to support the work begun in a small, rural community called Cange in Haiti’s Central Plateau. From there, it expanded across the country, then on to Peru and Russia, across Africa, and on to Mexico and the Navajo Nation.
Through it all, PIH has kept patient care at the center of its work and fought for health care as a human right—both within individual countries and the halls where global health policy is created.
In the timeline below, read how PIH has grown, innovated, and pushed the boundaries of global health to ensure that every single person has access to high-quality care.

1983
Paul Farmer and Ophelia Dahl begin operating a community clinic to provide free health care to the people of Cange, a small, rural village in Haiti.

1987
Dr. Paul Farmer, Ophelia Dahl, Dr. Jim Kim, Todd McCormack, and Thomas J. White found Partners In Health to support work providing health care to poor patients in Haiti.
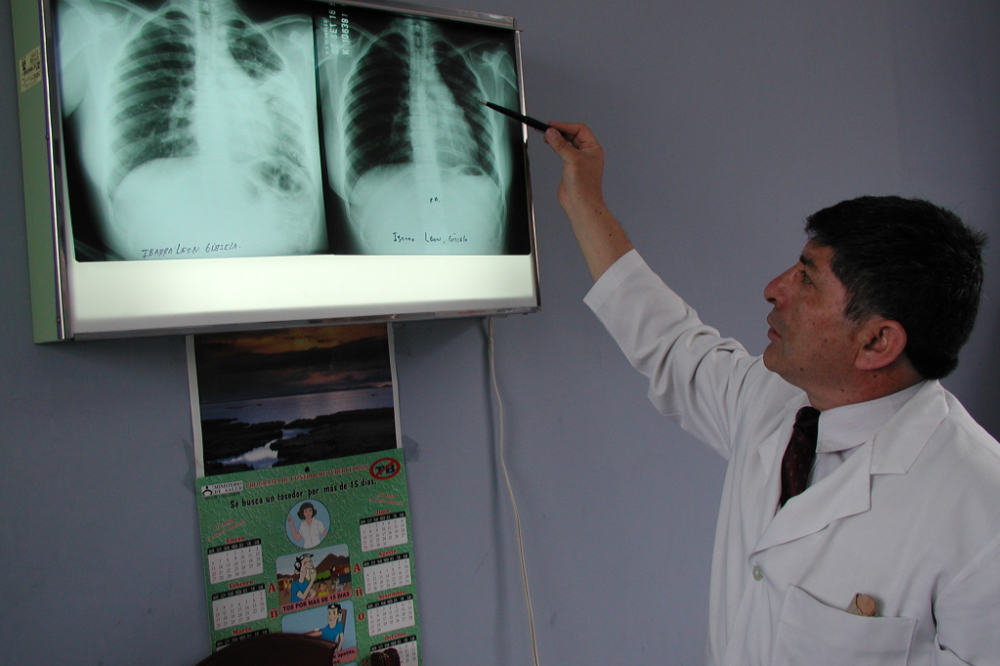
1994
PIH expands to Peru and begins supporting the government in battling an unchecked epidemic of multidrug-resistant tuberculosis. Our community-based MDR-TB treatment program sees an 80 percent cure rate, inspiring the World Health Organization to revise its treatment recommendations.

1998
PIH launches the HIV Equity Initiative, which provides antiretroviral therapy to HIV-positive patients in Haiti. Our example helps later inspire major organizations like the Global Fund, PEPFAR, and the World Health Organization to fund the fight against HIV in rich and poor countries alike.

1998
PIH expands to Russia and begins supporting the government in fighting tuberculosis and multidrug-resistant tuberculosis epidemics, first in prisons and then throughout the community of Tomsk.

2003
Tracy Kidder publishes Mountains Beyond Mountains, a book tracing the lives of PIH founders and our work in Haiti, Peru, and Russia.

