Q&A: Combating Sierra Leone’s Maternal Health Crisis Through COVID-19
Posted on May 5, 2020
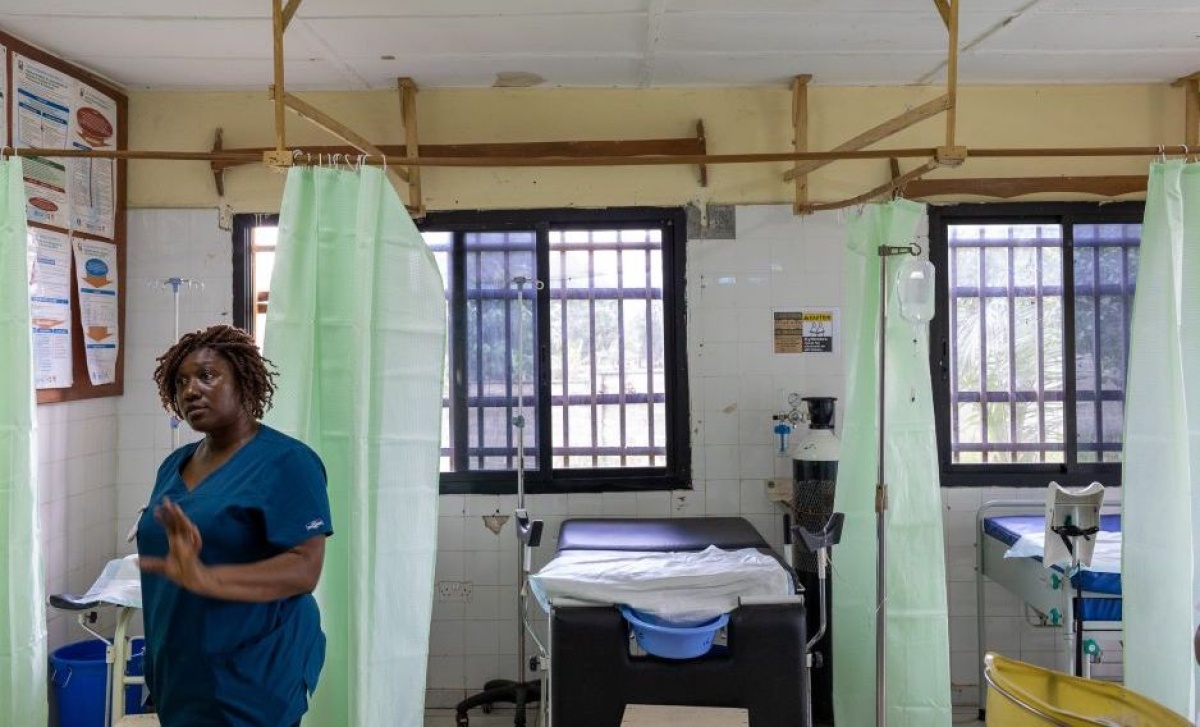
As the novel coronavirus continues to spread, patients aren’t just at risk of contracting its resulting illness, COVID-19. They also face higher risk for all other health issues, as many facilities must divert resources from routine medicine to emergency care. What’s more, COVID-19 is preventing families from seeking the care they need. Fear of the virus is spreading alongside the virus itself—and could prove just as deadly.
Expectant mothers across the globe find themselves uniquely impacted by these new barriers to health care. Nowhere in the world is the situation more acute than in Sierra Leone, where a woman’s lifetime risk of dying in pregnancy or childbirth is already 1 in 17 during non-pandemic times—the world’s worst maternal mortality rate.
Isata Dumbuya, a nurse midwife and manager of reproductive, maternal, neonatal, and child health for Partners In Health in Sierra Leone, has been working to combat these barriers in the maternity wards at PIH-supported Wellbody Clinic and Koidu Government Hospital in Kono District. Last year, the facilities provided more than 2,200 safe deliveries—a number that rises annually.

COVID-19 case numbers are also rising. PIH has been preparing Kono for a possible outbreak, as well as assisting the government with national response efforts, as the number of known cases increases past 200 in the country of seven million people.
“What we don’t want,” Dumbuya said, “is fear of COVID preventing women from coming into the hospital to access normal services that would improve their health and prevent them from having other morbidities that have nothing to do with COVID.”