2004
PIH co-founds OpenMRS, an open source electronic medical records software tailored for use in developing countries. Today, organizations and governments in 64 countries use OpenMRS.
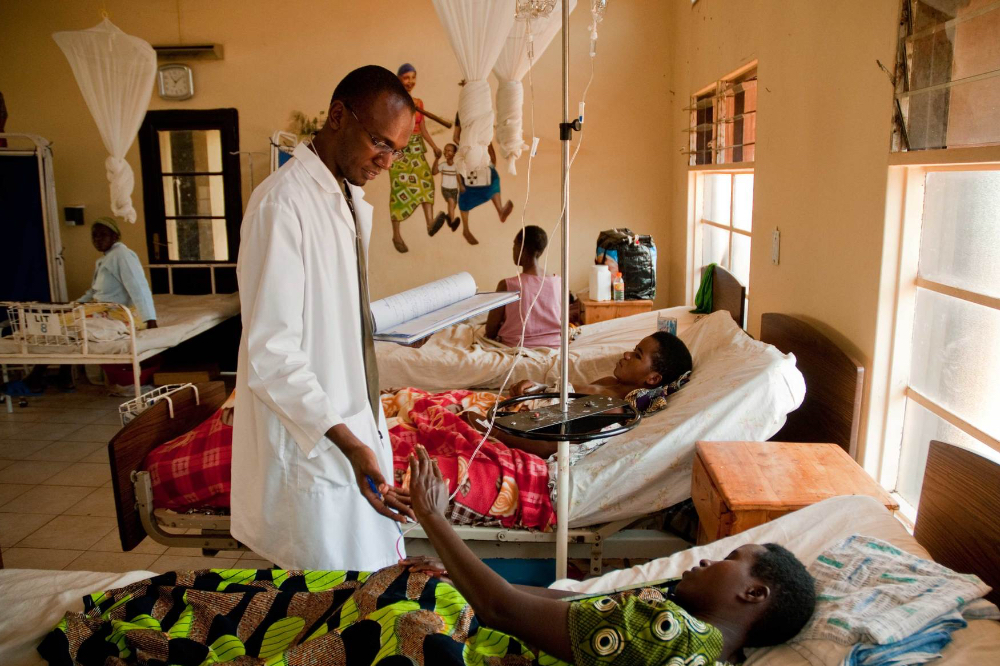
2005
PIH expands to Rwanda and partners with the government to bring high-quality health care to three of the country’s poorest regions. This includes oncology care at the Butaro Cancer Center of Excellence, which we open in 2012 to provide accessible, lifesaving cancer treatment to patients from Rwanda and east Africa.
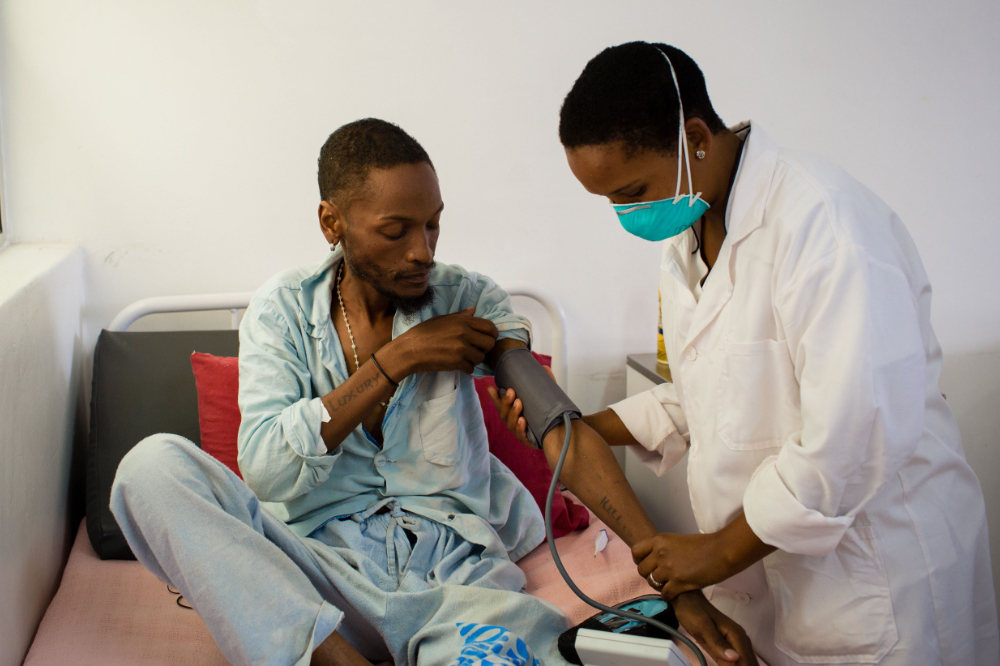
2006
PIH expands to Lesotho and begins supporting the government’s response to the HIV epidemic. We soon broaden our scope to treat tuberculosis, improve maternal health care, and, in 2014, become the government’s primary technical advisor on its National Health Reform, which is bringing the country closer to universal health coverage.

2007
PIH expands to Malawi and begins collaborating with the government to provide comprehensive primary care to the rural poor. We build a brand new community hospital and two health centers that offer same-day consultation and care—including maternal health care and treatment for HIV, hypertension, malnutrition, and mental illness.

2009
PIH expands to the Navajo Nation and establishes local partnerships to help improve community health and support community health representatives. In 2015, we help launch the Fruits and Vegetables Prescription program, which provides families—most of whom live a three-plus-hour drive away from a grocery store—free access to fresh, local produce.

2010
PIH expands to Kazakhstan to support the government’s fight against multidrug-resistant tuberculosis.

2010
When a catastrophic 7.0-magnitude earthquake strikes Haiti, PIH provides lifesaving health care and social support to earthquake survivors.

2010
Our global mental health care program launches, providing high-quality, culturally sound treatment for common and severe mental illnesses, from depression to schizophrenia.

2011
PIH expands to Mexico and begins collaborating with the government to help train new doctors, revitalize rural clinics, and maintain a force of community health workers, who specialize in areas like maternal health, depression, and diabetes.
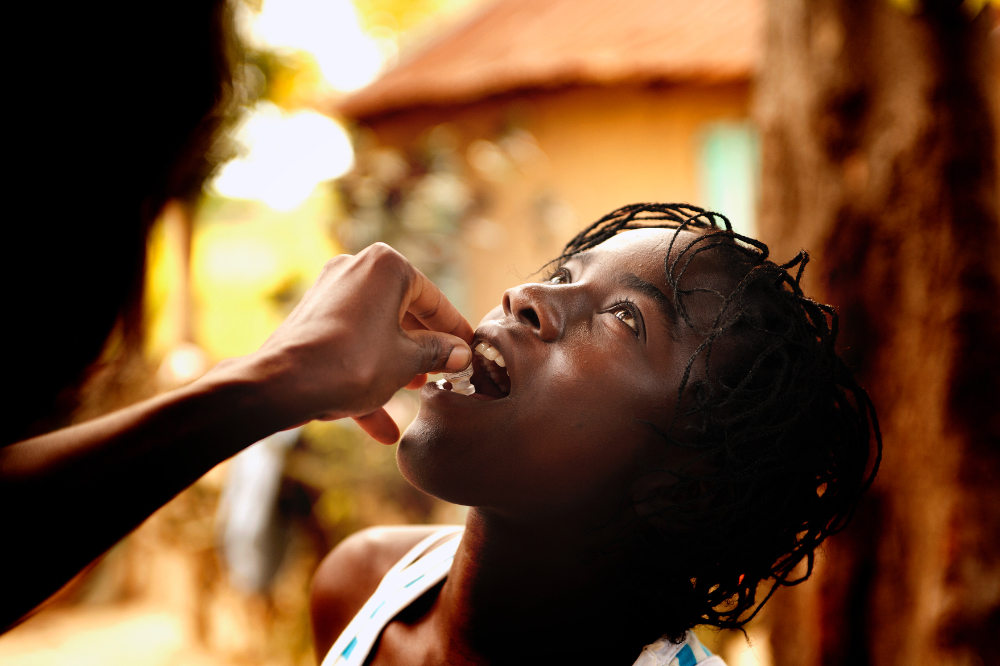
2012
After cholera is introduced to Haiti following the 2010 earthquake, PIH conducts a cholera vaccination campaign that protects 50,000 people against the deadly disease. The campaign’s success inspires the World Health Organization to establish a global stockpile of oral cholera vaccine.