We caught up with Dumbuya to hear more about the intersection of a longstanding epidemic—maternal mortality—and the new pandemic of COVID-19, and the measures PIH is taking to fight even harder to protect women and infants in Sierra Leone.
What impact has the coronavirus pandemic had on maternal health at Wellbody Clinic and at Koidu Government Hospital?
Dumbuya: Like most of the departments in the hospital, we did see a reduction in the number of women who came in, primarily for prenatal care. They are probably thinking, "This is not an emergency. I'm well, and I would rather save myself a journey into the hospital." Because there was a lot of uncertainty and fear around coronavirus, there was a common misconception in communities: "Don't go to the hospital." Women who might want to come for prenatal checks were being told, "Don't come."
We also saw, in the initial periods at least, that women who did come into the labor ward were much further along in their labor than we would like, so we didn't have a lot of time to monitor them or put interventions in place to have a better outcome. Women come in late most of the time, but this was just getting to later, critical stages, and there were fewer of them. For the first couple of weeks, almost every woman who came in ended up with a cesarean section.
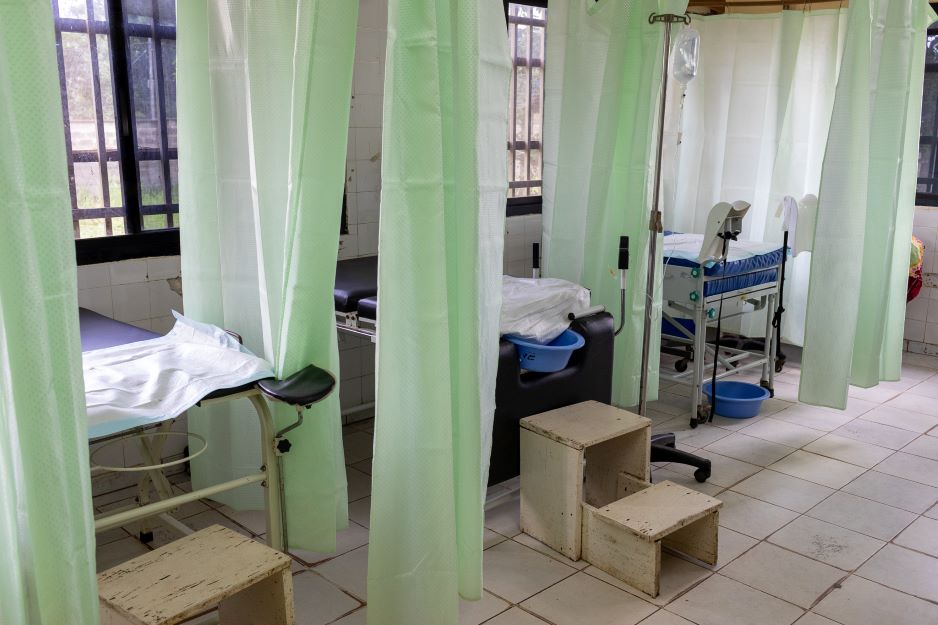
And were fewer patients arriving for care generally at the hospital?
Before, you would come into Koidu Government Hospital and there's usually a crowd of people. Some are patients, some are waiting, some have accompanied patients. That stopped. The few that had to come in were the ones that had no choice. And when they came in, they came in with one person. Usually the average rate of accompaniment is three people per patient. They were coming in with one person at a time and trying to get out as soon as they possibly could.
That was the same during Ebola, too. Most people in Sierra Leone never had Ebola, but were dying from malaria, tuberculosis, HIV, car accidents—everything that was affecting people before Ebola.
But it's getting better. We're getting more women to come in. We’re almost back to normal. In the prenatal clinics, especially at Wellbody, the numbers have started to increase. It's good to see that they're willing to come back. Patients are walking back in and seeking care, which is one of the things that we feared the most, one of fallouts: "These people are not gonna come to the hospital, and when they do come, they're gonna be critically sick, and we're gonna have more and more poor outcomes."
Before coronavirus, you were going out to the different chiefdoms around Kono District to educate community leaders and families about the services available at KGH and Wellbody. Have you been doing any outreach since the coronavirus pandemic started?