2013
PIH opens University Hospital in Mirebalais, Haiti, a 300-bed teaching hospital that provides advanced, high-quality care and offers specialized residency programs to train the next generation of clinicians.

2014
Responding to history’s largest Ebola outbreak, PIH expands to Sierra Leone and Liberia to help end the epidemic and to support the government in strengthening the countries’ weak health systems.
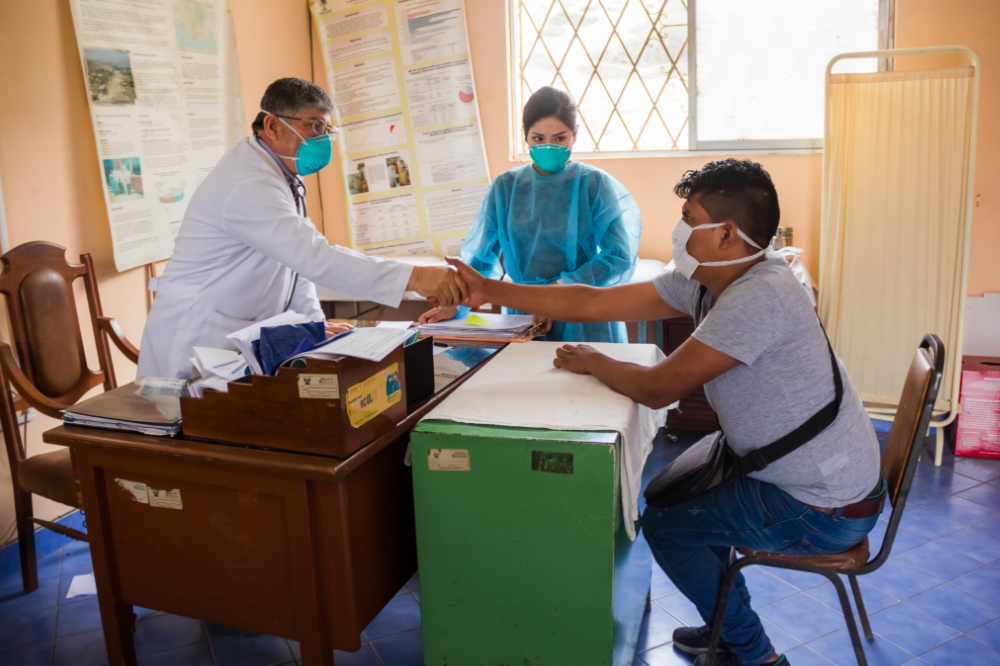
2015
PIH begins leading a partnership called endTB, which expands global access to new treatments for multidrug-resistant tuberculosis and conducts clinical trials to find shorter, less toxic, more effective drug regimens across multiple countries.

2018
The first cohort of PIH global nurse leaders completes our inaugural Nightingale Fellowship, a program designed for nurse leaders to make system-wide impacts to improve patient care.

2019
In Rwanda, PIH inaugurates the permanent campus of the University of Global Health Equity, which we founded in 2015. The university trains new generations of global health leaders by offering a graduate degree in global health delivery and, beginning this year, dual degrees in medicine and surgery to students from around the world.

2020
PIH launches the Community Tracing Collaborative—in partnership with the Commonwealth of Massachusetts and local boards of health—to accelerate the effort to contain the statewide spread of COVID-19.
2020
When COVID-19 spreads globally, PIH initiates a comprehensive response across countries and launches the U.S. Public Health Accompaniment Unit (USPHAU) to support some of the hardest-hit communities in the United States.
2021
In October, PIH announces that USPHAU will officially become our United States arm, PIH-US, which focuses on building more robust and equitable community health and social support systems across the country.
2021
The endTB project, led by PIH and partners, meets its goal of enrolling 750 patients across four continents in a clinical trial to find safer, shorter, and more effective treatments for multidrug-resistant tuberculosis. The results will be available in 2023.
2021
Several countries where PIH works celebrate long-term anniversaries: 10 years for PIH Canada, 10 years for Compañeros En Salud in Mexico, and 25 years for Socios En Salud in Peru.

2022
Paul Farmer, PIH's co-founder, unexpectedly passed away in Rwanda from an acute cardiac event on February 21.