I was really lucky to be part of the engagements with community health workers and other community stakeholders, explaining step-by-step what coronavirus is, the impact that it's having all over the world, how we are preparing to minimize the potential for us experiencing the same level of infection and death. And also just trying to get people to understand that the hospital is still open. Having that interaction, it allayed a lot of the people's fears. It generated a lot of questions. They seemed to understand a lot more about COVID by the time we were done and were willing to take the message forward and say, "Now we know, we are also less fearful, and we will let our people know and encourage them, 'You have to come to the hospital.'"
Maternal mortality in Sierra Leone has been an emergency for decades for women and children. What would you say to those who may be worried about COVID-19’s impact on plans and strategies to radically reduce maternal mortality?
With COVID, yes, this is the foremost thing, not just in Sierra Leone, but in the whole world at the moment. But there will be life after COVID. Maternal mortality in Sierra Leone still continues to deteriorate despite COVID, until we get more and more structured systems in place.
We're still pushing forward and realigning our plans with COVID. We're getting more and more ideas about things that we perhaps hadn't thought about or hadn't put very high on the list. We need more isolation units. We need more staff trained in high-dependency care. We're going to need more equipment, so that in the future, whether it's COVID or anything similar, we need to build in more critical care intervention for pregnant women.

One of the biggest differences between coronavirus and Ebola times is that health care in Kono has come such a long way; patients will still have access to the care they need in a way they didn’t during Ebola. What are some of the standout improvements you've seen in the maternity wards and in reproductive and maternal and child health care in Kono since you arrived?
There's so much. I remember when I first started here in 2018—the difference from then to now with staff motivation. We've had a few new staff, but most of them I met when I started. They now come to work because they really want to. They come in determined to do a great job and to enjoy doing their job.
We recently did a weeklong training, because we're opening up a high-dependency unit in maternity. This is also something new. We are able to look after critically ill women in a dedicated space—with staff that are now happy to come to the training. There’s a higher level of motivation, of pride that they take in their work, and of interest.
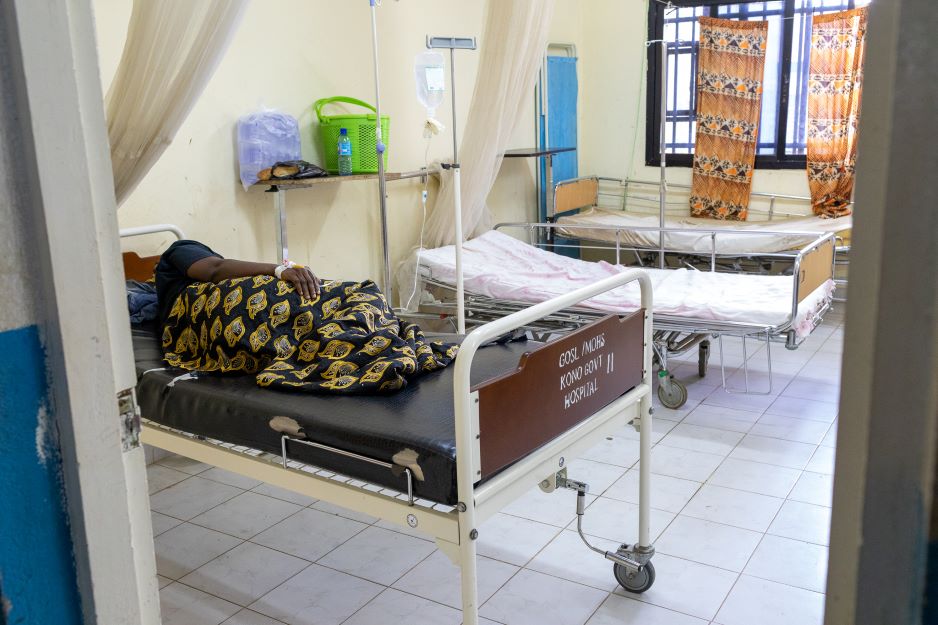
That transformation makes sense—going from having no resources and not being able to intervene to save a woman’s life to having resources, training, supplies, electricity, and a blood bank.
Women should not die in pregnancy. She should not die when she comes to give birth. This is not something that we should just take lightly anymore. This is something that we should do everything, with the resources, knowledge, finances that we have, to prevent from happening.
What's keeping you motivated and energized during this moment?
Every day I come in to work determined to support the staff I'm working with, both PIH staff and the Ministry of Health, to do the best they can in terms of patient care to help women and babies. The care that we give is intended to not just save lives, but also to improve their whole reproductive journey, to make it special and different from anything they've ever experienced.


